Varicoceles are swollen veins in your scrotum. They usually cause mild symptoms, including scrotal swelling or aching pain in your testicle. They may not cause any symptoms at all. However, they’re a common cause of infertility. A healthcare provider can diagnose a varicocele and recommend the proper treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
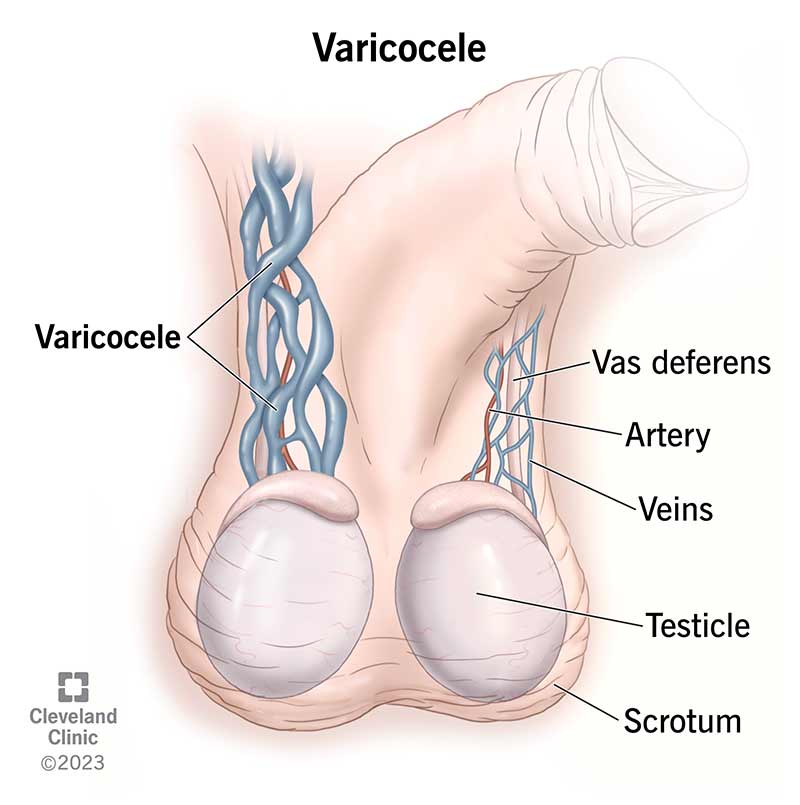
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15239-varicocele)
A varicocele (VAIR-ick-oh-seal) is a common disorder that enlarges the veins in your scrotum. Your scrotum is the pouch of skin behind your penis that typically contains your testes (testicles). Varicoceles are similar to varicose veins. Varicose veins cause veins in your legs to swell and lose their shape.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Varicoceles are usually painless but can sometimes cause testicular pain, which may come and go. In some people, a varicocele may cause infertility. If a varicocele doesn’t bother you, you may not need treatment.
Varicoceles aren’t life-threatening. However, a varicocele can be very serious if you’re trying to have a biological child.
Yes, varicoceles can affect fertility. Varicoceles can contribute to about 40% of all cases of male infertility. However, many people with varicoceles have no problems achieving pregnancy.
Medical experts don’t understand what role varicoceles play in infertility. It’s possible that the temperature inside your scrotum increases due to the buildup of blood in the veins. The higher temperature affecting both testicles may affect sperm count or production.
Talk to a healthcare provider if you suspect you have infertility. Fertility concerns are the top reason why people receive varicocele treatment.
Varicoceles affect 15% to 20% of all men in the United States — about 1 in 5. A varicocele is more likely to occur on the left side of your scrotum because of differences in how blood drains from your left testicle back into the major veins of the body. Less commonly, it can affect the right side or both sides.
Advertisement
Varicoceles usually don’t have any symptoms. However, you may notice:
Larger varicoceles may feel or look like a bag of worms or spaghetti. They may cause mild discomfort, aches or pains. Smaller varicoceles may be too small to see or feel.
Healthcare providers and medical experts aren’t sure what causes varicoceles to develop. Some think that a faulty “switch” (valve) inside certain veins in the spermatic cord may cause them. The spermatic cord is a band of tissues that holds your testicles in place. These veins return blood from your testicles to your body. The valve acts as a sort of “on/off” switch. It has two flap-like structures that help blood move back toward your heart. When a valve doesn’t work the way it should, blood may build up inside the veins in your testicles. Over time, the veins swell.
Varicoceles can affect anyone with testicles at any age. Healthcare providers believe that many varicoceles are present at birth (congenital). People often notice a varicocele during their teenage years. Medical experts suspect this may have to do with puberty, when blood flow to your genitals increases. In some cases, the varicocele can prevent your testicle from growing properly.
There isn’t enough research to definitively say that varicoceles cause erectile dysfunction (ED), but there may be a link. Some studies show that people who receive varicocele treatment may still sometimes fail to achieve an erection, but not as often.
Larger varicoceles may increase your risk of other complications, including:
A healthcare provider can diagnose a varicocele. They’ll review your medical history, ask questions about your symptoms and perform a physical examination.
During the physical exam, your provider may ask you to stand up, take a deep breath, hold your nose and mouth closed and strain to push air out. This is the Valsalva maneuver. They’ll feel your scrotum for enlarged veins as you’re holding your breath and straining.
Advertisement
They may also order the following tests to confirm their diagnosis:
After confirming the presence of a varicocele, your provider will grade its severity.
Healthcare providers use grades to detect and score varicoceles:
Advertisement
Varicocele treatment depends on the severity of your varicocele. For low-grade varicoceles, a healthcare provider may recommend at-home treatment options, including:
A varicocelectomy is a surgical procedure that treats severe varicoceles that are painful or affect your fertility. A surgeon who specializes in conditions that affect your urinary system and reproductive system will cut your affected veins and seal off the ends. This redirects blood flow to other healthy veins in your scrotum.
Advertisement
Most people make a full recovery after a varicocelectomy within six weeks.
It depends on the varicocele grade. Your healthcare provider may not recommend treatment if you have a small varicocele that doesn’t bother you or cause fertility issues.
If you have a higher-grade varicocele and don’t get treatment, it can permanently damage your testicles.
Many people with varicoceles have no symptoms at all. Some people may experience mild discomfort during certain activities, but the varicoceles won’t cause serious or long-term health problems.
Some people who have varicoceles have fertility issues. If you have concerns about your ability to have a biological child, talk to a healthcare provider. They’ll help you understand your options.
Medical experts aren’t sure what causes varicoceles to develop. As a result, they’re not sure how you can prevent them.
Talk to a healthcare provider if you have varicocele symptoms, including an inability to get your partner pregnant. They can diagnose a varicocele and recommend the best treatment for you.
If you receive treatment for a varicocele, schedule follow-up appointments with your provider. They’ll monitor your health and may order additional tests to make sure your treatment is effective.
A varicocele is an enlarged vein in your scrotum. A hydrocele is a fluid-filled sac surrounding a testicle in your scrotum. It commonly affects newborn boys when the thin membrane tunnel (processus vaginalis) fails to close after the testicles descend during fetal development.
A varicocele is a common condition that can affect males at different ages and stages of life. Most people experience mild or no symptoms. Deciding whether to treat a varicocele is up to you. Wearing supportive underwear or a jockstrap or taking over-the-counter pain medication may be enough to relieve minor symptoms. However, varicoceles can cause infertility. A varicocelectomy can repair a varicocele and sometimes improve your fertility. Talk to a healthcare provider about your treatment options, including how surgery may affect your fertility.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a condition that’s affecting your urinary system, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
