Corneal disease is a group of conditions that affect your cornea (the clear window at the front of your eye). Common types include keratitis, corneal dystrophy and corneal ectasia. Causes range from genetic mutations to eye injuries. Symptoms depend on the specific condition and can include eye pain, blurry vision and sensitivity to light.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
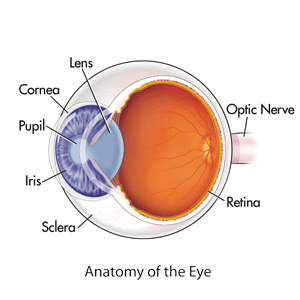
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/8567-2077.ashx?la=en&hash=4F52B223DF299E4E5277B4B616A7AB0ED86755D5)
The term “corneal disease” refers to a variety of conditions that affect your cornea. Your cornea is the transparent window on the front of your eye that serves as a barrier against dirt and particles. It also plays a key role in your vision. Corneal diseases can interfere with these functions and may cause pain or other symptoms in your daily life. However, some corneal diseases cause few or no symptoms but still need treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
If you have symptoms of corneal disease, including pain, blurry vision or sensitivity to light, see an eye care specialist right away. It’s also important to have eye exams on a regular basis, even if your eyes seem fine. An eye care specialist can tell you how often you should have exams based on your age, medical history and other factors. Your ophthalmologist will diagnose and treat corneal diseases and other eye problems to help you see clearly for many years to come.
Many of the diseases that can affect your cornea fall into three main categories:
Advertisement
Other conditions that may cause symptoms or damage your cornea include:
Symptoms vary based on the specific condition and may include:
These symptoms can point to many possible conditions. And some conditions have no symptoms, especially early on. That’s why it’s important to see an eye care specialist if you experience these issues.
Several things may cause corneal diseases, including:
You may face a higher risk of certain corneal diseases if you:
Eye care specialists diagnose corneal diseases through a comprehensive eye exam. They’ll perform many standard tests, including a slit lamp exam, to check the health of your cornea and other parts of your eye.
Your provider may also perform a fluorescein eye stain test. This involves putting a small amount of harmless dye into your eye and then shining a light on your eye. The dye makes any scratches or damage to your cornea visible to your provider.
Your provider will tell you if they notice any problems and discuss next steps, including referrals for treatment.
Advertisement
Treatment options vary widely based on your condition and can include:
Your eye care specialist will explain which treatment options are appropriate for you, and they’ll tailor a treatment plan to fit your needs.
Early diagnosis and treatment can help you manage your condition. Without treatment, some corneal diseases can lead to severe vision loss. That’s why it’s important to see an eye care specialist for regular checkups and tell them if you have any new or changing symptoms. They’ll tell you what you can expect in your individual situation.
It’s not always possible to prevent corneal disease, especially since some types are genetic. But you can lower your risk of certain corneal diseases. Here are some steps you can take:
Advertisement
Tell your provider if anyone in your biological family has corneal disease. This information can help your provider screen for and monitor certain conditions.
Regular eye exams are vital for your eye health. An eye care specialist can tell you how often you should have one. Most adults need an eye exam every one to two years. You may need more frequent exams if you have certain conditions or risk factors.
Seek medical care immediately if:
You can learn more about corneal disease (and its potential impact on you) by asking an eye care specialist:
Corneal disease is an umbrella term that describes a range of conditions affecting your cornea. While some conditions can sound scary, it’s important to remember that a wide range of treatments are available to help protect your vision and restore your eye health. Talk to an eye care specialist about what you can expect going forward.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s ophthalmologists and optometrists have the highest training available. We provide exams, vision correction and care for many eye conditions.
