Cornea transplant, also called corneal grafting, replaces a damaged cornea with tissue from a deceased donor. A cornea transplant can treat conditions such as Fuchs’ dystrophy and keratoconus. Most people have improved vision and less pain.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
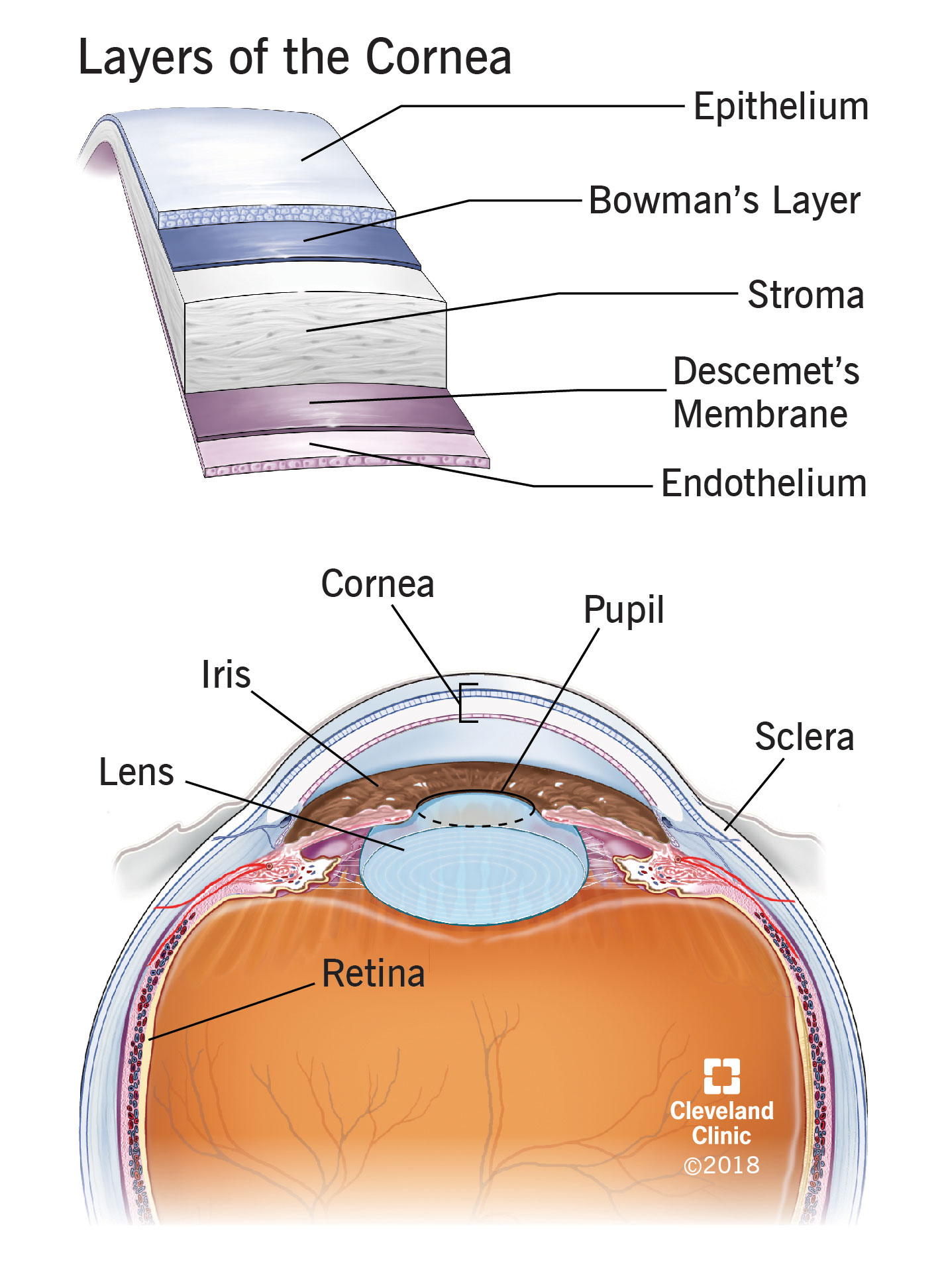
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17714-cornea-transplant)
Cornea transplant (corneal transplant) is surgery to replace your cornea, the clear front layer of your eye. Corneal grafting and keratoplasty are other terms for cornea transplant.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your eye care provider may recommend you consider a cornea transplant if you’ve damaged your cornea. Cornea damage causes eye pain, cloudy and blurred vision.
In a cornea transplant, your surgeon removes your damaged cornea and replaces it with donated healthy corneal tissue. For many people, cornea transplant surgery restores vision and improves their quality of life.
Your eye care provider may suggest a cornea transplant if you have:
There are about 185,000 cornea transplant surgeries performed every year throughout the world. In the U.S., ophthalmologists perform more than 47,000 corneal transplants annually. The top three countries for these procedures are:
People living in more than half of the countries in the world don’t have access to this surgery. One reason for this is the lack of donated corneas. There’s only one cornea available for every 70 individuals in need.
There are three surgical options for cornea transplant: penetrating keratoplasty, deep anterior lamellar keratoplasty and endothelial keratoplasty. Your cornea has three layers of tissue. Each of these surgeries targets a specific layer or layers of tissue.
Advertisement
All corneal transplants use corneas from deceased human organ donors. Every donor cornea undergoes thorough testing to make sure it’s safe for transplant.
Another term for penetrating keratoplasty is full-thickness cornea transplantation. Developed over 100 years ago, the modern version of this surgery continues to help thousands of people each year. In this procedure, your surgeon uses a small circular blade to remove the entire center part of the damaged cornea and replaces it with a healthy, same-shaped piece of donor cornea.
If the innermost layer of your cornea is healthy and the damage lies in the middle and outer layers, your surgeon may perform a partial thickness cornea transplant. Another term for this is a deep anterior lamellar keratoplasty. During this surgery, your surgeon removes the middle and outer layers of your cornea and replaces them with healthy donated corneal tissue.
This surgery may help if you have damage on the innermost layer of your cornea, the endothelium, which rests on Descemet’s membrane. Surgeons perform two types of endothelial keratoplasty surgeries:
Both surgeries involve removing damaged endothelial tissue and replacing it with healthy donor tissue. The difference between DSAEK and DMEK is the thickness of the donor cornea — DSAEK is thicker, while DMEK is thinner. You and your surgeon will decide which type of transplant is best for your specific eye condition.
Endothelial keratoplasty procedures require fewer sutures than other keratoplasty procedures. Instead, the technique uses an air bubble to keep the donor cornea in position. To increase the chance of success, you’ll need to make sure you’re lying face up when you rest or sleep for the first few days after surgery. Lying face up helps the air bubble keep your transplanted corneal tissue in place.
Your surgeon and the anesthesia team will review your medical history, answer your questions and confirm the surgical plan. They’ll let you know if you need to stop taking any medications or over-the-counter (OTC) products before your surgery. They’ll also tell you when to stop eating and drinking before the surgery. You’ll need transportation home after surgery since you won’t be able to drive.
The anesthesia team will administer either sedation or general anesthesia (making you unconscious), depending on your medical condition and what you and your healthcare provider have discussed. A caregiver will apply numbing medication to your eye.
Advertisement
The surgery typically takes less than two hours to perform.
You’ll need a driver to take you home after you leave the recovery unit. You may want someone to spend the evening with you. You’ll need to wear an eye patch when you leave.
Advertisement
Most people who have a cornea transplant see more clearly. In rare circumstances, you may have a cornea transplant to reduce eye pain.
A cornea transplant is generally a very safe surgery. Your surgical team will make every effort to reduce your risk of complications.
One of the most concerning complications of cornea transplant is organ (cornea) rejection. Rejection means your body’s immune system identifies the donated cornea as foreign and tries to fight off the transplant. Risk of rejection varies based on the surgical technique used and on the condition of your eye.
In some cases, your surgeon may recommend against surgery because your eye is likely to reject a transplanted cornea. Conditions like severe dry eye, blood vessels growing in the cornea and eye infections increase the chance of rejection.
If you have a cornea transplant, you’ll need to use eye drops for at least a year following surgery to reduce the risk of rejection.
Other complications of cornea transplant surgery include:
Advertisement
The degree of long-term success depends on a number of factors, including:
Because success varies, you should ask your surgeon what you might expect given your particular situation, including your eye health.
Keep in mind that you’ll probably have blurred vision after surgery that will gradually improve over time. Several factors affect how long it’ll take for the vision in your eye to return to normal.
For example, if you had a full-thickness transplant, it may take up to 12 months for you to have full vision. But if you had an endothelial transplant (DMEK or DSAEK), you may achieve good vision within three months.
You can’t drive on the day of your cornea transplant. Someone needs to drive you home after surgery and bring you back for your follow-up visit.
If you have good vision in the non-transplant eye, you can legally drive 24 hours after surgery. However, your surgeon may recommend waiting longer before driving, especially if you had an endothelial transplant.
It may take a few days to a few weeks before you can return to work. It depends on your level of discomfort, your vision and what activities you perform at work. If your job involves strenuous activities like lifting heavy objects, you may need to take additional time away from work.
Contact your surgeon immediately if you experience any signs of cornea rejection, including:
Contact your surgeon if you notice any other problems in your vision after cornea transplant, or you experience symptoms of infection, such as fever or eye drainage.
The key to avoiding a cornea transplant is to prevent damage or injury to your cornea. There are things you can do to protect your eyes, including:
You may need to wear glasses or contact lenses after a cornea transplant. A full-thickness cornea transplant surgery often leaves an irregular cornea surface. This imperfection in the curve of the cornea, called astigmatism, results in distorted vision, so you may need corrective lenses or even additional surgery.
You won’t typically need special types of contact lenses after endothelial transplants, like rigid gas permeable or scleral lenses (a larger lens that tops the white part of the eye). But you may need them after penetrating keratoplasty or deep anterior lamellar keratoplasty surgery. Your surgeon will talk with you to find the best options to meet your vision needs.
You may have a different type of surgery that’ll give you an artificial cornea (keratoprosthesis). You may need one of these if your body rejects the transplants.
Cornea transplant surgeries improve vision and reduce pain for many people. Probably any type of eye surgery seems intimidating, but the results are usually very good. Talk with your eye care provider about your cornea condition and if you’re able to have transplant surgery. If you do have a transplant, keep in contact with your provider. Keep your scheduled appointments and let your provider know about any issues with your vision. Your healthcare team is dedicated to keeping you healthy.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s ophthalmologists and optometrists have the highest training available. We provide exams, vision correction and care for many eye conditions.
