Pterygium (surfer’s eye) is a raised, fleshy, triangular-shaped growth that starts in the corner of your eye. Long-term exposure to UV light is the main cause. It may not cause symptoms, but sometimes, it can irritate your eye, and if it grows too much, it can affect your vision. Treatments include eye drops and surgery, if necessary.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
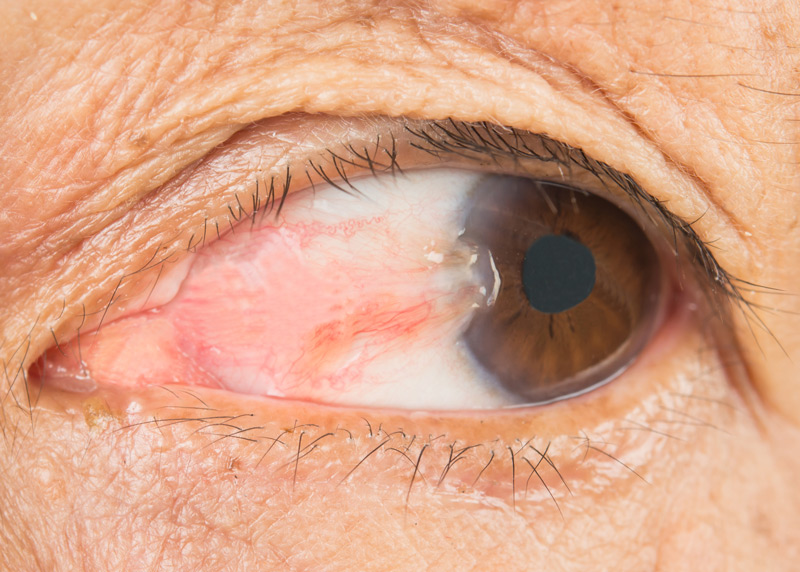
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/22497-pterygium)
A pterygium (ter-IJ-ee-um) is a raised, fleshy growth on your eye’s conjunctiva, the clear membrane that covers the white part of your eye. The growth may look whiteish or pinkish and may have visible blood vessels in it. It typically starts in the corner of your eye and grows toward your iris (the colored part).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Pterygium typically has a triangular or wing-like shape. The word, “pterygium,” comes from the Greek words pteryx, meaning “wing,” and pterygion, meaning “fin.” Another name for pterygium is surfer’s eye. This is because surfers are often in the elements that cause pterygium — sun, wind, sand and salt.
Surfers do get pterygia (the plural of pterygium) more often. But anyone can get one if they spend a lot of time outdoors without eye protection. It’s more common in older adults, who’ve had more exposure to the elements over time, and also in those who live near the equator, where sunlight is more intense.
A pterygium isn’t an invasive growth. It’s not cancerous, and it won’t spread to other nearby tissues. But it can continue to grow across the surface of your eye. If it reaches your cornea (the clear part that covers the colored part), it can damage your vision. In this case, you might need surgery to remove it.
Pterygium is an overgrowth of your conjunctiva tissue. Causes include:
Other possible risk factors include:
Advertisement
You might not feel your pterygium at first. You might only notice a raised, fleshy, wedge-shaped growth at the corner of your eye. When symptoms do develop, they can be mild to severe. They might include:
Over time, you might also notice:
Not everyone develops these symptoms. Some pterygia grow more than others.
A pinguecula is a different kind of growth on your eye’s conjunctiva. It develops from similar causes — generally, long-term exposure to environmental irritants, especially sunlight. But pingueculae are much more common than pterygia. Sometimes, what starts as a pinguecula later develops into a pterygium.
Your eye care provider can diagnose a pterygium with a slit lamp exam. A slit lamp is a type of microscope that focuses a narrow line (slit) of bright light on your eye. It helps your provider look at the front and inside of your eye. This is part of a standard eye exam. They’ll recognize a pterygium on sight.
Pterygium treatment depends on how much it’s affecting you. If it’s not causing you any symptoms, it probably doesn’t need treatment. But your eye care provider will keep an eye on it. They’ll schedule regular eye exams to check on how the pterygium is growing and whether it’s affecting your vision.
If the pterygium irritates your eye, your provider might prescribe:
Providers also recommend wearing hats and wraparound UV sunglasses to protect your eyes from further UV damage. This may help slow the growth of your pterygium or prevent it from growing faster. If your pterygium is growing toward your cornea, they’ll recommend removing it before it gets there.
The only way to get rid of a pterygium is with eye surgery. A pterygium won’t go away on its own. You may want to have your pterygium removed if it seriously irritates your eye, if it’s growing aggressively or if it’s already affecting your vision. You may also choose to have it removed for cosmetic reasons.
Advertisement
An ophthalmologist can remove your pterygium. If you don’t have one, your optometrist can refer you.
During pterygium surgery, your ophthalmologist will:
Surgeons use different methods for patching the hole left after they remove your pterygium.
Options include:
Pterygium surgery takes about an hour. After surgery, you’ll wear an eye patch for a few days while you recover. It takes four to six weeks for your eye to heal completely.
Your provider will prescribe medications to take home with you, including antibiotics to prevent infection and steroid eye drops to prevent the pterygium from growing back.
Advertisement
The primary risk is recurrence (return of the pterygium after surgery). If this happens, you may need another surgery. Fortunately, with new and improved surgical techniques, rates of pterygium recurrence are declining. Current research suggests the rate of recurrence is somewhere between 2% and 15%.
Recurrence is more likely to occur if you don’t take your prescribed eyedrops as directed, or if your eye has direct sun exposure after surgery. It’s important to follow your provider’s instructions on this. You can still spend time outside, but if you do, make sure to wear protection, like a hat or sunglasses.
Some of the medications that providers prescribe to prevent recurrence can also have side effects. Antimetabolites like mitomycin can cause “melting” or thinning of your sclera (scleromalacia) after pterygium surgery. Steroid eye drops can raise your eye pressure or lead to cataracts forming.
Most pterygia will continue to grow, but some grow much more slowly than others. It’s possible that your pterygium will never bother you much. Because of the risk that it might grow back, healthcare providers don’t recommend surgery for a pterygium that’s small and doesn’t cause symptoms.
However, a pterygium that keeps spreading across your eye can cause problems. It may irritate your eye or obscure your vision. If it reaches your cornea, it can pull at it and change the shape, causing astigmatism. It can also scar your cornea, which can affect your vision even after it’s removed.
Advertisement
A pterygium won’t go away unless a surgeon removes it. It’s likely to grow slowly throughout your life. Most people won’t need treatment for a pterygium. If it irritates your eye, you can usually manage these symptoms with over-the-counter medications. If it’s more than a minor nuisance, you can remove it.
There’s a small chance your pterygium will come back after surgery. If it does, it usually starts to appear within four months, and no later than 12 months after surgery. If you need to have another surgery, your surgeon will take extra measures to make sure the pterygium doesn’t come back again.
You can lower your risk of developing a pterygium — and slow its growth if you have one — by protecting your eyes from the elements, especially sunlight. Wear UV protection sunglasses when you’re in the sun. Protect your eyes from dry, windy, dusty climates by lubricating them with artificial tears.
Your provider will want to see you regularly to check on your pterygium and measure its growth — usually about once a year, unless it grows faster or slower than normal. Make sure to see them sooner if you start to develop new symptoms, or if your current medications aren’t working for you anymore.
A pterygium can look alarming when it first appears, but it’s not especially serious. You may never need treatment for it. If it does cause symptoms, you can often treat them with over-the-counter medications or eye drops. Your provider will keep an eye on it and let you know if they recommend removing it.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s ophthalmologists and optometrists have the highest training available. We provide exams, vision correction and care for many eye conditions.
