Ramsay Hunt syndrome, or herpes zoster oticus, occurs when the varicella-zoster virus (shingles) reactivates and spreads to the facial nerves near your inner ear. The varicella-zoster virus is the same virus that causes chickenpox and shingles (herpes zoster). Treatment for the condition may include medications including antivirals and corticosteroids.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
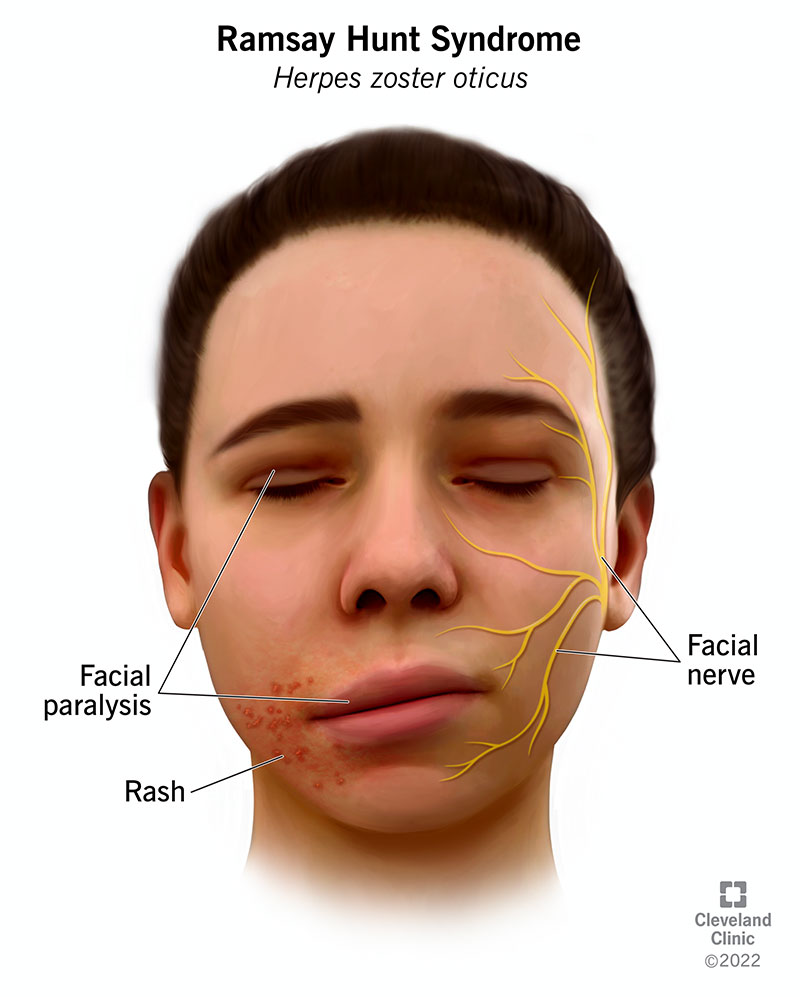
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/6093-ramsay-hunt-syndrome)
Ramsay Hunt syndrome is a complication of varicella-zoster virus infections, including chickenpox or shingles (herpes zoster). Other names for the condition include herpes zoster oticus and Ramsay Hunt syndrome type 2. It got its name when an American army officer and neurologist named James Ramsay Hunt first described the disorder in 1907.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
If you had chickenpox as a child, the virus that caused it (varicella-zoster virus) can remain inactive (dormant) in your nerves for years. Shingles occurs when the previously dormant varicella-zoster virus reactivates. The reactivation of the varicella-zoster virus in your facial nerve is called Ramsay Hunt syndrome.
Ramsay Hunt syndrome causes facial nerve paralysis (facial palsy) and intense ear pain. In addition, it may cause a painful rash on your ear, face or mouth.
Ramsay Hunt syndrome can affect anyone who’s had chickenpox or shingles. Most cases occur in people age 60 and older. The condition rarely affects children but has been diagnosed as young as three years old. People who are immunocompromised are more likely to be affected and generally experience more severe symptoms. They’re also less likely to have a complete recovery.
Ramsay Hunt syndrome affects about 5 out of every 100,000 people each year in the U.S.
However, some researchers think the condition is sometimes undiagnosed or misdiagnosed. This makes its true frequency more difficult to determine.
The disorder is the second most common cause of facial nerve paralysis, accounting for about 7% of all cases. Bell’s palsy is the most common cause of facial nerve paralysis.
Advertisement
Ramsay Hunt syndrome occurs when the varicella-zoster virus reactivates in the facial nerve, which is the cranial nerve that affects your face, tongue and inner ear. The varicella-zoster virus is the same virus that causes chickenpox and shingles.
If you had chickenpox as a child, the virus can remain inactive (dormant) in your nerves for years. Shingles occurs when the previously dormant varicella-zoster virus reactivates. The virus travels down your nerve fibers into your skin, causing painful sores. The virus sometimes develops into Ramsay Hunt syndrome, affecting your facial nerve. Researchers aren't sure why the virus sometimes involves the facial nerve.
Ramsay Hunt syndrome may cause weakness or stiffness on one side of your face, based on which branch of the facial nerve is affected. This may make it difficult to close your eye. It may also make it hard to wrinkle your forehead or make facial expressions such as smiles or frowns. It may also cause drooping and/or paralysis on one side of your face. This can cause slurred speech and it may make it difficult to eat.
Ramsay Hunt syndrome usually affects the nerves on only one side of your face. Therefore, you may experience symptoms only on that side of your face. Other Ramsay Hunt syndrome symptoms may include:
Ramsay Hunt syndrome may also cause vertigo. Vertigo is the false sensation that things around you are spinning or moving.
Ramsay Hunt syndrome isn’t contagious. But if you have the condition, it means you have the varicella-zoster virus. The virus can spread if someone comes in contact with the fluid from blisters that form in the affected person. It’s most likely to cause chickenpox in people who’ve never had the disease or gotten the chickenpox vaccine. Ramsay Hunt syndrome can cause serious health issues in people with compromised immune systems. It’s a good idea to avoid certain groups of people until your blisters scab over. These people include:
Advertisement
Your healthcare provider will perform a physical exam to diagnose Ramsay Hunt syndrome. They’ll ask you about your medical history and symptoms. Your provider will look for a rash and signs of weakness in your face.
Diagnosis can be difficult because the symptoms of the condition don’t always develop at the same time. Therefore, your provider may request a laboratory test to confirm the diagnosis. They may collect a sample of your saliva, blood or fluid from a blister. A pathologist will examine the sample under a microscope, looking for the varicella-zoster virus.
It isn’t necessary, but your provider may also request an imaging test called a magnetic resonance imaging (MRI) scan. This test can give your provider proof that another condition or disorder isn’t causing your symptoms.
Ramsay Hunt syndrome treatment may include various medications. Your healthcare provider may prescribe:
Advertisement
Natural treatment for Ramsay Hunt syndrome includes using a cold compress to reduce your pain. You may also consider wearing an eye patch. If you’re unable to close your eye, you risk damaging your cornea due to irritation. You may also want to use artificial tears or eye lubricants to prevent your eye from drying out.
If you have complete facial paralysis, your healthcare provider may perform a surgical procedure. The surgery can help relieve the pressure on your facial nerves.
Ramsay Hunt syndrome recovery time depends on the severity of your facial paralysis. If you don’t have much damage to your nerve and you’re otherwise healthy, your symptoms may improve within a few weeks to a few months. However, it may take up to a year to achieve a full recovery. If the damage to your facial nerve is more severe, your chances of a full recovery are less likely.
Antiviral medications can help, but your chances of a full recovery are better if you start treatment within three days of symptoms appearing. Early diagnosis and prompt treatment with antiviral therapy seem to improve long-term outcomes. About 70% of people with Ramsay Hunt syndrome will return to complete or almost complete facial function. However, even with prompt treatment, some cases result in permanent facial paralysis or hearing loss.
Advertisement
While very rare, Ramsay Hunt syndrome can come back just as a shingles infection can. That’s because the varicella-zoster virus remains present within your nerves forever.
Complications of Ramsay Hunt syndrome may include nerves that grow back incorrectly to the wrong structures in your face. This can cause abnormal reactions to certain movements. For instance, when you smile, it may cause your eye to close. Other complications of the condition may include:
If the virus reactivates in other nerves, such as those in your brain or spinal cord, you may experience other complications. These may include:
James Ramsay Hunt described at least three syndromes. Ramsay Hunt syndrome type 2 is the best known of these conditions. Although they share Ramsay Hunt’s name, types 1 and 3 are unrelated to type 2.
Ramsay Hunt syndrome type 1 is a rare neurological disorder. It causes seizures, tremors, loss of bodily function and cognitive impairment. Ramsay Hunt cerebellar syndrome is another name for the condition.
Ramsay Hunt syndrome type 3 is a type of neuropathy in the palm section of your ulnar nerve. Hunt's disease and artisan's palsy are other names for the condition.
Ramsay Hunt syndrome can occur as a complication of shingles. The condition can cause a painful rash, severe pain and facial paralysis. If you notice any of these symptoms, contact your healthcare provider right away. You’re more likely to make a full recovery with prompt diagnosis and treatment. You may also want to consider the shingles vaccine to prevent future outbreaks.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
