Esophageal perforation is a tear or hole in your esophageal wall. It’s usually an acute injury, but some slow-progressing conditions can also cause it. If a rupture occurs — no matter how small — it’s an emergency. Contents from your esophagus can escape through the hole into your chest and into your bloodstream, causing life-threatening complications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
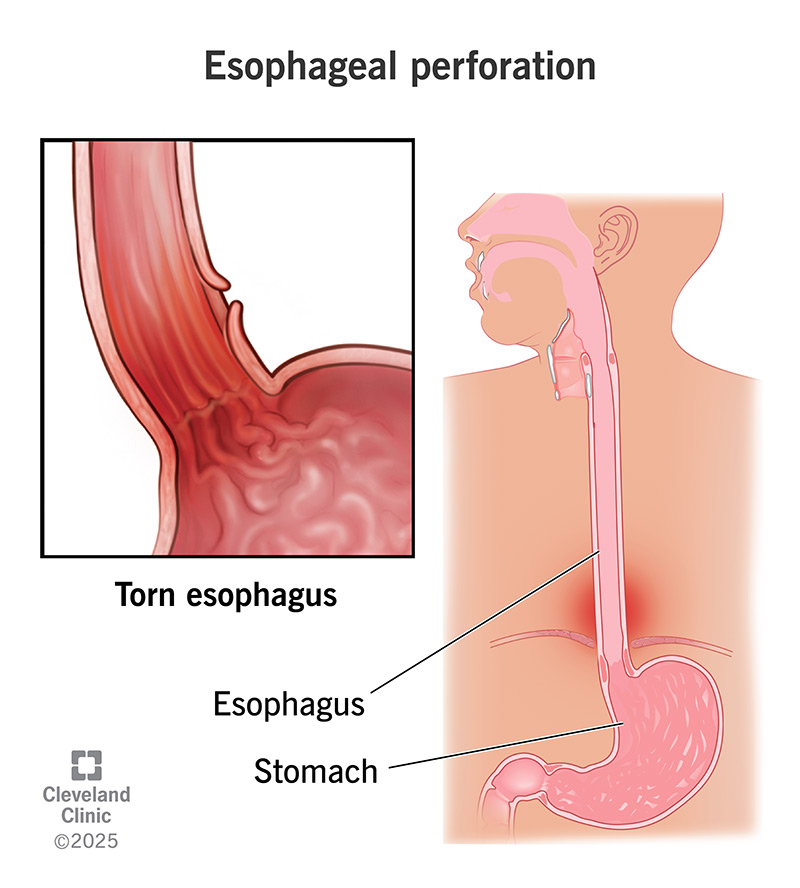
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/24284-esophageal-rupture.jpg)
Esophageal perforation is a rupture, tear or hole in your esophagus wall. It’s a medical emergency.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your esophagus is the swallowing tube that connects your mouth to your stomach, passing through your chest. It carries the food and liquids you ingest, along with bacteria and chemicals produced by your digestive system. These contents are safe in your esophagus, but harmful to other parts of your body.
If these contents escape through a hole in your esophagus, they can cause infection and inflammation in your neck, chest, abdomen or bloodstream. These conditions can quickly become life-threatening, so prompt treatment is essential. Ideally, a torn or ruptured esophagus should be treated within 24 hours.
Esophageal perforation is typically an acute injury, causing sudden, noticeable pain when it occurs. Most ruptures happen in your chest cavity, causing chest pain. If your rupture is higher or lower in your esophagus, you might feel pain in your neck or upper abdomen, or it might be referred to your shoulder. It might feel sharp, tearing, burning or penetrating. Other symptoms might include:
If you suspect you have a rupture, go to the ER right away. Severe pain and difficulty breathing or swallowing are emergency symptoms. Tell a healthcare provider about what was happening when they began. If they started after an injury or surgery, an episode of violent vomiting or swallowing something you shouldn’t have, an esophageal rupture is possible. Your provider will check for it.
Advertisement
All causes of esophageal perforation are rare. But among them, the most common cause is injury during a medical procedure on your esophagus. This is called iatrogenic injury, and it causes about half of all perforations. Examples of esophageal procedures include esophageal dilation to treat esophageal stricture, myotomy to treat esophageal dysmotility and Nissen fundoplication to treat GERD.
The second most common cause is a spontaneous rupture from tremendous stress within your esophagus. This is also called an effort rupture, or Boerhaave’s syndrome. It represents about 15% of all esophageal ruptures and affects about 0.0003% of the population. It usually happens during forceful and repeated vomiting. But excessive strain during weightlifting, seizure or childbirth can also cause it.
Other possible causes of esophageal rupture include:
Your esophagus is more prone to perforation than other gastrointestinal organs because it doesn’t have an outer layer (serosal layer) like others do. This makes the wall thinner and weaker to begin with.
Having certain esophageal disorders can also raise your risk of esophageal perforation. Your esophagus might be more likely to rupture if it’s already been injured or damaged by inflammation on the inside.
Some of these risk factors include:
A torn esophagus can lead to life-threatening complications, including:
A healthcare provider will take X-rays in the region where your symptoms occur (your neck, chest or abdomen). They’ll look for signs of esophageal perforation, including air pockets and leaked fluids. To confirm the diagnosis, they might follow up with another imaging test called an esophagram. For this test, you’ll swallow a contrast solution that will highlight the inside of your esophagus on the X-ray.
Advertisement
Once your diagnosis is confirmed, your healthcare team will want to treat it as soon as possible. They’ll need to address the tear while also managing any complications. Standard treatment includes:
The type of repair or intervention you’ll need will depend a lot on the size of the hole or tear and the overall condition of your esophagus. Some people with very minor injuries may not need direct repair. A stent or tube in your esophagus can seal off the perforation until it heals by itself. In other cases, a surgeon might need to remove dead tissue, a foreign body or a tumor and then close the wound.
Advertisement
If you have a severe injury and/or preexisting damage to your esophagus, you might need part or all of your esophagus removed. If you have other complications, you may need additional interventions.
You can recover from a torn esophagus, but your prognosis (outlook) depends on how severe the tear is and how soon you get treatment. Minor tears that get treatment within 24 hours have the best prognosis. If you go 48 hours or more before treatment, you’re more likely to develop life-threatening complications. Those who need more extensive surgery or other emergency interventions have higher mortality rates.
Esophageal ruptures are frightening. Fortunately, they’re rare. But when they do occur, they can be difficult to recognize right away. This is one of many reasons to always take chest pain seriously.
Your esophagus wall is thin and vulnerable, and it can be injured unexpectedly. When it’s injured, you might not realize where the pain is coming from or what it means. Regardless, don’t try to tough it out. If you ever feel a sudden, severe pain in your chest, or even in your throat or upper abdomen, go to the emergency room. Even a small esophageal tear can lead to infection and all of its possible complications.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Esophageal disorders can cause many symptoms, including heartburn or trouble swallowing. At Cleveland Clinic, we’ll find a treatment that works for you.
