Septic shock is the most dangerous stage of sepsis, when an infection triggers a harmful chain reaction in your body. Septic shock can cause dangerously low blood pressure, organ failure and even death. Knowing the warning signs, acting quickly and getting immediate treatment can help save your life.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
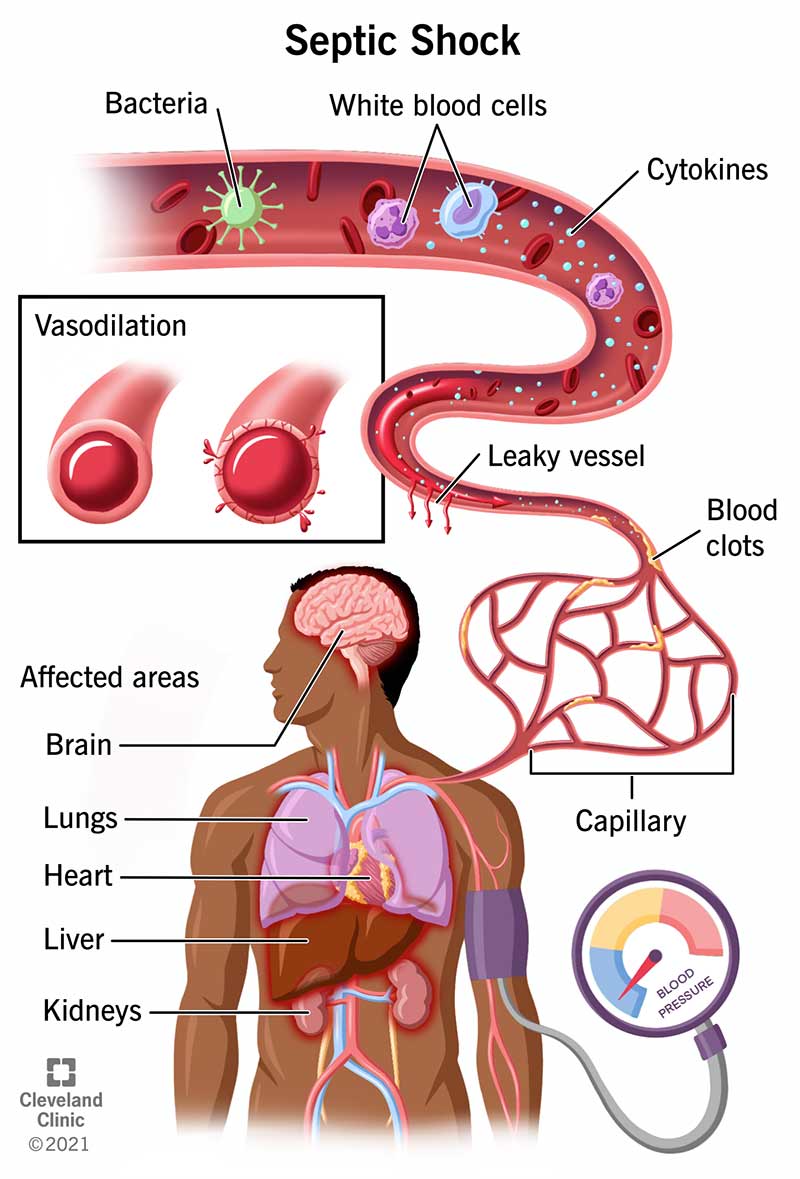
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23255-septic-shock)
Septic shock is the most severe, dangerous stage of sepsis. Sepsis is a serious condition that occurs when your immune system overreacts to an infection and starts harming your body.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Septic shock can cause extremely low blood pressure and organ failure even with fluid treatment. With septic shock, your cells aren’t using oxygen properly, and the way your body uses energy is disrupted.
Septic shock is life-threatening and requires immediate medical treatment.
Sepsis exists on a scale of severity. It may start with an infection and bacteria in your blood (bacteremia). It can then progress to septic shock. This can lead to multiple organ failure and death.
In other words, sepsis is like your house is on fire and it’s spreading quickly. Septic shock is like the fire is so intense that the walls are falling in — the structure is collapsing.
When sepsis turns to septic shock, your blood pressure will begin to drop significantly. You may experience very high and then very low body temperatures. Symptoms of septic shock can affect your whole body. These may include:
Septic shock happens when an infection triggers such an extreme immune response that it causes a chain reaction of harmful effects throughout your body. The steps involved in developing septic shock are:
Advertisement
Your chances for developing septic shock increase if:
Septic shock is a serious medical condition that can lead to severe complications, including:
Your healthcare provider may diagnose septic shock if you have sepsis and you start to develop worsening signs and symptoms. These include extremely low blood pressure, cooler limbs and skin discoloration.
Your provider may order certain tests, including:
If you develop septic shock, you need immediate treatment. You’ll likely be transferred to an intensive care unit (ICU). Depending on your condition, healthcare providers may try several septic shock treatments, including:
Yes, but recovery can take a long time. You may continue to have symptoms for months or years. These long-term effects are called post-sepsis syndrome. These effects can include:
Advertisement
To help with your recovery, make sure you:
Septic shock is a severe, life-threatening condition. People do survive, but the survival rate is low. Survival depends on several factors, including:
Without immediate treatment, most people die if they develop septic shock. According to studies, rates of death — even with treatment — range from 10% to 52%. Early recognition and fast treatment can make a lifesaving difference.
To prevent septic shock, you need to prevent sepsis. The best way to do that is to avoid getting infections. If you do get an infection, get treatment right away.
It’s also important to keep up to date on your vaccines. Vaccines can help prevent some infections, and they greatly lessen the severity of others.
Septic shock is a medical emergency. Knowing the signs, acting fast and getting immediate treatment can save your life. If you have a bacterial infection, see your healthcare provider right away. Septic shock can feel overwhelming to think about — but knowing what it is, how it happens and when to act can make all the difference.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Whether you need stitches, a broken bone set or think your appendix might be causing your abdominal pain, Cleveland Clinic’s emergency medicine team is here to help.
