Cholangiocarcinoma is cancer that forms in your bile ducts. It doesn’t cause symptoms in the early stages, so it’s often advanced and hard to treat by the time a healthcare provider finds it. Treatments include surgery, chemotherapy and gene-targeted therapies. Palliative care to ease symptoms is often a key part of treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Learn about biomarker testing, what to eat, managing your mental health and more.
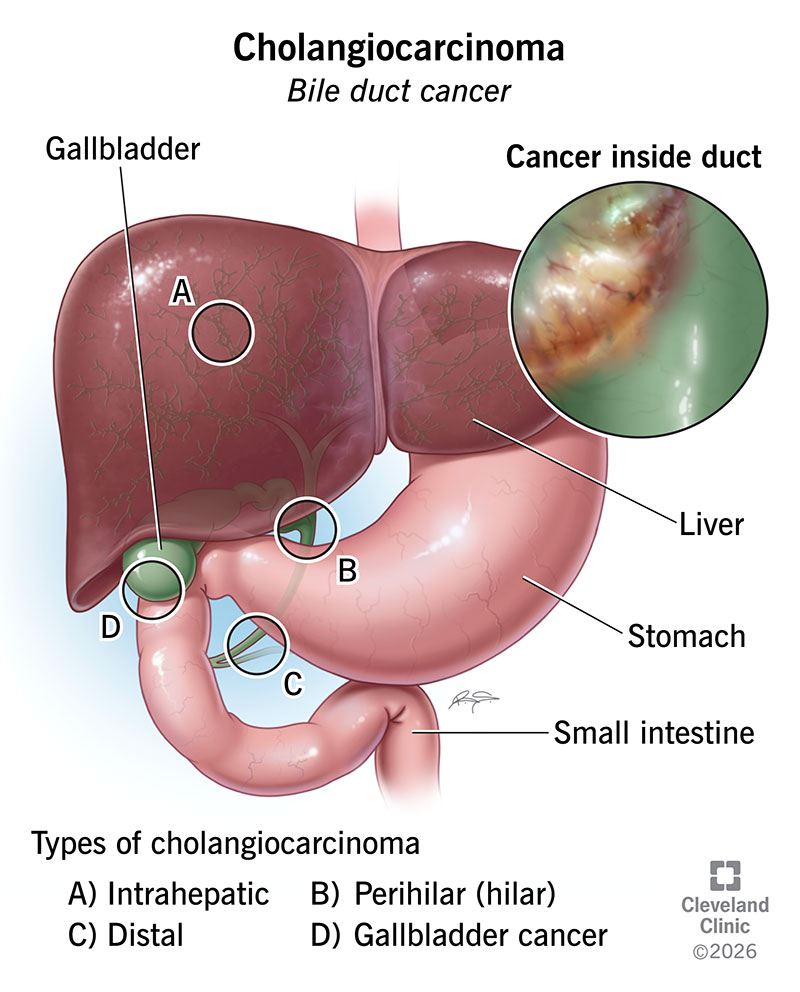
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/bile-duct-cancer-cholangiocarcinoma)
Cholangiocarcinoma is a rare cancer that starts in your bile ducts. It’s also called bile duct cancer. Bile ducts are tubes that bring bile from your liver and gallbladder to your small intestine. Bile is a fluid that helps you digest fats.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This disease is aggressive, which means it spreads fast. It doesn’t often cause symptoms in the early stages, when surgery might cure it. Most people don’t find out they have it until it’s already advanced. At this point, it’s challenging to treat.
Still, no two diagnoses are the same. Your treatment plan and outlook depend on lots of factors that your healthcare provider will discuss with you.
There are four types:
Symptoms don’t usually start until the tumor blocks a bile duct. At this point, it’s usually advanced. Symptoms include:
Advertisement
Experts don’t know what causes cholangiocarcinoma. But conditions that cause long-term inflammation in your bile ducts may play a role.
Ongoing damage from inflammation can cause changes in cell DNA. DNA contains the instructions that tell cells how to work properly. But damaged DNA can cause cells to keep growing and dividing when they shouldn’t. The cells can cluster together to form tumors that damage tissue.
Cholangiocarcinoma is most common in Southeast Asia. This is because it’s sometimes a complication of an infection from a Chinese liver fluke parasite called clonorchiasis.
Most people with this disease don’t have any known risk factors. But experts have found some conditions that may make you more likely to develop it, such as:
Your healthcare provider will consider your symptoms and medical history. You may need:
Providers use your test results to stage the disease, or learn how advanced it is. Staging systems vary based on the type of cholangiocarcinoma.
But in general, they rank the disease from stage 0 to stage IV (4). Stage 0, or carcinoma in situ, is the earliest stage. This means you have abnormal cells that could become cancer, but haven’t yet. Stage IV is the most advanced. At this stage, it’s spread beyond your bile ducts to distant organs.
Surgery can treat bile duct cancers that haven’t spread. Other treatments can make surgery more effective. Or they can help you live longer without surgery. As this disease doesn’t always respond to current treatments, your healthcare provider may suggest you take part in a clinical trial to access new therapies.
Surgery is the main treatment for earlier-stage disease. But it’s only an option when your surgeon can remove the tumor without harming your liver or key structures that drain your bile ducts. Only about 2 to 3 out of every 10 people diagnosed with bile duct cancer meet these criteria.
A liver transplant is a possible cure for some types of the disease. This procedure replaces your liver with one from a donor.
This treatment sends drugs throughout your body to destroy cancer cells. You may need it after surgery to get rid of any remaining cancer cells. Chemo can sometimes shrink tumors so they’re small enough to remove with surgery. Or it may help you live longer with fewer symptoms.
Advertisement
Special types of chemotherapy allow providers to send the treatment directly to a tumor. They include:
This treatment uses X-rays from a machine to kill cancer cells or shrink tumors. Providers often use it alongside chemotherapy. Sometimes, providers place tiny beads of radiation in the blood vessels supplying a tumor to shrink it. This is called transarterial radioembolization (TARE).
This treatment can destroy cancer cells that have certain gene errors. They include genes linked to several types of cancers, including FGFR2, HER2 and BRAF. The errors cause cancer cells to make proteins that fuel their growth. Targeted therapies block the proteins.
This treatment helps your body fight cancer. Some cancer cells contain a protein that prevents your immune cells from attacking. Immunotherapy disables this protein so immune cells can fight the cancer.
Your provider may suggest lesser-known cancer treatments that can provide symptom relief. In some cases, they help people live longer. They include:
Advertisement
Learn about biomarker testing, what to eat, managing your mental health and more.
Bile duct cancer is an aggressive and often fatal disease. It can be cured if surgery removes all of it. But surgery isn’t always successful. The tumor can come back. Your provider will monitor you to ensure you get the treatment you need if it does.
Most cancers aren’t diagnosed until they’re too advanced for surgery. At this point, the focus shifts from curing the cancer to slowing its progression. Palliative care is important, too. It can help you manage the physical and emotional challenges of living with this disease.
Fewer than 2 out of 10 people diagnosed with this disease survive past five years.
Still, it’s important to remember that lots of things affect your life expectancy. And new treatments are helping people with cancer live longer with fewer symptoms. Plus, survival rates report on numbers from previous years. They don’t reflect the advancements.
This is why it’s a good idea to talk to your healthcare provider about your prognosis based on your situation.
Bile duct cancer, or cholangiocarcinoma, is a difficult cancer diagnosis to receive. Research into more effective treatments is ongoing. But for now, it’s still one of the most challenging cancers healthcare providers treat.
Advertisement
This is why it’s important to find a care team you trust to guide you through treatment. It’s essential to take care of both your body and your mind. This may mean joining a support group or connecting with a therapist you trust. It may mean getting help from palliative care specialists. There are resources available. You’re not alone in the fight against this disease.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s cancer experts diagnose and treat bile duct cancer (cholangiocarcinoma) with the latest therapies and compassionate care that focuses on you.
