A coronary artery spasm is a quick tightening of the blood vessels that deliver blood to your heart muscle. These spasms may cause chest pain, or you may not feel any symptoms. You often have coronary spasms late at night or early in the morning. Treatment focuses on relieving chest pain and preventing spasms.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
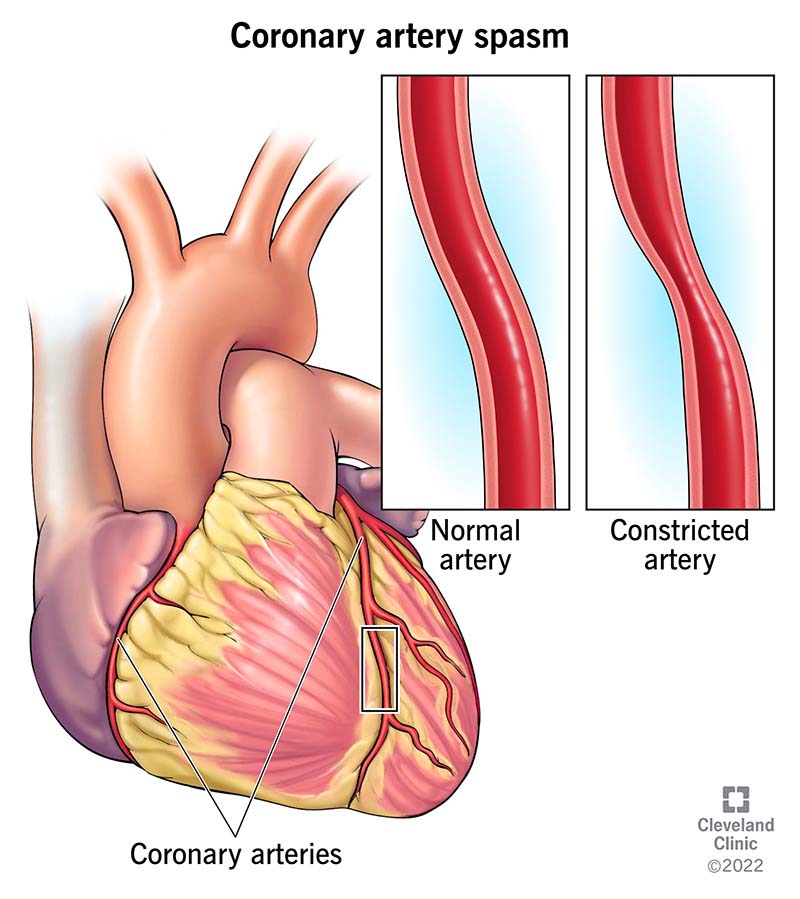
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/16900-coronary-artery-spasm)
A coronary artery spasm is a tightening (contraction) of your heart’s arteries (coronary arteries). These spasms don’t usually last long, and you may not even notice them. But they can increase your risk of heart attack and other heart complications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your coronary arteries are blood vessels that supply blood to your heart muscle. When these arteries tighten, they temporarily decrease or block blood flow to your heart muscle.
Coronary artery spasms may lead to chest pain known as angina. While artery blockage from cholesterol plaque is a more common cause of angina, coronary spasms can also result in chest pain called vasospastic angina. Unlike angina from plaque, vasospastic angina can often happen while you are resting.
If you have risk factors for heart disease, you also have risk factors for a coronary artery spasm. The most common risk factors include:
Many people who don’t have high blood pressure or high cholesterol experience coronary artery spasms. Often, these people smoke regularly.
Certain heart conditions can cause a coronary artery spasm, including:
Often, something triggers a coronary artery spasm, such as:
Advertisement
You may not have any noticeable symptoms of a coronary artery spasm. If you do, you might feel light chest pain, especially pain that occurs:
A coronary artery spasm may wake you up at night. You may have spasms as infrequently as a few times a year or as often as a few times a day.
Coronary artery spasms vary in length. They may last anywhere from five to 30 minutes.
Sometimes, you don’t feel a coronary artery spasm at all. Or you may feel:
To diagnose a coronary artery spasm, your healthcare provider uses tests that check your heart health, including:
Your provider may also give you an ambulatory monitor to wear at home. This monitor records your heart’s electrical activity as you do your daily activities. It gives your provider a better view of your heartbeat throughout the day. The monitor also records heart activity at night, which can be important for diagnosing coronary artery spasms.
The goal of treatment is to prevent spasms and relieve chest pain. If you have a spasm, a medicine called nitroglycerin (Nitrostat®) widens your arteries to improve blood flow and relieve chest pain.
To prevent spasms long term, your provider may prescribe medications:
Sometimes, coronary artery spasms lead to an irregular heart rhythm in your heart’s lower chambers (ventricular arrhythmia). If you have ventricular arrhythmia, your provider may recommend an implantable cardioverter defibrillator (ICD) to prevent any serious complications. ICDs use electrical signals to keep your heartbeat in a regular rhythm.
Coronary artery spasms are chronic, meaning you need long-term treatment to manage them. With treatment, most people control symptoms and experience fewer spasms.
If you have high cholesterol or other risk factors, treating these conditions can reduce your risk of spasms. You can also avoid triggers, such as extreme cold or smoking cigarettes, that can lead to coronary artery spasms.
Advertisement
Coronary artery spasms that last a long time may lead to a heart attack. Call 911 immediately if you have any signs of a heart attack, including chest pain along with:
A coronary artery spasm is a sudden tightening of the arteries that send blood to your heart. The spasms are quick and may be painless, but they can increase your risk of a heart attack. Coronary artery spasms often happen in late-night or early-morning hours and may wake you up. Treatment focuses on relieving chest pain and preventing spasms.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
