Percutaneous coronary intervention (PCI) is a treatment to open a blocked artery. Arteries are the blood vessels that carry oxygen-rich blood through your body. You may need a PCI if you have a buildup of a fatty, waxy substance (plaque) in your arteries. Or you may have a PCI to clear blockages after a heart attack. Another name for a PCI is coronary angioplasty.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
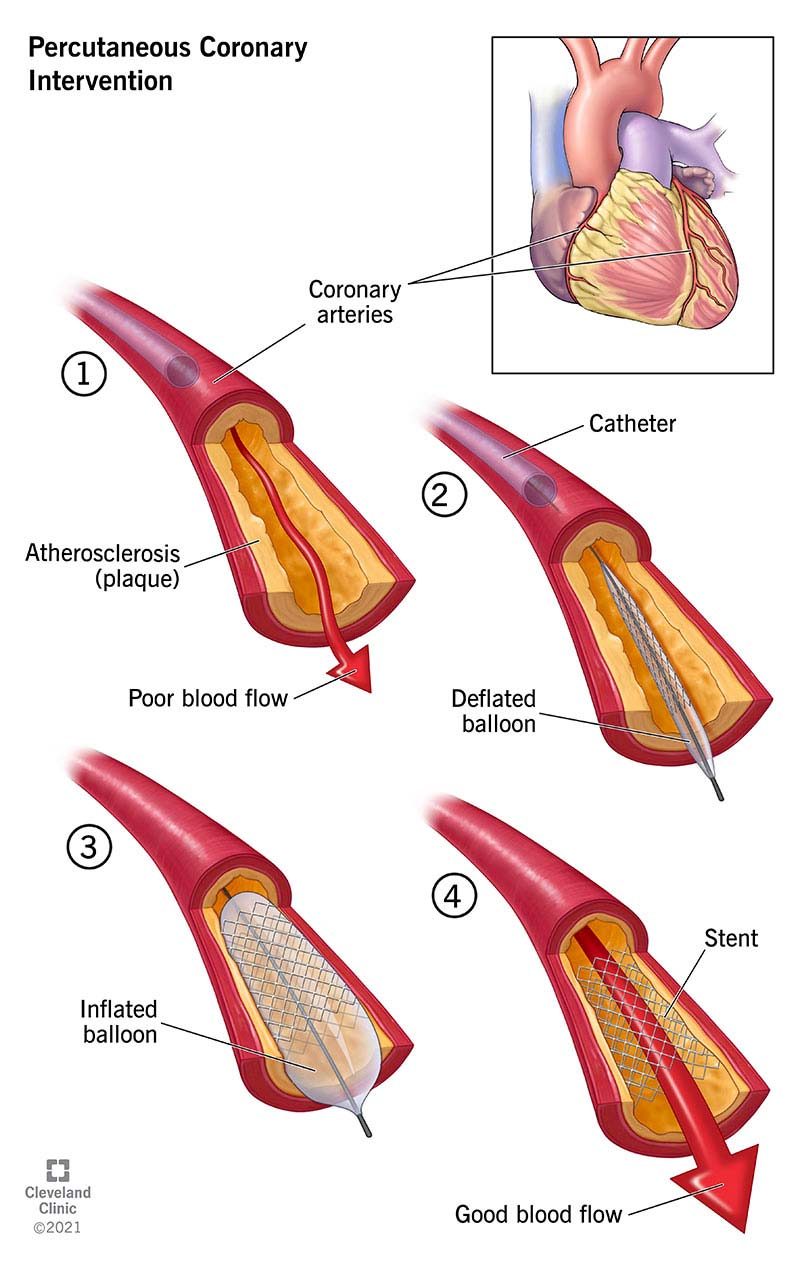
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22066-percutaneous-coronary-intervention-illustration)
A percutaneous coronary intervention (PCI) is a minimally invasive procedure to open blocked coronary (heart) arteries. An older name for PCI is coronary angioplasty with stenting or angioplasty for short.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Arteries are the blood vessels that carry oxygen-rich blood from your heart throughout your body. A PCI procedure uses a small balloon to reopen a blocked artery to increase blood flow.
Usually, your interventional cardiologist then places a small, permanent tube (stent) to keep the artery open long term. The stent usually contains medication that releases directly into your artery (drug-eluting stent) to reduce the risk of re-narrowing within the stent.
You may need a PCI procedure to remove buildups of a thick, fatty substance called plaque from your arteries. Plaque that builds up and hardens in your arteries is atherosclerosis.
Atherosclerosis increases your risk of cardiovascular disease and blocks blood flow through your heart. Your heart doesn’t pump blood efficiently, and you may have chest pain (angina).
Healthcare providers may also use PCI as a heart attack treatment. PCI quickly opens blood vessels, which can help minimize heart damage.
You and your healthcare provider will discuss which treatment is best for you. Whether you have PCI, medical therapy or coronary artery bypass graft (CABG) surgery depends on several factors that include:
Advertisement
Your healthcare provider gives you specific instructions to prepare for a PCI. In a non-emergency situation, you will likely need to not eat or drink (fast) for several hours before the surgery.
If you take blood-thinning medications (anticoagulants), you may need to stop taking them temporarily. These medicines can increase your bleeding risks during a procedure. Be sure to follow your provider’s instructions.
An interventional cardiologist (doctor specializing in the heart, blood vessels and circulatory system) performs the PCI. You receive a sedative (anesthesia) to help you remain calm and relaxed. You are usually awake but can’t feel anything during the procedure.
During a PCI, your cardiologist:
The procedure usually lasts between 30 minutes and two hours. The exact treatment time depends on several factors, including the extent of plaque buildup.
Usually, you stay in a recovery area for several hours after a PCI. You may have bruising or soreness where the doctor inserted the catheter. You might return home that day or stay in the hospital overnight.
A PCI improves blood flow in your heart. It can reduce the symptoms of a blocked artery, such as:
All heart treatments have some risks. Risks of a PCI procedure may include:
Percutaneous coronary intervention is generally a safe procedure with a low risk of complications. When providers perform a PCI using a drug-eluting stent, the likelihood that the artery will close again is less than 5%.
Usually, you can resume usual activities within a week after a PCI. If you have a job that requires physical activity or heavy lifting, you may need to wait longer to return to work.
During recovery from a PCI, your cardiologist may prescribe blood-thinning medicines. These drugs, such as clopidogrel (Plavix®), prasugrel (Effient®), or ticagrelor (Brilinta®), lower your risk of blood clots. You should take these medications according to the recommendations of your healthcare provider.
Advertisement
After a PCI, call your healthcare provider right away if you have:
Percutaneous coronary intervention is a heart treatment to open blocked blood vessels. You may need a PCI to remove plaque buildup in your arteries. Healthcare providers also use PCIs as an emergency heart attack treatment. PCI procedures are minimally invasive treatments. They often have shorter recovery times and a lower risk of complications than heart surgery. After a PCI, you should adopt healthy lifestyle habits to lower the chances that arteries will close again.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you need treatment for coronary artery disease, you want expert care. At Cleveland Clinic, we’ll create a treatment plan that’s personalized to you.
