Osteoporosis silently weakens your bones. This increases your risk of broken bones without you knowing it. You can prevent bone density loss with treatments and exercise. Ask your healthcare provider about a bone density test if you’re over 65 or have a family history of osteoporosis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
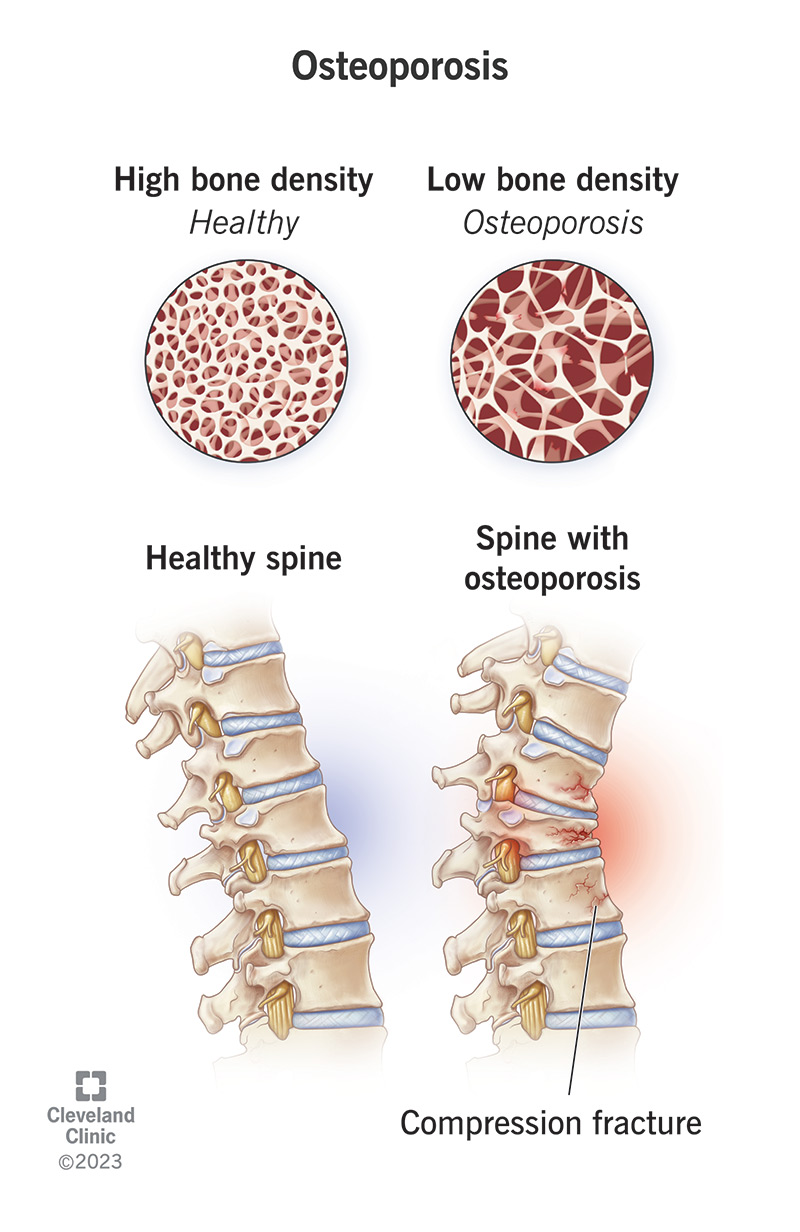
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/4443-osteoporosis)
Osteoporosis is a disease that weakens your bones and makes them much more likely to fracture. It makes your bones thinner and less dense than they should be.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your bones are usually dense and strong enough to support your weight and absorb most kinds of impacts. As you age, your bones naturally lose some of their density and their ability to regrow themselves. If you have osteoporosis, your bones are much more fragile than they should be, and are much weaker.
You might not know you have osteoporosis until it causes you to break a bone. Osteoporosis can make any of your bones more likely to break, but the most commonly affected bones include your:
Osteoporosis doesn’t have symptoms the way that lots of other conditions do. That’s why healthcare providers sometimes call it a silent disease.
You won’t feel or notice anything that signals you might have it. You won’t have a headache, fever or stomachache that lets you know something in your body is wrong.
The most common “symptom” is suddenly breaking a bone. Especially after a small fall or minor accident that usually wouldn’t hurt you.
Even though osteoporosis doesn’t directly cause symptoms, you might notice a few changes in your body that can mean your bones are losing strength or density. These warning signs of osteoporosis can include:
Advertisement
It might be hard to notice changes in your own physical appearance. A loved one may be more likely to see them, especially your height or posture. People sometimes joke about friends or family members “shrinking” as they age. But this can be a sign that you should visit a healthcare provider for a bone density test.
Around 1 in 3 adults over 50 who don’t have osteoporosis have osteopenia. This means your bone density is lower than it should be for your age. It’s an early sign of osteoporosis. Osteopenia can progress to become osteoporosis if it’s not treated.
Osteoporosis happens as you age and your bones lose their ability to regrow and reform themselves.
Your bones are living tissue like any other part of your body. They’re constantly replacing their own cells and tissue throughout your life. Up until about age 30, your body naturally builds more bone than you lose. After age 35, bone breakdown happens faster than your body can replace it. This causes a gradual loss of bone mass.
If you have osteoporosis, you lose bone mass faster than usual. People in postmenopause lose bone mass even faster.
Anyone can develop osteoporosis. You may have a higher risk if you:
Certain health conditions can make you more likely to develop osteoporosis, including:
Some medications or surgical procedures can increase your osteoporosis risk as a side effect, including:
A healthcare provider will diagnose osteoporosis with a bone density test. Providers sometimes refer to bone density tests as DEXA scans, DXA scans or bone density scans. All of these are different names for the same test.
A bone density test uses low levels of X-rays to measure how much calcium and other minerals are in your bones. It’s similar to a typical X-ray. There are no needles or injections.
Checking for changes in your bone density is the best way to catch osteoporosis before it causes a fracture. Your provider might suggest you get regular bone density tests if:
Advertisement
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_ah52zjad/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Registered dietitian Julia Zumpano explains how diet can improve bone health.
The most important part of treating osteoporosis is preventing broken bones. Your healthcare provider will suggest treatments to strengthen your existing bone tissue and slow down any bone density loss.
The most common osteoporosis treatments include:
Staying active can strengthen your bones. It also helps all the tissue connected to them, like your muscles, tendons and ligaments. Your provider might suggest weight-bearing exercise to strengthen your muscles and train your balance. Exercises that make your body work against gravity can improve your strength and balance without putting too much stress on your bones. Some good options include:
You might need to work with a physical therapist to find exercises and movements that are right for you.
You might need over-the-counter or prescription calcium or vitamin D supplements. Your provider will tell you:
Your provider may suggest prescription medications. Some of the most common osteoporosis medications include:
Advertisement
If you have severe osteoporosis or a high risk of fractures, you might need other medications, like:
These medications are usually given as injections.
Visit a healthcare provider if you notice any changes in your body that might be osteoporosis warning signs. Tell your provider about any other symptoms you’re experiencing, especially if you have bone pain or trouble moving.
You’ll need regular appointments with a healthcare provider. They’ll tell you how often you’ll need follow-up bone density tests. Your provider will monitor any changes in your bone density and will adjust your treatments as needed.
Broken bones can always cause complications. And that’s especially true as you age. Some fractures, like broken hips, can have a big impact on your life. Talk to your healthcare provider if you’re worried about your risk of falls or bone fractures. They’ll help you stay safe and healthy.
Staying physically active and making sure you get enough calcium and vitamin D are the best ways to support your bone health. But osteoporosis isn’t always preventable. Your provider will help you find a combination of treatments that’s best for your unique needs.
Advertisement
Osteoporosis can feel like the worst kind of surprise. You may never know you have it until you suddenly break a bone. Your healthcare provider can help you stay on top of your bone health. Before osteoporosis causes issues.
They’ll help you monitor your bone density. And they’ll suggest ways to strengthen your bones. Oftentimes, the things you do to maintain your overall health will also help your bones.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
You might have brittle bones, but an osteoporosis diagnosis doesn’t mean you can’t keep having fun in life. Cleveland Clinic is here to help.
