Trigeminal neuralgia is a chronic pain disorder that causes intense pain attacks in your face. It happens when your trigeminal nerve is damaged or irritated. Several treatment options can help relieve pain, ranging from medications to surgical procedures.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
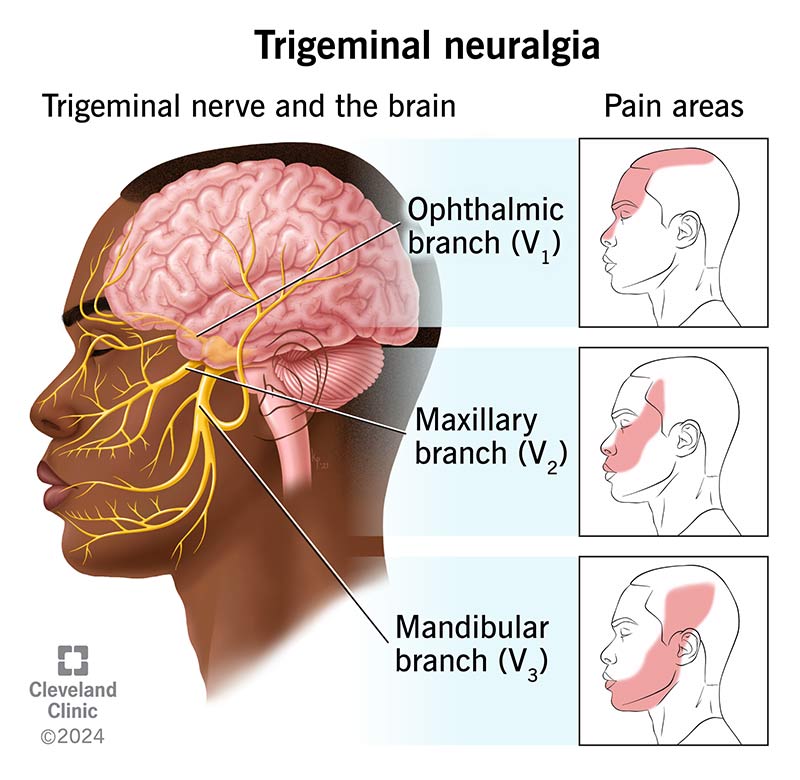
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15671-trigeminal-neuralgia)
Trigeminal neuralgia (TN) causes episodes of intense facial pain that can disrupt your everyday activities. It typically happens when a blood vessel puts pressure on your trigeminal nerve near your brainstem. This nerve provides sensation to your head and face. Trigeminal neuralgia is a type of neuropathic pain.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Trigeminal neuralgia isn’t life-threatening, but it can be life-altering. Activities as simple as chewing, talking, smiling and brushing your teeth can trigger brief bouts of intense pain, making TN both a physical and emotional condition. TN is typically chronic (long-term) but several treatments can help manage your symptoms.
Another name for trigeminal neuralgia is tic douloureux.
About 150,000 people in the U.S. receive a trigeminal neuralgia diagnosis every year. Females are more likely to develop it than males. Most cases develop after age 50. Trigeminal neuralgia very rarely affects children.
The main symptom of trigeminal neuralgia is sudden, intense pain in your face — usually on one side. The pain may be an electric shock-like or stabbing sensation. You may also have facial muscle spasms during the attacks. In between pain attacks, you may feel the following sensations:
There are two main forms of trigeminal neuralgia based on how you experience symptoms:
Advertisement
Typically, trigeminal neuralgia is unilateral, meaning it only affects one side of your face. In rare cases, it can affect both sides of your face (bilateral) but not at the same time. In some cases, trigeminal neuralgia can get worse over time with longer and more frequent pain attacks.
It’s mostly simple activities that require you to move or touch your face that can trigger painful TN episodes, including:
The pain attacks rarely occur during sleep.
In general, pressure on or damage to your trigeminal nerve causes TN. Healthcare providers categorize trigeminal neuralgia based on the specific cause:
Factors that may increase your risk of developing TN include:
To start, your healthcare provider will ask you about your symptoms and medical history. They’ll do a physical exam of your head and neck area and a neurological exam. They’ll likely make their diagnosis based on a few different factors, like:
Many conditions have facial pain as the main symptom, so your provider will need to rule them out. Examples include cluster headaches, migraines, postherpetic neuralgia and TMJ dysfunction.
Your provider may recommend a brain MRI to figure out what exactly is causing TN, like pressure from a blood vessel or a tumor.
Healthcare providers use a combination of medications, surgery and other therapies to treat trigeminal neuralgia. It may take time to find the best approach for you.
Medication is often the first therapy your provider will suggest for primary (classic) and idiopathic TN. They include:
Advertisement
Each of these medications has certain side effects. Together, you and your provider will decide which option is best for you.
Providers typically only consider surgery as a treatment for TN if:
Surgical options for TN vary in complexity and have a range of risks and side effects. Your provider will go over all the considerations with you. Surgical options for TN include:
Advertisement
Your provider may recommend other treatments for trigeminal neuralgia pain management — usually in combination with medication. They include:
Trigeminal neuralgia affects people differently. So, it’s difficult to predict how TN will affect you. Some people have a series of episodes that last for weeks or months, followed by pain-free periods. Others have persistent background facial pain in addition to pain attacks. For some, the pain attacks worsen over time. In addition, medications for TN might lose effectiveness over time.
For all of these reasons, it’s important to check in with your healthcare provider regularly about how TN is affecting you and if your treatment plan is working. You don’t have to live in constant pain.
The pain of trigeminal neuralgia is so severe that it can greatly affect your mental health and everyday life. People with TN are at risk of experiencing:
It’s crucial to seek professional help if TN is affecting your mental health. Reach out to your healthcare provider or a mental health professional, like a psychologist.
Advertisement
The treatments for TN may also lead to complications. Long-term use of antiseizure medications can cause issues like osteoporosis. Surgical procedures for TN can also lead to complications, like permanent facial numbness.
No one should have to live with frequent pain attacks. See your healthcare provider if you develop intense pain in your face. If you have TN, you’ll likely need to see your provider regularly to make sure your treatment plan is working for you.
It may be helpful to ask your healthcare provider the following questions about trigeminal neuralgia:
Although trigeminal neuralgia is a physical condition, it can just as greatly impact your mental and emotional health. You may become afraid of doing certain normal activities or avoid being around people for fear of experiencing intense pain attacks. The good news is that several treatment options can help you get back to living the life you enjoy — even if this is a condition that’ll likely be present, in some way, for the rest of your life.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
You don’t have to live with the electrical, shock-like pain that comes with trigeminal neuralgia. Cleveland Clinic providers are here to help you get relief.
