Temporomandibular joint disorders (TMDs) affect the joints that help your jaw move. They can cause pain, clicking, headaches and trouble chewing. TMD is common in adults and often starts between the ages of 20 and 40. Early care can make a big difference in how you feel day to day.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
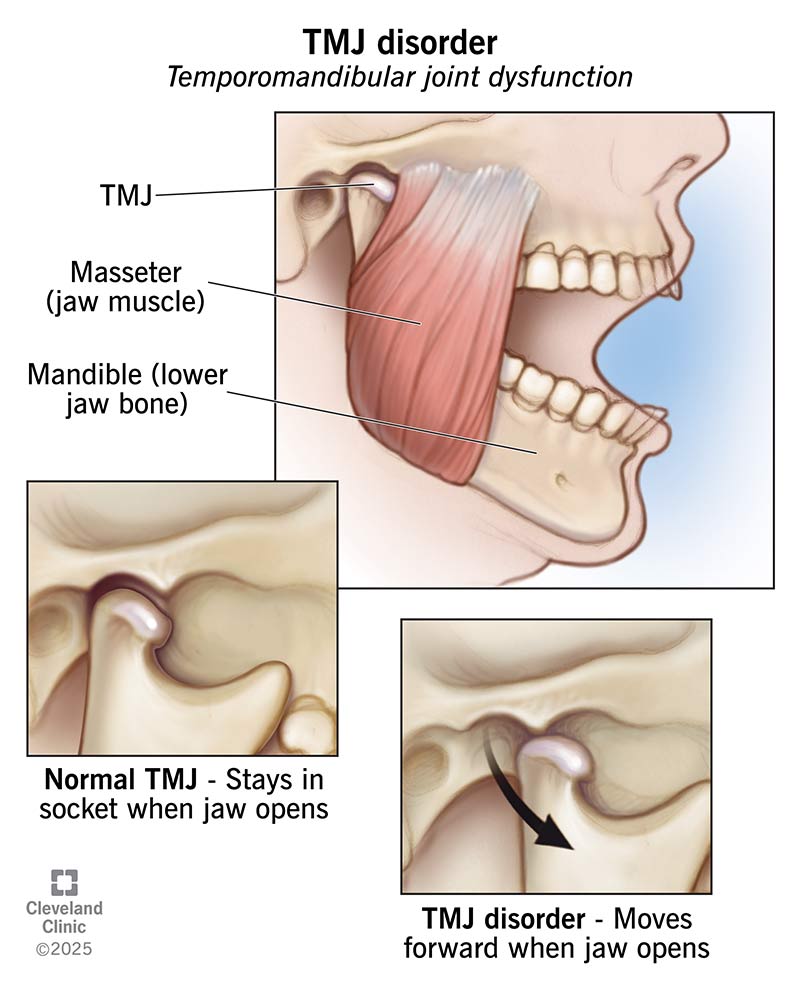
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/15066-tmj-disorder)
TMJ disorders affect the joints in your jaw and the muscles around them. The medical term is temporomandibular joint dysfunction (TMD), but many people call it TMJ.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You have two TMJs — one on each side of your face, near your ears. These joints help you chew, talk, and move your jaw.
TMD is common. It affects up to 12 million people in the U.S., mostly between the ages of 20 and 40. Females are twice as likely to have it.
The good news? It’s treatable and rarely causes lasting problems.
Signs of TMD can include:
If these symptoms don’t go away, see a healthcare provider.
TMD can happen for many reasons:
Some habits can make TMD worse:
Try these tips:
TMD can lead to long-term pain, chewing problems, or damage from grinding your teeth. The causes often overlap, so it may take time to find the right treatment.
Advertisement
To diagnose TMD, your provider will do a physical exam and may order imaging tests. They’ll check how your jaw moves and look for signs of pain or stiffness.
During your exam, your provider may:
You may also need imaging tests, like:
Finding TMD early can make treatment more effective.
Treatment depends on what’s causing your symptoms and how severe they are. Most people start with noninvasive options.
Medicines can help ease pain, swelling and muscle tension. Your provider may suggest:
Many therapies don’t involve surgery. They focus on relaxing your jaw and improving movement:
If other treatments don’t help, your provider may suggest surgery, such as:
TMD treatment often combines self-care, medical devices and professional care.
If your jaw pain, clicking or stiffness doesn’t improve, talk to a healthcare provider. They can help find what’s causing it and suggest the right treatment.
TMD can be short-term or last longer. Some people feel better in a week or two. Others may need ongoing care. With the right treatment, most people get relief and normal jaw movement.
Yes. With early diagnosis and the right treatment, TMD is often manageable — and sometimes curable.
TMD affects people in different ways. Whether your pain is short-term or ongoing, help is available. If symptoms are interfering with your daily life, don’t wait — talk to your healthcare provider.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Temporomandibular joint (TMJ) disorders cause more than jaw pain. Cleveland Clinic’s TMJ specialists offer the latest treatments for relief.
