Stress fractures are usually overuse injuries. They happen when physical activity puts too much pressure on a bone and it doesn’t have enough time to recover. Stress fractures start as bone bruises that eventually become small cracks in the bone’s surface. Common causes include playing a sport and a repetitive motion you do for your job.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
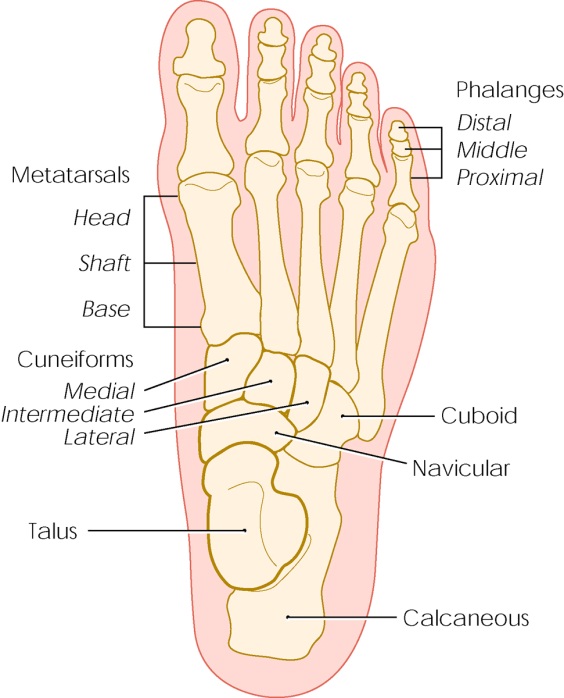
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15841-stress-fractures)
A stress fracture is a small crack in one of your bones. It’s a type of bone fracture (the medical term for broken bones).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Stress fractures are exactly what their name sounds like — fractures that happen when something puts too much stress on your bone. Healthcare providers sometimes call stress fractures overuse injuries because repetitively using the same part of your body usually causes them. You might also see stress fractures called hairline fractures, a name that refers to the hairline crack that forms in your bone.
Any repetitive motion or activity that puts pressure on your bones can cause a stress fracture — playing a sport or doing physical work are common causes. Visit a healthcare provider if you feel pain, swelling or tenderness on or near a bone (especially during or after physical activity).
Stress fractures usually affect weight-bearing bones in your lower body. These are the bones that support the weight of your body when you’re standing or moving. You’re most likely to experience a stress fracture in your:
They’re less common, but stress fractures can also affect bones in your:
Stress fractures are common injuries for athletes and people who do physical work. Experts estimate that stress fractures make up around 20% of all sports injuries.
Advertisement
The most common symptoms of a stress fracture include:
Most people with a stress fracture feel less pain after they stop physical activity. But you might feel pain all the time depending on where the stress fracture is. Because stress fractures are more common in your lower legs and feet, the pain is usually worse when you’re walking or standing with weight on your affected bone.
You’ll probably feel pain that’s focused (localized) in one spot near the fracture. For example, if you have a stress fracture in your foot, your whole foot might hurt, but the area around your damaged bone will be the most painful and tender.
Stress fractures are almost always overuse injuries. This means they happen when something puts too much pressure on a bone and the bone doesn’t have enough time to recover after physical activity. Stress fractures usually develop slowly over time when you do a repetitive motion (like training for a sport or performing the same type of movement all day at work).
Stress fractures start as inflammation on a bone’s surface (healthcare providers call this a stress reaction). Stress reactions are like deep bone bruises. If something keeps putting pressure on that same spot before the stress reaction can heal, your bone can crack and create a stress fracture. The bruise will reach deeper into the bone over time until it makes it weak enough to break. That’s when a stress reaction becomes a stress fracture.
Some of the most common causes of stress fractures include:
Athletes who play sports that put a lot of stress on their lower bodies are more likely to develop stress fractures, including:
Advertisement
Certain health conditions can increase your risk of a stress fracture, including:
A healthcare provider will diagnose a stress fracture with a physical exam. They might use imaging tests to confirm the diagnosis and take pictures of the fracture. They’ll examine the part of your body that hurts. Tell them what you were doing when you first noticed pain and other symptoms.
Your provider might ask you to stand or hop on one leg and then the other. This will help them understand where you might have a stress fracture, and how much it affects your ability to move normally.
Your provider might use some of the following tests to take pictures of your bones:
Your provider will suggest treatments based on the location of the fracture and the severity of your symptoms. The most common treatments for stress fractures include:
Advertisement
Advertisement
Most people don’t need surgery to treat a stress fracture. Your provider might suggest surgery if the fracture isn’t healing like it should, or if you’re experiencing severe symptoms. You might need surgery if the fracture’s in a bone that’s more likely to cause other complications (like your hip joint).
A surgeon will perform a procedure called an internal fixation. They’ll put pins, screws or metal plates into your bone to hold it together while it heals. Your provider and surgeon will tell you what to expect and how long it’ll take to recover.
You should start feeling better as soon as you stop putting stress on your injured bone and start treating your symptoms. Don’t resume training, working out or practicing before your provider says it’s safe, even if you’re feeling better. It’ll probably take at least a few weeks for your bone to heal enough before you can return to physical activities. The fracture can come back or get worse if you resume activity too soon.
Most people need to rest for at least a few weeks after experiencing a stress fracture. You might need to avoid sports and other physical activities for a few months.
As long as you can feel pain, the bone is still fragile in that area, and could break again in the same place. It usually takes six to eight weeks for a stress fracture to heal. Stop the activities that caused the stress fracture while you’re healing.
Your provider will tell you how long you need to take a break from playing sports or working out.
These steps can help prevent a stress fracture:
Don’t resume physical activities before your healthcare provider says it’s safe. If you stress your bone again before it has time to heal, you’re more likely to reinjure it.
Visit a healthcare provider as soon as you notice new symptoms like pain and swelling. Even if you don’t have a stress fracture, your provider can examine your injury and suggest treatments to prevent more serious complications.
Listen to your body if you’re experiencing pain during and after physical activity. Pain is often the first sign that you need to stop and rest. You can prevent a stress fracture before it happens by stopping physical activity and visiting a healthcare provider as soon as you notice pain and other symptoms.
Go to the emergency room right away if you’ve experienced trauma.
If you think you have a bone fracture, you need to see a healthcare provider as soon as possible. Go to the emergency room if you experience any of the following:
You might be able to walk normally with a stress fracture. It depends on which bone is fractured, and how severe your symptoms are. Your provider will tell you which types of movements are safe while you’re healing. Don’t jog, run, work out or do any intense physical activity without talking to your provider.
A healthcare provider needs to diagnose and treat all stress fractures. Even though rest and giving your body time to heal are the most common treatments, you still need your injury examined and diagnosed by a provider before you can return to sports or other physical activities.
Visit a provider if you’re experiencing stress fracture symptoms. The sooner it’s diagnosed, the faster your bone can start healing. Your provider will help you understand why the stress fracture happened and how you can prevent injuries in the future.
Stress fractures are one of the most common injuries athletes and physically active people experience. It’s frustrating to know your favorite sport or training regimen could’ve caused your injury. But don’t rush your recovery. Your bone and body need time to heal.
Visit a healthcare provider as soon as you notice any stress fracture symptoms. They’ll diagnose your injury and suggest treatments that help get you back out on the field, court or track as soon as it’s safe.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From sudden injuries to chronic conditions, Cleveland Clinic’s orthopaedic providers can guide you through testing, treatment and beyond.
