Thoracentesis is a procedure that a provider uses to drain extra fluid from around the lungs (pleural space) with a needle. It’s used to test the fluid for infection or other illnesses and to relieve chest pressure that makes it tough to breathe. Thoracentesis is a short, low-risk procedure done while you’re awake.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
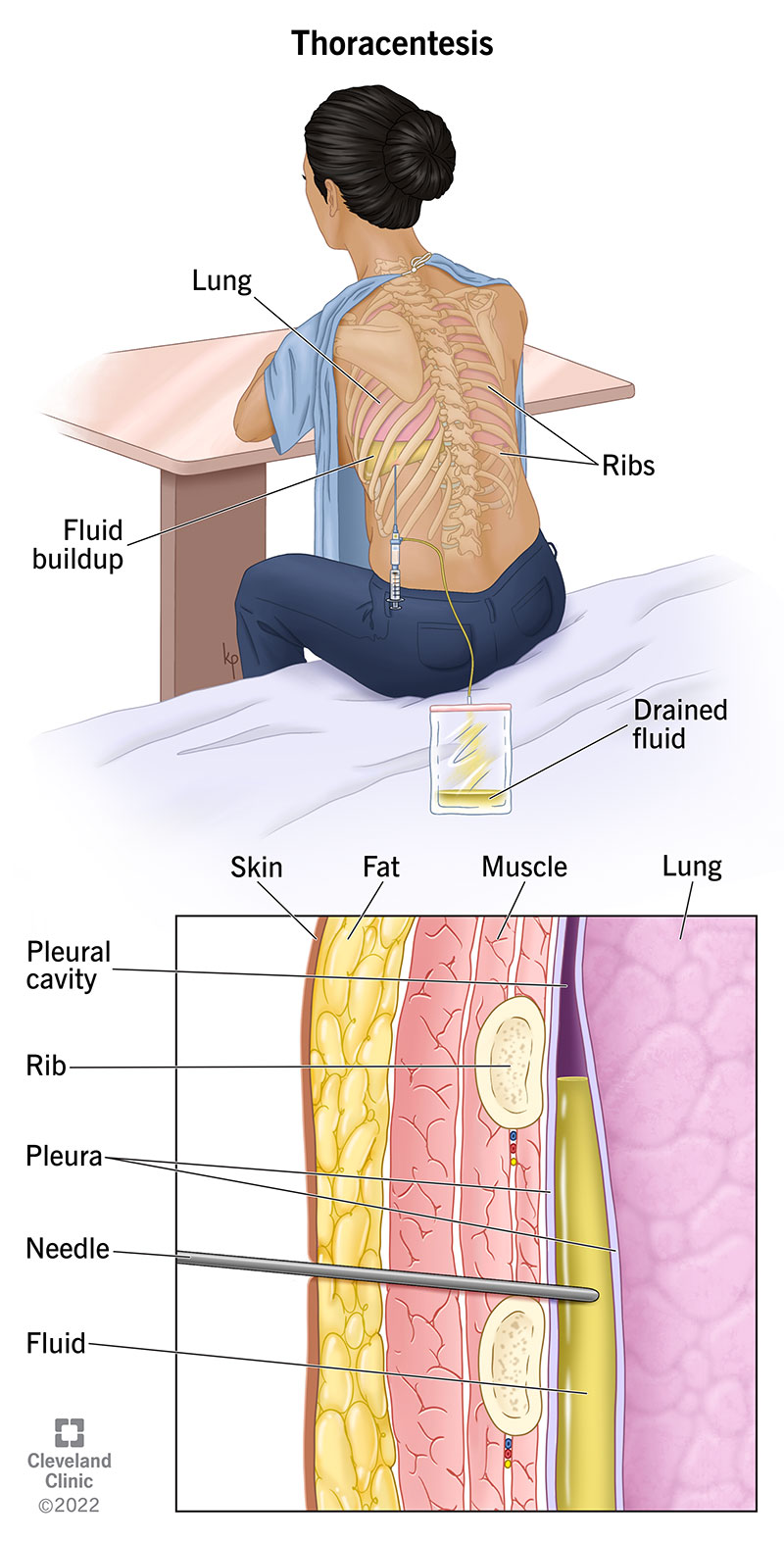
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/24254-thoracentesis)
Thoracentesis is a procedure that takes fluid out from around your lungs (pleural space). The pleural space is the area outside your lungs but inside your chest wall.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your lungs and chest wall are both lined with a thin layer called pleura. A small amount of fluid between these two layers helps them move smoothly past each other when your lungs get bigger and smaller as you breathe. Just like a hinge needs oil to help the door move smoothly, your lungs need pleural fluid to help you breathe.
Some medical conditions and diseases cause fluid to leak into the pleural space (pleural effusion), which makes it hard to breathe. Healthcare providers use thoracentesis to test the fluid for diseases or to relieve symptoms.
Thoracentesis and paracentesis both remove extra fluid from your body. Thoracentesis removes fluid from your chest and paracentesis removes fluid from your abdomen.
Thoracentesis drains fluid from your chest during the procedure, which usually lasts about 15 minutes. A chest tube, or a smaller drain with a curled end (pigtail catheter), stays inside your chest and drains fluid or air over a few days. It’s placed by a surgeon, pulmonologist or radiologist.
No, thoracentesis isn’t considered a major surgery. Thoracentesis is minimally invasive, which means your provider doesn’t have to make large cuts in your tissue. Recovery time for minimally invasive procedures is short and risks are much lower than for major surgery.
Advertisement
If you have a pleural effusion, you may need to have thoracentesis done to look for the cause or to make you more comfortable.
Thoracentesis is done either to relieve your symptoms or to test the fluid around your lungs (or both). Common reasons to have thoracentesis done include:
Thoracentesis treats pleural effusion, or excess fluid in the space between your lungs and your chest wall. It helps relieve symptoms and figure out what might be causing the fluid, so that your provider can treat it appropriately. Many underlying conditions cause pleural effusion, including:
Heart failure is the most common cause of pleural effusion.
Thoracentesis is a common procedure, with nearly 180,000 done each year in the U.S. alone.
Your healthcare provider will give you specific instructions on how to prepare for a thoracentesis. They may ask you to:
Tell your provider if you:
Before a thoracentesis, your provider will take your blood pressure and use a small device on your finger to measure your blood oxygen level. They’ll use imaging (X-ray, ultrasound or CT scan) before the procedure to see where the fluid is and how much of it there is.
You’ll change into a gown that’s open in the back and remove any jewelry. Your provider will have you sit with your arms resting on a table. If you’re unable to sit, you can lie on your side.
A thoracentesis is usually done at a hospital and takes about 15 minutes. Your provider may ask you not to move or to hold your breath at different points during the procedure.
Advertisement
You may feel pressure or discomfort while they take fluid out, but it shouldn’t be painful. Tell your provider if you have chest pains or feel short of breath or faint.
During a thoracentesis your provider will:
After a thoracentesis, your provider may get another X-ray or ultrasound of your lungs. If you’re going home afterwards, they’ll continue to watch your vital signs until it’s OK for you to leave.
You might cough for up to an hour after thoracentesis. This is normal and helps your lungs expand again.
Advertisement
Your provider usually sends the drained fluid to a lab. The lab will look for signs of infectious diseases or other causes of pleural effusion. Your provider will let you know what they find and what it means for your health.
Yes, you’re awake during a thoracentesis procedure. Your provider uses a local anesthetic to numb the surrounding area.
The best position for a thoracentesis is sitting up and resting on your arms on a table in front of you. Your provider can get to your back in this position and it’s easier to hold yourself still. If you can’t sit, you can lay on your side instead.
Thoracentesis shouldn’t be painful. Your provider will numb your skin before putting the needle in. Removing the fluid might cause you some discomfort, but it shouldn’t be painful.
Thoracentesis is a safe way to diagnose infections and other illnesses that cause pleural effusion. It also relieves pressure on your lungs, making it easier to breathe.
Your healthcare provider doesn’t have to make large cuts or damage tissue (minimally invasive), so there’s low risk of complications. It can be done as an outpatient procedure, which means you’re able to go home afterward.
Thoracentesis is a safe procedure with low risk for complications. Complications from thoracentesis usually aren’t serious. They’re minimized by locating the fluid with imaging before the procedure. Ask your healthcare provider to explain the risks in your specific case.
Advertisement
Risks of thoracentesis include:
Recovery time for thoracentesis is short. Your provider may tell you avoid strenuous activities for 48 hours. You can usually take off the bandage after 24 hours.
Ask your provider how to manage any symptoms or side effects you have after the procedure, including pain, coughing or fluid leaking from the drainage site. Follow their instructions for post-op care.
You should be able to go back to your everyday activities, like work or school, as soon as you feel up to it. Ask your provider if you have any restrictions on what you can do after a thoracentesis.
Many people have fluid on their lungs that keeps coming back because of an underlying medical condition. If you have a medical condition that causes pleural effusion, you may have to have multiple thoracentesis procedures.
Thoracentesis can be done as frequently as every few days for certain conditions. The risk of complications is minimized by making sure that the procedure is done only when necessary for symptom relief or to find the cause of pleural effusion.
Call or see your healthcare provider if you’ve had a thoracentesis and have any of these symptoms:
Thoracentesis is a common, low-risk procedure. It can give you answers about what’s causing the fluid around your lungs and relieve pressure that makes it hard to breathe. Don’t hesitate to ask your healthcare provider about any concerns you have. You’ll breathe easier afterward.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Breathing issues can affect your life in many ways. Cleveland Clinic’s respiratory therapy program treats your symptoms so you can feel better day to day.
