Program Overview
Since its inception in 1989 as the first U.S.-based physician Hospice and Palliative Medicine Fellowship, Cleveland Clinic’s Hospice and Palliative Medicine Program has trained clinically excellent physicians, physician educators and physician scientists.
At Cleveland Clinic, we believe that excellent palliative care requires a blend of extensive medical knowledge and deep personal connection. In our fellowship, we foster are collaborative and collegial, fostering a culture that promotes your education and career development. We desire a class of fellows from all backgrounds with varied interests and career goals who work together to provide the best possible care to patients.
Our fellows graduate with:
- Expert training in symptom management
- Mastery of family meetings
- Exposure to a broad spectrum of clinical disease and an understanding of where hospice and palliative care fits for each disease
- A unique experience tailored to their interests and desired career
|
|
|
Living in Cleveland
Cleveland, a mid-sized city located on Lake Erie, features a host of cultural attractions, recreational activities, major sporting events and an exploding culinary scene. Cleveland is home to the second largest theater district in the U.S., a park system featuring 23,700 acres in 18 reservations, and is the birthplace of rock ’n’ roll, home to the Rock ‘n’ Roll Hall of Fame and Museum. Cleveland Clinic is located near the University Circle area, which is the cultural epicenter of Cleveland. This area features Severance Hall and the world-renowned Cleveland Orchestra, the Cleveland Museum of Art, several other museums, and Case Western Reserve University. Downtown Cleveland, home to all major sports venues and an exploding culinary scene, is approximately two miles from Cleveland Clinic’s main campus.
Clinical Training & Didactics
In our fellowship program, we take the balance between service and education very seriously. Since you are with us for only one year, your clinical experiences play a key role in becoming the competent HPM physician you want to be.
Clinical Curriculum
- 1 week of palliative medicine bootcamp in July
- 22 weeks of inpatient palliative care consult services
- 4 weeks embedded with the Solid Tumor Oncology (STO) team
- 12 weeks on the general palliative consult service
- 6 weeks on the regional hospital palliative consult service
- 2 weeks of outpatient Palliative Care Clinic + 1 full day/week on other rotations (for a total of roughly 10 weeks in clinic)
- 6 weeks of home hospice and home palliative care
- 4 weeks of inpatient hospice
- 2 weeks of hospice long-term care at the VA’s Inpatient Unit
- 1 week of long-term care at a Long-Term Acute Care Hospital (LTACH)
- 2 weeks of inpatient pediatric palliative care
- 2 weeks of psycho-oncology
- 10 weeks of elective/selective time
- 2-4 weeks of electives
- 6-8 weeks of selective time
- Repeating any of the core hospice and palliative care rotations
- Bone marrow transplant or Leukemia embedded services
- Separate regional hospital experience
- 15 days of vacation and 5 personal days (20 days of PTO)
Popular electives include:
- Bioethics
- Radiation Oncology
- Addiction Medicine
- Chronic pain
- Acute pain
- Integrative Medicine
- Rotations in Hematology, Oncology, Pulmonary, Emergency, or other specialties.
- Research
- Medical education
- Business/Leadership
- Additional time on any of the primary services above.
- Create your own
Rotation Schedule
| Clinical rotation | Total Time |
|---|---|
| Orientation/Bootcamp | One week |
| General palliative consults | Twelve weeks |
| Solid tumor oncology consults | Four weeks |
| Hilcrest (Regional) Hospital consults | Six weeks |
| Inpatient hospice | Four weeks |
| Home hospice | Six weeks |
| Pediatrics | Two weeks |
| Outpatient clinic block | Two weeks |
| Long term care - LTACH | One week |
| Long term care - VA Hospital | Two weeks |
| Psycho-oncology | Two weeks |
| Electives/Selectives | Ten weeks |
Didactics and Beyond
Lectures serve to complement and enhance the learning that occurs on clinical services. This starts during orientation with our palliative care “bootcamp” and then continues with our monthly academic days. Academic days alternate between day-long communication skills retreats and lecture-based didactics on advanced palliative medicine topics.
Bootcamp
The year begins with a week of didactics prior to any clinical work, giving you a chance to develop a foundation for your clinical rotations and meet many of the attendings you’ll be working with. Bootcamp lectures cover the basics of communication, pain management, nausea, constipation, and other symptoms as well as practical matters such as overviews of the major rotations, documentation guidelines, EMR use, etc. We’ll have you feeling comfortable and prepared for patient care by the time you start seeing patients.
Communication Skills Training
Communication training consists of day-long retreats where fellows and faculty will learn, discuss and practice communication skills. The 7 retreats are spaced evenly throughout the year and designed to build over time to cover more and more advanced skills. Faculty keep the learning both enjoyable and impactful by employing a variety of techniques and drills from medical improv and sociodrama, as well as from Cleveland Clinic’s Center for Excellence in Healthcare Communication courses. Dr. Neuendorf brings her experience leading the Center for Excellence in Healthcare Communication, where she has taught communication skills to thousands of physicians across the country and the world.
Topics include:
- Foundational Skills
- Empathic statements
- Reflective listening
- Exploring the patient’s perspective
- Sharing information collaboratively
- Framework for family meetings
- Giving bad news
- Discussing uncertainty
- Sharing prognosis
- Code status discussions
- Communication Challenges – How to respond to:
- Patients focused on a miracle
- Patients using the “fight” metaphor
- Patients coping through denial
- Medical Mistrust
- Patients who experience racism or other forms of discrimination
Lecture Based Didactics
Lectures are taught by faculty in palliative medicine as well as related fields including psychiatry, ethics, geriatrics and interventional pain management. Lectures given throughout the year will include the essentials to be a competent specialist and will include advanced topics such as buprenorphine, ketamine, donation after cardiac death, pain management in substance use disorder as well as topics on education and leadership.
For an example, you can watch Dr. Neale give a talk on Ketamine.
Other Educational Series
In addition to lectures during the academic half-days, fellows will be able to participate in the following conferences:
- Journal club
- Palliative Medicine Grand rounds
- Case conferences
- Psychosocial rounds
- Narrative Medicine
- M&M conferences
- Interdisciplinary team meetings
- Psychosocial tumor board
- Opioid Management Review Committee
- Ask the Expert conference
Hospital & Rotation Locations
Hospitals
Most training will take place at Cleveland Clinic’s Main Campus. Fellows also will train at Hillcrest Hospital, a community-based hospital, and the VA. Fellows can choose to rotate with our palliative team at Fairview Hospital as well.

- Over 100 specialties are represented.
- 44 buildings, over 85 operating rooms, more than 1,400 beds and more than 200 ICU beds.
- To learn more about our facilities, visit our GME page for a virtual tour and overview of the resources and amenities available.

Taussig Cancer Center is located on Main Campus and is our department’s home, including outpatient palliative medicine clinic space, and office space for our fellows and staff.
Take a virtual tour of the Cancer Center.

- Hillcrest Hospital is a busy community hospital with 500 beds on Cleveland’s east side.
- Hillcrest Hospital features a level II trauma center and 48 ICU beds.

- Fairview Hospital is a busy 488 bed community teaching hospital on Cleveland’s west side overlooking the city's Metroparks.
- Features a level I trauma center and 52 ICU beds.
Louis Stokes Cleveland VA Medical Center
Heroes Harbor is a 12 bed inpatient hospice unit located in the Louis Stokes Cleveland VA Medical Center.
Fellows
Current Fellows
Class of 2025-2026

Michael Dinh, DO
Hometown: Austin, Texas
Medical School: Kansas City University College of Osteopathic Medicine
Residency: Texas Health HEB – Internal Medicine
Hobbies: Dancing (two-step, swing, salsa), leisure reading, exploring the local restaurant scene
Why did you choose Cleveland Clinic? Getting to know the program during AAHPM Annual Assembly was a wonderful experience that really drew me to Cleveland Clinic. Additionally, I want to pursue training that would prepare me for any and all future opportunities while also pushing me to be the best physician I can be.

Frank Dresner, MD
Hometown: Charlottesville, Virginia
Medical School: Lékarská Fakulta, Univerzity Karlovy
Residency: Mercy Health – Saint Elizabeth Youngstown Hospital - Internal Medicine
Hobbies: Baking, traveling, watching TV
Why did you choose Cleveland Clinic? I want to train at Cleveland Clinic because of its commitment to providing equal access to healthcare and the opportunity to serve a wide-ranging community. Its commitment to innovation, education and multidisciplinary care aligns with my goals of becoming a well-rounded, compassionate physician.

Alec Good, DO
Hometown: Blacksburg, Virginia
Medical School: Philadelphia College of Osteopathic Medicine
Residency: Trident Medical Center, Charleston, South Carolina – Emergency Medicine
Hobbies: Photography, scuba diving, international travel, strength training, hiking, golf
Why did you choose Cleveland Clinic? I chose Cleveland Clinic for the opportunity to work in one of the most robust hospital systems worldwide and to train in a location which would expose me to challenging and complex medical situations. Also – and perhaps most importantly – the vibes were great!

Eiman Kazi, DO
Hometown: Los Angeles, California
Medical School: College of Osteopathic Medicine of the Pacific
Residency: UCSF – Fresno Medical Education Program – Internal Medicine
Hobbies: Reading, journaling, nature hikes, traveling, exploring coffee shops and trying new restaurants
Why did you choose Cleveland Clinic? I chose Cleveland Clinic because I wanted exposure to a wide range of pathology and medically complex cases. I also had a wonderful interview day and could tell I would be working with very supportive faculty.

Kelly Makino, MD
Hometown: Rochester, New York
Medical School: University of Rochester School of Medicine and Dentistry
Residency: University of Hawaii J A Burns, School of Medicine – Family Medicine
Hobbies: Adventuring with my husband and kids (traveling, exploring nature, visiting family), cooking (especially inspired by our farm share offerings), music, dancing (mostly family kitchen dance parties these days), reading, listening to audiobooks/podcasts and playing board games
Why did you choose Cleveland Clinic? I was excited to join a program with a larger fellowship cohort, where learning happens not only through faculty and patients, but also through peer collaboration. The faculty I met during interviews felt like the kind of role models I hoped to learn from — kind, compassionate, thoughtful and all-around good people. The program’s culture strikes a meaningful balance between academic rigor and deep humanism, with strong interdisciplinary integration and a commitment to caring for the whole person. Altogether, the Hospice and Palliative Medicine team at Cleveland Clinic feels like the ideal environment for my training.

Ashley White, DO
Hometown: Harrisburg, Pennsylvania
Medical School: Lincoln Memorial University- DeBusk College of Osteopathic Medicine
Residency: Sinai Hospital of Baltimore – Internal Medicine
Hobbies: Card games, visiting aquariums and zoos, paint-by-numbers, fishing with my husband
Why did you choose Cleveland Clinic? Aside from its proximity to family, I chose this program for its rare balance: the breadth of a major academic center’s broad spectrum of pathology paired with a genuine focus on quality of life – not just for patients, but for trainees as well. Even before starting, it stood out for its flexibility, offering fellows the ability to tailor their year to individual goals, supported by expert one-on-one mentorship and distinctive communication training.
Class of 2024-2025

Kodiak Carb, MD
Hometown: Bryn Mawr, PA
Medical School: Drexel University College of Medicine
Residency: Allegheny Health Network – Internal Medicine
Hobbies: Yoga, Lifting weights, Running, Hiking, Baking
Why did you choose Cleveland Clinic? I chose Cleveland Clinic for my fellowship because of the environment they portrayed and kindness they exhibited.

Nathaniel Larson, MD
Hometown: Jamestown, NY
Medical School: University of Virginia School of Medicine
Residency: University of Rochester Medical Center – Internal Medicine
Hobbies: Snowboarding, Guitar, Running, Super Smash Bros.
Why did you choose Cleveland Clinic? Why Cleveland Clinic - I wanted to train at a program where I knew I would be exposed to a wide spectrum of clinical cases and complexity. I also had a great experience on my interview day, and I could tell right away that I would be learning in a supportive environment with passionate people.

Brigid Prayson, MD
Hometown: Shaker Heights, OH
Medical School: Ohio State University College of Medicine
Residency: Allegheny Health Network – Internal Medicine
Hobbies: Hiking with my dog, spending time with family/friends, food(exploring restaurants), flower arranging, reading
Why did you choose Cleveland Clinic? I wanted to train here because it serves patients from all backgrounds, culture, disease processes, demographics and the dedication to education, innovation and quality of patient care. Cleveland is home for me, and I am excited to have the chance to learn and train while serving my own community.

Mikisa Solomon, MD
Hometown: Connellsville, PA
Medical School: University of Pittsburgh Medical Center
Residency: University of Pittsburgh Medical Center – Internal Medicine
Hobbies: Working out, Gluten-free baking, Writing, Traveling, Playing with my puppy
Why did you choose Cleveland Clinic? One of the reasons why I chose Cleveland Clinic was because of the medical complexity of the patient population. I, also, wanted to train at an institution that had a wide variety of clinical rotations to choose from to ensure that I feel well prepared for whatever path I choose within the field of Palliative Care.

Kayla St Lucia, MD
Hometown: Niskayuna, NY
Medical School: Lake Erie College of Osteopathic Medicine
Residency: University of Buffalo – Internal Medicine
Hobbies: Baking, True Crime Podcasts, Hiking
Why did you choose Cleveland Clinic? I chose Cleveland Clinic primarily for the positive and encouraging culture that I experienced on my interview day. One of my career goals is to be involved in academics and I feel that being at Cleveland Clinic would help me not only reach my career goals but provide me with the best education.

Michael Wiley, MD
Hometown: Chambersburg, PA
Medical School: Indiana University School of Medicine
Residency: Ohio Health Riverside Methodist Hospital – Internal Medicine
Hobbies: Winning at trivia around town, lounging at the pool, snuggling my cat Ferdinand, going on long walks listening to music
Why did you choose Cleveland Clinic? I chose Cleveland Clinic because it is a world-class institution with an incredible range of patients and medical complexity that will provide me both the depth and breadth of knowledge as a foundation for future practice.
Class of 2023-2024

Qurratulain Ahmed, MD
Hometown: Karachi, Pakistan
Medical School: Aga Khan University
Residency: UMass Chan Medical School, Baystate – Internal Medicine
Hobbies: Outside of work, I love cooking food that reminds me of home, reading books, spending time with my husband and Whats-apping the rest of my family back in Pakistan.
Why did you choose Cleveland Clinic?
I chose Cleveland Clinic - mostly because I had a wonderful interview day, felt very welcomed and comfortable with everyone I met. I knew that I would learn immensely being at a renowned, academic center with a high patient volume and significantly complex medical cases in an environment that is also conducive to learning.

Meena Bhaskaruni, MD
Hometown: Toronto, Ontario, Canada
Medical School: St. George’s University School of Medicine, Grenada
Residency: Ellis Family Medicine Residency, Schenectady – Family Medicine
Hobbies: Reading, dancing and watching TV
Why did you choose Cleveland Clinic?
Cleveland clinic is a world class institution that provides care for a wide spectrum of people. The program has a good mix of both inpatient and outpatient exposure as well as excellent training in palliative care and hospice.

Gurjit Brar, MD
Hometown: Vancouver, Canada
Medical School: Saba University School of Medicine
Residency: Leonard J. Chabert, Houma, LA – Internal Medicine
Hobbies: Running, cycling, hiking, star gazing
Why did you choose Cleveland Clinic?
The Cleveland Clinic has a robust curriculum, electives available towards my interests of teaching/administrative/ethics, structured fellowship support system, dedicated time for AAHPM, and begins with an educational ‘bootcamp’ designed to lay foundations early on in fellowship.

Max Geisinger, MD
Hometown: New York City, NY
Medical School: Sidney Kimmel Medical College at Thomas Jefferson University
Residency: University of Maryland Medical Center – Internal Medicine
Hobbies: Cooking, exploring new cities, live music and comedy
Why did you choose Cleveland Clinic?
I chose Cleveland Clinic because I wanted to learn as much as possible in a one-year fellowship. This program provides the opportunity to work on extremely complex cases with caring and talented colleagues at Main Campus, while also being able to rotate at several regional hospitals where you get exposure to community Hospice and Palliative medicine. During my interview day it was also clear that program leadership had thoughtfully considered why I'd be a good fit and were excited to get to know me better as a person.

Adeela Mushtaq, MD
Hometown: Wah Cantt, Pakistan
Medical School: Rawalpindi Medical College
Residency: University of Pittsburgh Medical Center McKeesport – Internal Medicine
Hobbies: Reading, spending time in nature and with my husband, stone painting
Why did you choose Cleveland Clinic?
I enjoyed the interview experience. Dr. Neuendorf amazed me with how she worked to choose my interviewers; I could see a lot of thought and emphasis went into making sure the candidate experience was positive. One interviewer, who shared my faith tradition, was able to connect with me, about her experiences at the hospital and city of Cleveland. And I came to learn that another scheduled interviewer, who at the last minute was not able to participate, was a former mentor and co-author I’ve worked with. I really appreciated the proactive efforts made for me.

Ashwini Ronghe, MD
Hometown: Mumbai, India
Medical School: Grant Government Medical College
Residency: University at Buffalo – Internal Medicine
Hobbies: Reading, Indoor rock climbing, Eating
Why did you choose Cleveland Clinic?
On a professional front I wanted a place where I would have exposure to working in different settings such as outpatient clinics, inpatient palliative care unit, intensive care unit as well as home visits. I also wanted to work with patients with different medical, surgical, oncologic, cardiac, and pulmonary conditions so I am a well-rounded physician at the end of the fellowship. On a personal front, I connected with Dr. Neuendorf over the kind of books we read and her vision for the field of Palliative Medicine. I felt a sense of family with the team where they truly look out for each other and help each other grow. And that's when I knew this was the place for me.
Post Fellowship
As you can see below, fellows from the past 10 years have left our program and are influencing the world of medicine in many different ways.
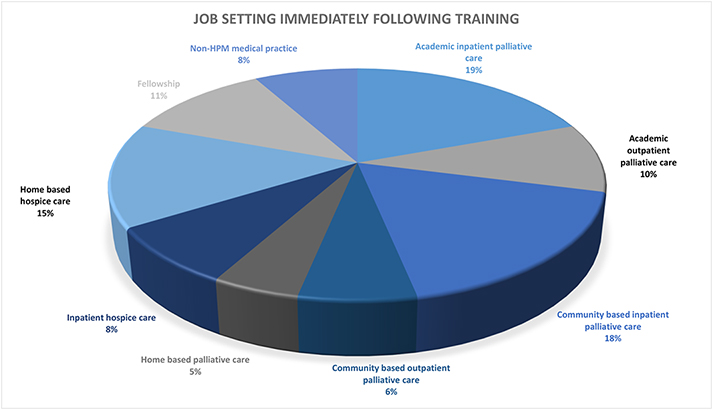
Our Staff
David Harris, MD
Program Director
Clinical Practice: Inpatient Palliative consults
Areas of Interest: Communication training
Something to know about Dave: I love to try new restaurants and keep a list of good places to eat for every city that I’ve been to. I like reading about psychology, decision-making or poetry
John Brandon Walters, MD
APD Evidence Based Learning and Resources
Clinical Practice: Outpatient Palliative Care, Hospice
Areas of Interest: Operations, Value based care
Something to know about Brandon: My first name is John but I go by my middle name Brandon
Laura Shoemaker, DO, MS, FAAHPM
Chair, Department of Palliative and Supportive Care, The Lois U. and Harry R. Horvitz Endowed Chair in Palliative Medicine
Clinical Practice: Outpatient Palliative Medicine
Areas of Interest: Leadership, Program Development, Coaching, Narrative Medicine
Something to know about Laura: In my free time I love to play tennis and cuddle my 2 beagles, Bosco and Lucy
Liz Weinstein, MD, MEd
APD Faculty Development
Clinical Practice: Outpatient Palliative Care
Areas of Interest: Communication skills teaching, Value based care, Clinical program development
Something to know about Liz: I grew up in Cleveland and came back after 18 years away to raise my kids here.

Sarah Persaud, MD
VA Faculty
Clinical Practice: I work in the inpatient hospice unit at the VA (Heroes Harbor) and see inpatient palliative care consults.
Areas of Interest: I have always had an interest in medical education. My favorite aspect of this is teaching learners at the bedside, but I do enjoy other aspects of education, including curriculum development, as well.
Something to know about Sarah: I think wellness for both learners and physicians is very important. I will always try to create a safe learning environment for rotators, and value life outside of the hospital.
Rotation Leads
Hospice Inpatient
Dr. Laura Hoeksema
Home/Field Hospice 1
Dr. Tracy Gulling-Leftwich
General Consults
Dr. Jason Ondrejka
STO Consults
Dr. David Harris
Hillcrest Consults
Dr. Kathryn Richards
Outpatient Clinic
Dr. Renato Samala
Long Term Care (VA Hospital)
Dr. Sarah Persaud
Long Term Care (LTACH)
Dr. Jafar Abunasser
Pediatrics
Dr. Kristin Carter
Fairview Consults
Dr. Katherine Eilenfeld
BMT Consults
Dr. Susan McInnes
Benefits
Comprehensive Health Plan: Graduate Medical Education at Cleveland Clinic offers a comprehensive and competitive benefits program that recognizes the needs of healthcare providers from a wide range of backgrounds and experience. as well as providing individuals and families with meaningful benefit choices.
- Dental Insurance.
- Vision Plan.
- Prescription Drug Benefit.
Retirement Programs: 403(b) Savings and Investment Plan (SIP)
- Funded with Pre-Tax, Roth, and/or After-Tax contributions.
- Fidelity Investments financial support by representatives at no cost.
Voluntary Benefits:
- MetLife Auto/Home/Pet Insurance.
- MetLaw Group Legal Plan.
- Global CARE Program.
Flexible Spending Accounts:
- Healthcare FSA.
- Dependent Care FSA.
Additional Insurance Coverage:
- Group Long Term Disability.
- Supplemental Individual Disability.
- Life Insurance.
- Professional Liability Insurance.
Paid Time Off (PTO):
- 20 vacation days.
- 3 separate days for post-fellowship job interviews.
- Sick days.
Travel Benefit: Cleveland Clinic strongly encourages trainees to participate in scholarly/research activities. Eligibility will be determined by the Program Director. Please refer to the Graduate Physician's Manual for further details.
- One Education Institute sponsored trip per academic year if presenting as a first-author with an accepted abstract (Maximum reimbursement of $2,500 per academic year).
- Funds are available for fellows in the accredited program to attend academic meetings for the purpose of presenting or engaging in leadership roles within national societies.
Maternity and Parental Leave:
- 100% pay for up to 8 weeks of maternity leave for mothers following childbirth.
- 100% pay for up to 4 weeks of parental leave for both parents following the birth or adoption of a child.
Board Exam Preparation: American Academy of Hospice and Palliative Medicine’s HPM Pass 4th Edition subscription.
- Mock exam scheduled during the second half of the year to simulate the board certification exam.
- Includes 80 peer-reviewed questions, covering 11 content modules identified in the current ABIM Hospice & Palliative Medicine Certification exam blueprint.
GME Annual Education Allowance:
- Cleveland Clinic aims to be the best place to train and the best place to work in healthcare. An important step toward that shared goal is the new annual educational allowance for clinical trainees, effective Jan. 1, 2024.
- The GME Office will provide each clinical trainee an educational fund of $1,000 for material to enhance their learning. The fund will be available annually starting on the day the trainee was first appointed and through the end of the trainee’s academic year.
iPhone: Clinical trainees will receive Cleveland Clinic issued iPhones during orientation.
Benefit Highlights: Find out what benefits you receive as a Cleveland Clinic trainee.
Finance Highlights: Get key information such as salary to help you manage your finances.
Support Programs
Well-Being Resources
- TT4 Gym: Access to exercise facilities that are reserved exclusively for residents and fellows.
- Gain access to facilities available to all CCF employees, as well as free fitness resources and mobile apps
- Walker Fitness Center
- Office of Caregiver Experience: Offers resources for emotional, physical, spiritual and social well-being
- Childcare resources
Well-Being Programs
- Emerge Stronger: Emerge Stronger is a confidential, one-on-one peer support program for any Cleveland Clinic caregiver distressed by an unanticipated clinical event, adverse event or medical/healthcare error. Support is provided by a peer in your field. This hospital-wide program was started by Dr. Hoeksema, one of our hospice physicians.
- Relaxation Program: Podcasts from Cleveland Clinic doctors on proper behaviors and techniques for relaxation.
- Stress Free Now: Six-week online program designed to decrease stress, build resilience and increase energy.
- Burnout Prevention Module: Helps to create a holistic, supportive culture of wellness and prevent trainee burnout.
- Wellness Connection: A 30-minute presentation delivered by a wellness industry professional on the third Wednesday of each month.
- Employee Wellness Monthly Newsletter: Events, raffles, and incentive programs.
- Healthy Choice Program: A voluntary discount program that offers employees an opportunity to receive discounted rates on their health plan through achieving well-being and health goals.
- Caring for Caregivers: A group of therapists that provide therapy exclusively to Cleveland Clinic caregivers either in person on main campus, or virtually.
Available Services & Support Programs
House Staff Association: Peer-elected representative body of Cleveland Clinic physician trainees (house staff), which includes residents and fellows.
- Advocate for and promote the well-being, interests, and education of Cleveland Clinic house staff.
- Provide input on policy to improve patient care and the work environment.
- Sponsors activities for house staff such as educational seminars, volunteer events, an annual art contest, painting with the DIO, QPS opportunities, outing to sporting events, fine arts exhibits and concerts.
Applying
Cleveland Clinic Hospice and Palliative Medicine Program
We appreciate your interest in applying to our Hospice and Palliative Medicine Fellowship Program. As the first established Hospice and Palliative Medicine program in the United States, we pride ourselves on fostering an environment that encourages continuous improvement initiatives and emphasizes patient-centered care. After completion of the fellowship program, our graduates feel confident that they can provide the best quality of life and clinical care for patients who are often feeling at their worst.
Application Process
All required clinical education for entry into ACGME-accredited fellowship programs must be completed in an ACGME-accredited residency program, or in an RCPSC-accredited or CFPC-accredited residency program located in Canada. Prior to appointment in the program, fellows must have completed an ACGME- or RCPSC-accredited program in child neurology, family medicine, internal medicine, pediatrics, physical medicine and rehabilitation, or neurology; or at least three clinical years in an ACGME- or RCPSC-accredited graduate educational program in one of the following specialties: anesthesiology, emergency medicine, obstetrics and gynecology, psychiatry, radiation oncology, radiology, or surgery.
The application process for fellowship is conducted through ERAS®. Please visit the ERAS® website for more information about the application process and up-to-date deadlines for the current application cycle. The following is a list of required ERAS® application materials:
- Personal Statement(s).
- Letters of Recommendation (Upload to ERAS® Letter of Recommendation Portal).
- Medical Student Performance Evaluation (Deans Letter).
- Medical School Transcript.
- ECFMG Status Report (International Medical Graduates Only).
- Photograph.
- USMLE and COMLEX Transcripts.
Advice on your application
We want to get to know you! The newer ERAS® application doesn’t have a clear place for you to share hobbies, passions, quirks, etc. We encourage you to add this to your application in any place that seems appropriate. In the past, applicants entered this as an "experience".
What we look for
We believe that if we set clear expectations for our learners, they will rise to the occasion. In that spirit, we are sharing what we look for on your CV and personal statement below.
CV:
- Experience working in any sort of job before residency
- Involvement in non-clinical activities, particularly involvement as a leader, or longitudinal involvement
- Nominated awards, especially peer nominated awards
- Involvement in research
Personal Statement:
- Experiences that show adaptability, grit or resilience
- Personal, compelling writing
- Experiences that show depth of character, wisdom or that make us want to meet you
Interview Process
We are offering a virtual interview out of respect for the time and financial burden that travelling for interviews can entail.
Here are some details about our interview day — Virtual Interface: Thalamus
- Interview length: Interview day runs from 8 a.m. to 1 p.m. EST for morning interviews, and from 12 - 5 p.m. EST for afternoon interviews.
- Interview agenda: Each candidate will receive a personalized agenda from the Program Coordinator prior to the interview day. This will include a detailed schedule for your interview as well as provide you with informational resources about our Fellowship Program and the Cleveland Clinic as an organization.
- Program overview: The interview day will begin a brief overview of the Fellowship provided by the Program Director. (Approximately 40 minutes)
- Current fellow Q&A: Following the overview, candidates will have the chance to interact with fellows from the current program separately to hear about their perspective and ask them questions. (Approximately 20 minutes)
- Teaching/Conference: Next, candidates will be provided with a short teaching conference by the Program Director so you are able to experience what a lecture might look like during a didactics session. (Approximately 25 minutes)
- Break: Prior to the interview sessions, candidates will have a short break. (Approximately 5 minutes)
- Interviews: The candidate will meet with the program director and 3-4 other members of our team. Each interview will last approximately 30 minutes, with a 10-minute break between each session. (Approximately 2 hours and 30 minutes total)
- Program director farewell: Everyone will jump back on a group call with the Program Director to review and finish the day. (Approximately 20 minutes)
Candidate Selection
We are a participant of the National Resident Matching Program (NRMP) Main Match and therefore, do not fill any positions outside of the Match. Applications will be accepted during the month of July each year for positions to begin July 1 of the next academic year. Please refer to the NRMP Website for more information regarding deadlines for the current application cycle.
Contact Us
Interested applicants are encouraged to contact our Fellowship Program Coordinator regarding inquiries into our program. We are dedicated toward making the fellowship application process as seamless as possible and look forward to interacting with you in the future.
Kaitlyn Lawson (She/Her)
Fellowship Program Coordinator
Email: lawsonk9@ccf.org
Phone: 216.636.1683
Location: Cleveland Clinic Taussig Cancer Institute
CA6, 9500 Euclid Ave., Cleveland, OH