Hypopharyngeal cancer is an uncommon cancer that develops in your lower throat, behind your voice box. Symptoms may include hoarseness, sore throat and ear pain that doesn’t go away after two weeks. Treatments include surgery, chemotherapy, radiation therapy and immunotherapy. You can reduce your risk by avoiding tobacco use and limiting alcohol.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
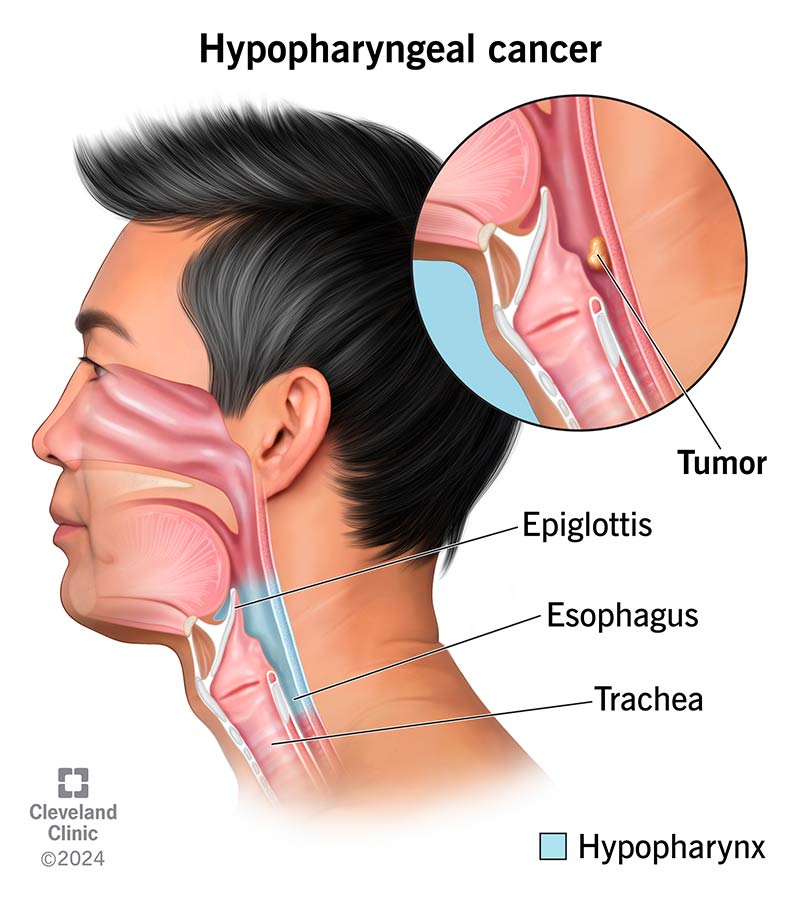
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/hypopharyngeal-cancer)
Hypopharyngeal cancer is an uncommon throat cancer that develops in your hypopharynx, which is in the lower part of your throat (pharynx) just behind your voice box (larynx). It causes cancerous tumors that often spread (metastasize) quickly to other areas of your body. You may not have noticeable symptoms until after tumors have spread. Treatment includes surgery and/or radiation therapy and chemotherapy to remove tumors and relieve symptoms.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It’s not common. Each year, an estimated 2,000 to 4,000 people in the U.S. receive a hypopharyngeal cancer diagnosis. For comparison, the American Cancer Society estimates more than 238,000 people received a lung cancer diagnosis in 2023.
Hypopharyngeal cancer may not cause symptoms right away. When it does, symptoms may include:
Hypopharyngeal cancer symptoms are similar to other, less serious conditions. Having any of the symptoms listed above doesn’t mean you have hypopharyngeal cancer. But you should talk to a healthcare provider if you have symptoms that last for more than two weeks.
Hypopharyngeal cancer develops in cells that line your hypopharynx. These cells mutate and become cancerous cells that multiply and create tumors. Experts don’t exactly why this happens, but they do know certain risk factors significantly increase the chance you’ll develop hypopharyngeal cancer, including:
Advertisement
Early on, hypopharyngeal cancer often spreads to lymph nodes in your neck. That’s why a lump in your neck is something you should discuss with a healthcare provider. Without treatment, hypopharyngeal cancer can spread to your:
A healthcare provider will ask you about your symptoms, including how long you’ve had them. They may ask about your tobacco and alcohol use because those activities can increase your risk of developing hypopharyngeal cancer.
They’ll do a physical examination that may include feeling your neck for swollen lymph nodes and examining your throat.
Depending on your symptoms, your provider may refer you to an ear, nose and throat (ENT) specialist or otolaryngologist, a provider who specializes in diagnosing and treating head and neck conditions. Your ENT may order the following tests to determine if you have hypopharyngeal cancer:
Cancer staging is how oncologists describe cancer in more detail, like tumor location, if or where it’s spread or if cancer affects other areas of your body.
Hypopharyngeal cancer stages range from Stage I (cancer in your lower throat that hasn’t spread) to Stage IV (cancer that has spread to other parts of your throat and mouth, your nasopharynx and the base of your skull, and more distant parts of your body like the lining of your chest cavity).
Advertisement
They also describe hypopharyngeal cancer by grade. A cancer grade can help oncologists predict how quickly cancer will spread. Hypopharyngeal cancer grades range from GX (cancer isn’t likely to spread or is less likely to spread) to G3 (cancer is likely to spread very quickly).
The most common treatments are surgery to remove the tumor and radiation therapy to kill any cancerous cells that may remain after surgery. Your oncologist may combine surgery with chemotherapy or immunotherapy.
Hypopharyngeal cancer surgical options are:
Advertisement
Throat surgery for cancer affects your ability to speak, eat and breathe. Before your surgery, ask your surgeon how treatment will affect you. For example, you may work with a speech-language pathologist to learn ways to manage any speech or swallowing issues from surgery.
Hypopharyngeal cancer can come back after treatment (recur). It also increases your risk of developing a new kind of cancer in a different area of your body. Healthcare providers may refer to this as second cancer.
As a result, you should expect to have regular follow-up appointments so your oncology care team can check on your overall health and watch for signs of recurrent or metastatic hypopharyngeal cancer or second cancer. Your follow-up care may include imaging tests and physical examinations. The schedule may include appointments every:
When you think about survival rates, it’s important to remember that survival rates are estimates based on other people’s experiences with hypopharyngeal cancer. Survival rates vary widely depending on whether a tumor remains where it started or spreads (metastasizes) to nearby tissues and lymph nodes (regional) or other areas in your body (distant).
Advertisement
These rates also vary depending on your overall health and other factors. Ask your oncologist to explain what survival rates mean in your situation. They know you and your overall health, which makes them your best resource for information.
The five-year survival rates based on tumor location are:
| Stage | Five-year survival rate |
|---|---|
| Local | 61% |
| Regional | 39% |
| Distant | 28% |
| Stage | |
| Local | |
| Five-year survival rate | |
| 61% | |
| Regional | |
| Five-year survival rate | |
| 39% | |
| Distant | |
| Five-year survival rate | |
| 28% |
In some cases, surgery and other treatments may cure hypopharyngeal cancer. That's more likely to happen if a tumor measures 2 centimeters or less and hasn’t spread. Unfortunately, most people with this cancer don’t receive a diagnosis until the condition is in advanced stages.
You can reduce your risk of hypopharyngeal cancer by:
If you had throat surgery, you’ll need to learn new ways to breathe and speak. That’s a lot of change to manage, so don’t hesitate to ask your speech-language pathologist for help. They may have suggestions about support groups for people recovering from throat surgery.
Here are some other ways you can take care of yourself:
That depends on your situation, including treatment. Ask your oncology care team to explain the kind of symptoms or issues you can expect, and when you should contact them.
Hypopharyngeal cancer can be a life-changing illness. Unfortunately, many people don’t receive a diagnosis until after the cancer has spread. At this point, you will need major surgery, followed by major lifestyle changes and lifelong follow-up.
If you have hypopharyngeal cancer, it may help to know your oncology team members will do everything they can to help you. They’ll help you understand your diagnosis and treatment options, and they’ll be there to support you as you learn to live with the changes that cancer treatment may cause. Don’t hesitate to ask for their help.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you hear that you might have throat cancer, you’ll want expert care. Cleveland Clinic’s providers can create a throat cancer treatment plan to match your needs.
