Coughing up blood (hemoptysis) involves coughing or spitting up blood mixed with mucus or spit. It can have many causes, most of which aren’t serious. Still, see a healthcare provider immediately if you cough up a lot of blood, have a cough that worsens or have additional symptoms like chest pain, blood in urine or stools, or fever.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
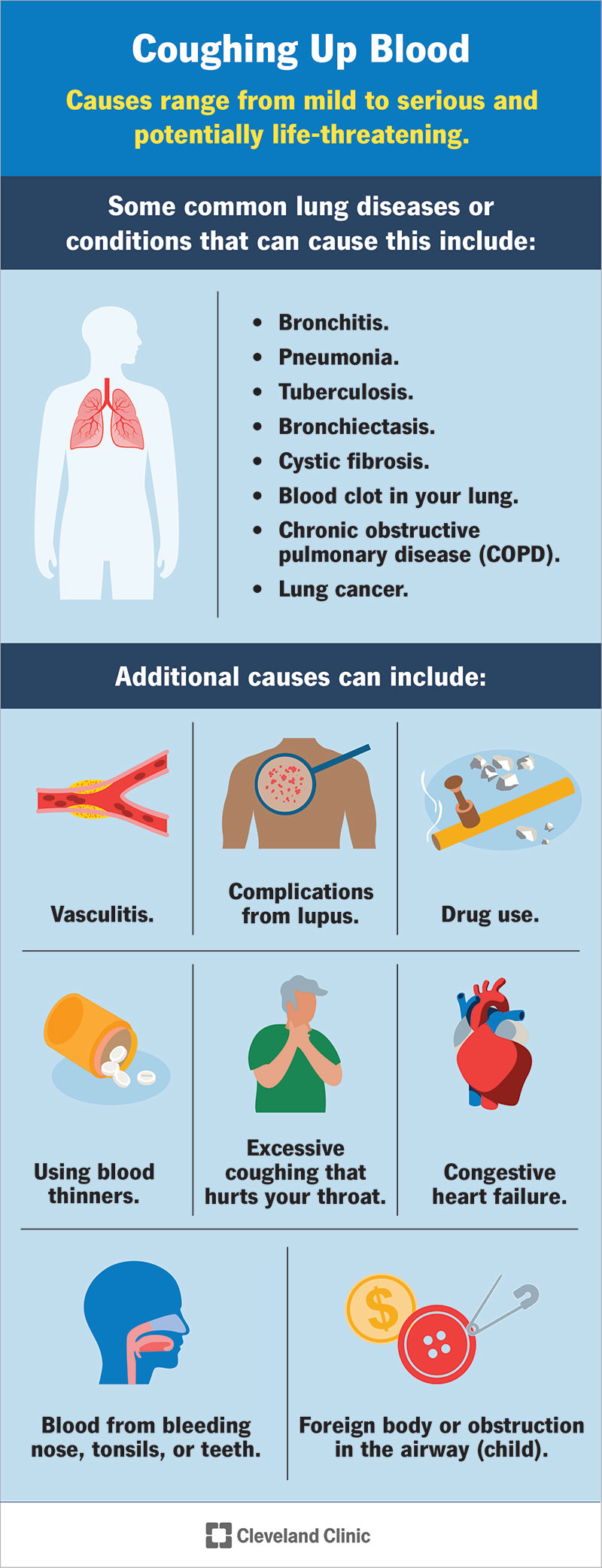
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/17696-coughing-up-blood)
Coughing up blood involves coughing or spitting up blood or bloody mucus from your lower respiratory tract (lungs and throat). Also called hemoptysis (pronounced “he-MOP-tih-sis”), coughing up blood is common and can have many causes. Most causes aren’t serious. However, you may need to visit an ER immediately if you’re coughing up large amounts of blood.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Blood that you cough up often looks bubbly or frothy and is mixed with mucus or spit. It can appear pink, red or rust-colored and is usually in small amounts.
Coughing up blood (hemoptysis) isn’t the same as vomiting blood (hematemesis). Blood that’s coughed up usually looks like blood-stained spit mixed with mucus. The blood comes from your throat or mouth. Vomiting blood involves spewing large quantities of blood. It usually involves internal bleeding in your upper gastrointestinal (GI) tract.
See a healthcare provider immediately if you’re vomiting blood.
It can be. It all depends on what’s causing your blood loss and the extent of your blood loss. Most causes aren’t serious and are treatable. Still, coughing up blood can be a sign of serious conditions, like a severe infection or lung cancer. Losing too much blood at once can be life-threatening and require emergency medical attention.
Only a healthcare provider can determine how serious your condition is. If you’re coughing up large quantities of blood, or if your condition doesn’t improve, see a provider.
Causes range from mild (most common) to serious and potentially life-threatening. Usually, coughing up blood is related to an infection. The most common causes include:
Advertisement
Other causes include:
Your healthcare provider will review your medical history, perform a physical exam and ask questions to determine what’s causing you to cough up blood. They may ask:
Your healthcare provider may also ask about behaviors that put you at risk, like drug use or smoking. They may try to identify potential causes by asking about other symptoms you’ve been experiencing.
They may perform any of the following tests to diagnose the underlying cause:
Your provider may perform additional procedures or order other tests depending on what they suspect is causing you to cough up blood.
Treatment depends on how serious your blood loss is and what’s causing you to cough up blood.
If you’re experiencing severe blood loss, you’ll receive care in the intensive care unit (ICU). Your care team will work to stabilize you and stop the bleeding before proceeding to diagnose what’s causing your blood loss.
Advertisement
Treatments for severe blood loss related to coughing up blood may include:
Once they determine what’s causing you to cough up blood, your healthcare provider will discuss the best treatment plan to address your symptoms and underlying condition.
Treatments to address conditions that may cause you to cough up blood include:
Coughing up blood can be a sign of a serious medical condition. Seek emergency care if you’re coughing up large quantities of blood.
If you're coughing up small amounts of blood for longer than a week, make an appointment with a healthcare provider. They’ll determine what’s causing your hemoptysis and get you the necessary treatment.
Seek immediate medical attention if you’re coughing up more than a few teaspoons of blood, if you’ve been coughing up blood longer than a week or if your cough is accompanied by other symptoms, including:
Advertisement
Don’t panic if you’re coughing up small amounts of blood. The most common causes are treatable. If you’re losing large amounts of blood, your condition isn’t improving and you have other symptoms, see a healthcare provider immediately. It’s important to know what’s causing this symptom so you can get the care you need. Regardless of the cause, the sooner you receive treatment, the better.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Whether you need stitches, a broken bone set or think your appendix might be causing your abdominal pain, Cleveland Clinic’s emergency medicine team is here to help.
