Fine-needle aspiration (FNA) uses a needle and syringe to get a tissue or fluid sample from a suspicious mass in your body. Healthcare providers use it to help diagnose abnormal tissue in several areas of your body, such as your breasts, thyroid and lymph nodes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
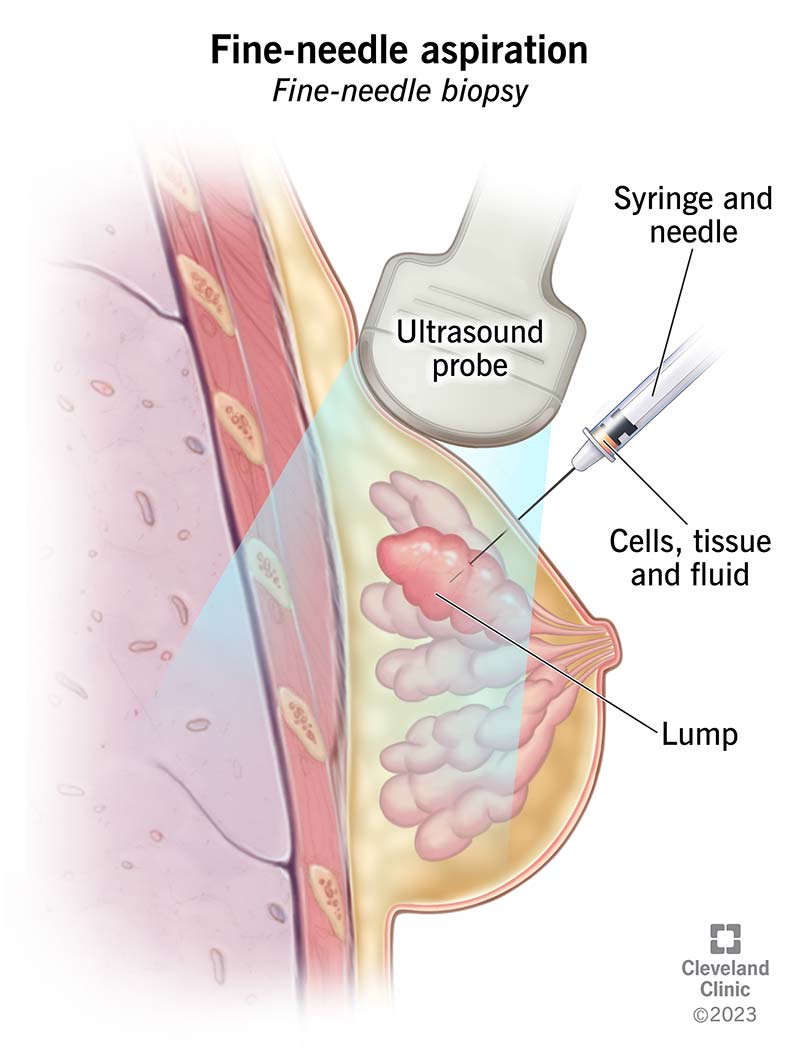
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17872-fine-needle-aspiration-fna)
Fine-needle aspiration (FNA) is a procedure healthcare providers use to get a cell sample from a suspicious lump or an abnormal area of your body. It’s also called a fine-needle biopsy. FNA involves using a thin needle and a syringe to pull out cells, tissue and fluids.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your healthcare provider then sends the sample to a cytology lab. There, a cytotechnologist screens the cells, and a specialist called a pathologist examines them for analysis. Both providers use the study of cytology to examine the cells.
FNA is the least invasive (least damaging to your body) type of biopsy, but it has limits.
A core biopsy and fine needle aspiration are both types of needle biopsies.
The needle for a core needle biopsy is wider than that used for FNA. A core biopsy gathers more tissue that can provide more information about the suspicious area than FNA can.
While FNA just involves a thin needle, a core biopsy sometimes requires a small incision to insert a spring-loaded biopsy needle.
Providers most commonly use core biopsies for breast biopsies. They use FNAs for several areas of your body.
Fine-needle aspirations have two main purposes: diagnostic and therapeutic.
Healthcare providers may also use FNAs to help guide treatment in cases where cancer has spread from the original tumor site (metastatic cancer). Pathologists can look for genetic or molecular markers in the cell samples that show if the cancer will respond better to certain cancer treatments.
Advertisement
Healthcare providers can use fine-needle aspiration (fine-needle biopsy) in any situation where a tissue or fluid sample would help with diagnosis. A pathologist looks at the collected cells under a microscope to determine their type and characteristics.
FNAs are one of several types of biopsies. Your provider may choose FNA or a different kind of biopsy, like excisional or incisional, depending on your unique situation.
Fine-needle biopsies may be necessary to assess a suspicious lump or mass. They can help diagnose:
Providers can use FNA on almost any region of your body. But providers most commonly use it to biopsy newly identified masses in your:
With the help of imaging guidance, like endoscopic ultrasound and computed tomography (CT) scan, providers can use FNA to collect tissue from deeper areas of your body, such as your:
Providers sometimes use FNAs to remove fluid from masses to help treat them, like:
They may use this technique instead of the standard incision and drainage approach in cosmetically sensitive areas, like your breast. However, FNAs can potentially spread infections, so providers can’t use them in all cases.
You usually don’t have to do anything special to prepare for fine-needle aspiration. In any case, your healthcare provider will let you know what to expect and how to prepare.
You’ll likely have an FNA in your healthcare provider’s office or a hospital as an outpatient (meaning you’re not staying overnight).
The process can vary based on which part of your body your provider is getting a sample from. But you can generally expect the following during a fine-needle aspiration:
Advertisement
Your provider will send the sample(s) to a laboratory where a pathologist will analyze it. They’ll look at the cells under a microscope and may perform other tests on the sample. The pathologist will put together a report of the findings and send it to your provider to share with you.
It’s common to have some soreness and bruising at the injection site. These are usually minor and go away within a couple of days.
Complications of fine-needle aspiration are relatively rare but can include:
There are several possible results you could get from a fine-needle aspiration. Analysis of the sample may show:
Sometimes, the laboratory may ask for additional samples to make a more accurate report. In any case, your healthcare provider will explain the report to you. Together, you’ll decide the next steps.
Advertisement
Contact your healthcare provider if you develop any symptoms of an infection, like a fever or pus or redness at the injection site. If your lump or bump changes in an unexpected way after the FNA, talk to your provider.
Finding or learning that you have a suspicious mass in your body can be stressful. The good news is that a biopsy, such as fine-needle aspiration, is the best way to know what the mass is. If you have any questions or concerns about a fine-needle aspiration procedure, don’t hesitate to talk to your healthcare provider. They’re available to help and support you.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
