Rocky Mountain spotted fever (RMSF) is a serious illness you get from a tick bite. The bacteria Rickettsia rickettsii cause it. Symptoms include a high fever and headache. Rash may start three or more days after other symptoms. RMSF can be fatal if not treated quickly with antibiotics. RMSF is found in most states in the U.S.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
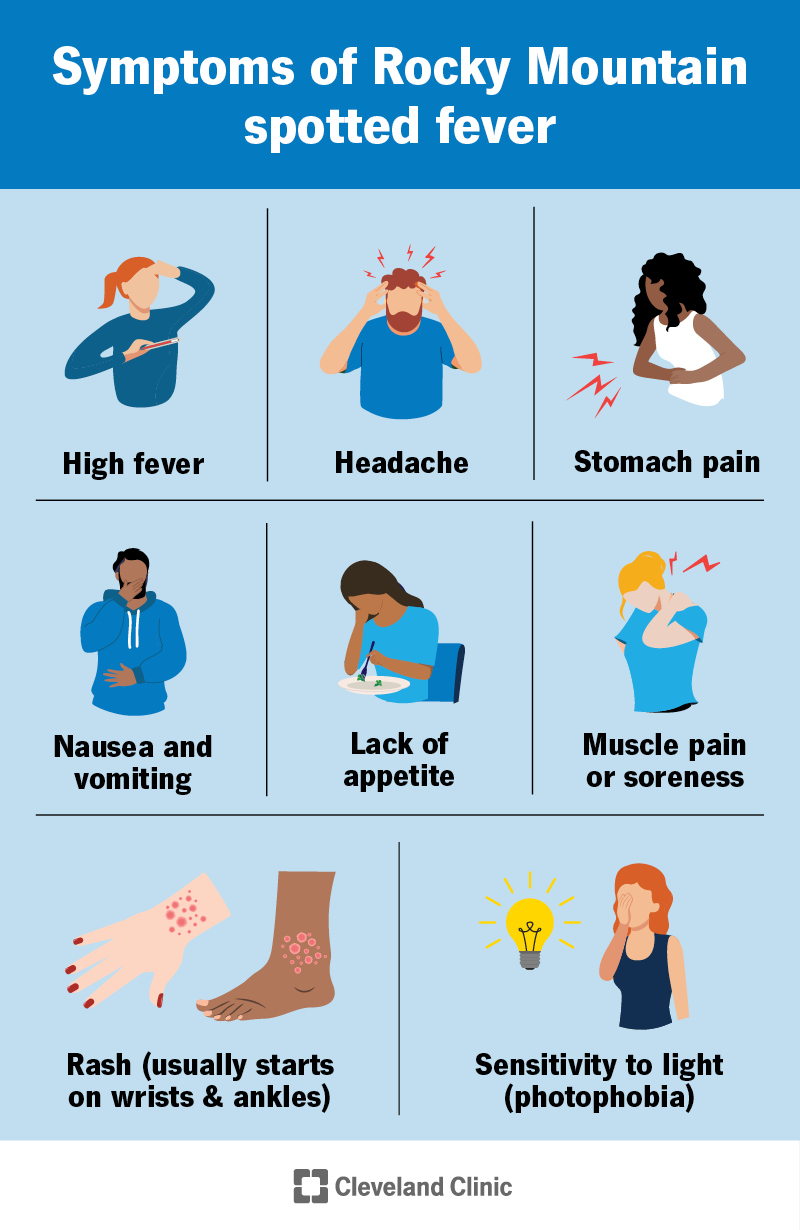
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17838-rocky-mountain-spotted-fever)
Rocky Mountain spotted fever (RMSF) is a potentially life-threatening illness you get from tick bites. The bacteria Rickettsia rickettsii (R. rickettsii) causes it.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Symptoms start out similar to many other illnesses, including headache, fever and muscle aches. If not treated right away, the bacteria attack your blood vessels, muscle cells and tissues. This can lead to leaking blood vessels, excess fluid in your tissues and damage to your muscles, nerves and organs. RMSF can be fatal or lead to lifelong health issues.
Cases of RMSF happen in the U.S., Canada, Mexico and South and Central America. Reported cases happen every month of the year. But you’re most likely to get it in warmer months, when ticks are most active.
Symptoms usually develop over a few days, starting with flu-like symptoms and getting worse. They can start two days to two weeks after an infected tick bites you.
Symptoms of Rocky Mountain fever include:
The rash is flat and appears as red, pink, purple or dark dots or splotches. It usually starts on your wrists, forearms and ankles and spreads to other parts of your body. This can appear within a few days to a week after your first symptoms start. Some people don’t get a rash at all. Don’t wait for a rash to appear to get treatment.
Advertisement
Later, more severe symptoms include:
The bacteria R. rickettsii causes Rocky Mountain spotted fever. You get it through the bite of an infected tick. In the U.S., the American dog tick and the Rocky Mountain wood tick are the main carriers. Other types of ticks, such as the brown dog tick, also carry RMSF in some places.
You’re more likely to get RMSF in the summer months, when ticks are common and people are outdoors a lot.
You’re at a higher risk for getting severely ill with RMSF if you:
Even with antibiotic treatment, some people with Rocky Mountain spotted fever have serious or life-threatening complications. These could include:
Your healthcare provider will diagnose RMSF based on a physical exam, your symptoms and whether it’s possible that you were bitten by a tick. Make sure you tell your provider if you’ve been anywhere that you could’ve encountered a tick in the past two weeks, even if you don’t remember being bitten.
Your provider can use blood and skin tests to confirm the diagnosis. But the results may not be available right away. Your provider will probably have to decide whether to treat you for RMSF before the results come back. Tests include:
Healthcare providers treat RMSF with the antibiotic doxycycline. You usually have to take it for seven to 10 days.
Treatment is most effective when it starts within five days of your symptoms appearing. If you start treatment too late, RMSF can damage your body and cause life-threatening complications.
You may need additional treatments if you’re severely ill. These could include blood transfusion, mechanical ventilation or other therapies.
If you start antibiotics soon after the symptoms of RMSF appear, you should feel better within a few days. You’ll still have to take antibiotics for several more days. Continue taking all medications as prescribed, even if you feel better. If your symptoms don’t improve, contact your healthcare provider right away.
Advertisement
If you have a tick bite or have been in an area with ticks and have symptoms of RMSF, see your healthcare provider right away. Let them know you think you could have Rocky Mountain spotted fever.
If you have a tick bite but don’t have any symptoms, you don’t need to see your provider yet. Taking antibiotics when you’re not sick won’t help prevent RMSF. Keep an eye out for any symptoms so you can get treatment right away if they start. Not every tick bite spreads RMSF.
Go to the nearest ER if you have any of these symptoms:
If you receive treatment with antibiotics within days of your symptoms starting, you’re likely to recover with no lasting issues. Some people have serious complications that need treatment in a hospital.
Even after you recover, it’s possible to have long-term health issues, especially if you were very sick. These include:
In the U.S., the fatality (death) rate for Rocky Mountain spotted fever is 5% to 10% with treatment. It’s more likely to be fatal the later you’re treated after symptoms start. The outlook is good if treated promptly. For reasons that aren’t well understood, the fatality rate is much higher in certain countries, like Mexico and Brazil.
Advertisement
You can reduce your risk of Rocky Mountain spotted fever by avoiding tick bites. Tips include:
Rocky Mountain spotted fever and Lyme disease are both infections you get from tick bites, but they’re different illnesses. RMSF can be fatal if not treated quickly. Lyme usually isn’t life-threatening.
Ticks aren’t just an annoyance — their tiny bite can make you very sick. The best way to prevent Rocky Mountain spotted fever is to avoid tick bites. But if a tick bites you and you have symptoms, contact your healthcare provider right away. Early treatment is the best way to avoid serious complications.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
