Polycystic ovary syndrome (PCOS) is a common condition that affects your hormones. It causes irregular menstrual periods, excess hair growth, acne and infertility. Treatment for PCOS depends on if you wish to become pregnant. People with PCOS may be at higher risk for certain health conditions, like diabetes and high blood pressure.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
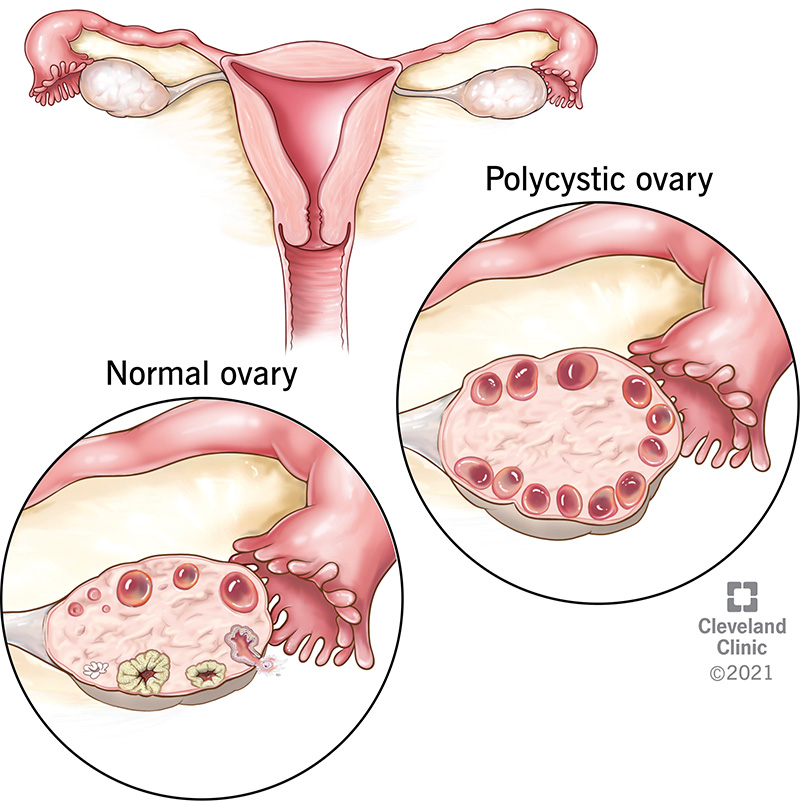
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/8316-polycystic-ovary-syndrome-pcos)
Polycystic ovary syndrome (PCOS) is a hormonal imbalance that occurs when your ovaries (the organ that produces and releases eggs) create excess hormones. If you have PCOS, your ovaries produce unusually high levels of hormones called androgens. This causes your reproductive hormones to become imbalanced. As a result, people with PCOS often have irregular menstrual cycles, missed periods and unpredictable ovulation. Small follicle cysts (fluid-filled sacs with immature eggs) may be visible on your ovaries on ultrasound due to lack of ovulation (anovulation). However, despite the name "polycystic," you don’t need to have cysts on your ovaries to have PCOS. The ovarian cysts aren’t dangerous or painful.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
PCOS is one of the most common causes of female infertility. It can also increase your risk of other health conditions. Your healthcare provider can treat PCOS based on your symptoms and if you wish to become pregnant.
Females can get PCOS any time after puberty. Most people are diagnosed in their 20s or 30s when they’re trying to get pregnant. You may have a higher chance of getting PCOS if you have obesity or if other people in your biological family have PCOS.
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_ps5rc6lt/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Learn about PCOS from Ob/Gyn specialist Erica Newlin, MD
PCOS is very common — up to 15% of females of reproductive age have PCOS.
The most common signs and symptoms of PCOS include:
Advertisement
Yes, it’s possible to have PCOS and not have any symptoms. Many people don’t even realize they have the condition until they have trouble getting pregnant or are gaining weight for unknown reasons. It’s also possible to have mild PCOS, where the symptoms aren’t severe enough for you to notice.
The exact cause of PCOS is unknown. There’s evidence that genetics play a role. Several other factors, most importantly obesity, also play a role in causing PCOS:
Having PCOS may increase your risk for certain pregnancy complications, although most people with PCOS are able to successfully carry a pregnancy. Other complications of PCOS related to pregnancy include increased risk of:
In most cases, your healthcare provider can diagnose PCOS after an examination and discussing your symptoms. They may order blood tests or perform an ultrasound to help with the diagnosis.
Your healthcare provider will:
Typically, healthcare providers diagnose PCOS if you have at least two of the three symptoms:
Advertisement
Your healthcare provider will determine treatment based on your symptoms, medical history and other health conditions, and if you want to get pregnant. Treatments can include medications, lifestyle changes or a combination of both.
Advertisement
While there isn’t a cure for PCOS, your healthcare provider can help you manage your symptoms. The effects of PCOS may change over time so that you become less aware of the condition. However, there isn’t a treatment that permanently cures it.
The hormone changes you experience during menopause often resolve the symptoms of PCOS. It doesn’t matter how old you are — if your symptoms affect your quality of life, talk to your healthcare provider.
Yes, you can get pregnant if you have PCOS. PCOS can make it hard to conceive while also increasing your risk for certain pregnancy complications, but many people with PCOS do get pregnant on their own. Your healthcare provider will work with you to develop a treatment plan to help you ovulate. Your treatment plan could include medication or assisted reproductive technologies like in vitro fertilization (IVF).
Advertisement
Talk to your healthcare provider to make sure you understand your treatment plan and how you can increase your chances of a healthy pregnancy.
Research shows PCOS may raise your risk for several health conditions, including:
Talk to your healthcare provider to make sure you understand your risk for developing these conditions.
There’s no proven way to prevent PCOS, but you can take small steps to reduce your symptoms. For example, eating nutritious foods, exercising regularly and managing a healthy weight for your body can help you avoid the effects of PCOS.
One of the best ways to cope with PCOS is to maintain a healthy bodyweight, eat nutritious foods and exercise regularly. These changes to your lifestyle can affect hormone levels, in turn regulating your menstrual cycle and easing your symptoms.
If excess hair growth or acne is hurting your confidence, cosmetic treatments or working with a dermatologist might be helpful.
Finally, if you’re trying to conceive and have PCOS, know that you’re not alone. Nearly 1 in 10 people have PCOS. Your healthcare provider will work with you to help you get pregnant if that’s what you want.
Contact a healthcare provider if you suspect you have PCOS. Some signs that may point to PCOS include:
Researchers are learning more about the causes of PCOS. However, some evidence shows PCOS has a genetic or hereditary component. This means if your biological parent has PCOS, you may be more likely to have it, too.
People with PCOS have a hormonal imbalance that disrupts their menstrual cycle, ovulation and possibly, conception. These hormones are like an intricate web and the function of your reproductive system relies heavily on its balance. The hormones that play a role in PCOS are:
PCOS and endometriosis are different conditions, but both can cause ovarian cysts and infertility. Endometriosis is a condition where the lining of your uterus (endometrium) grows in other places like your ovaries, vagina or fallopian tubes. It typically causes pelvic pain or severe menstrual cramps. People with PCOS have irregular periods, unpredictable ovulation and other physical side effects due to excess male hormones.
PCOS is a common condition that affects your menstrual cycle and causes other symptoms. Talk to your healthcare provider about your symptoms if you suspect you have PCOS. Lifestyle changes and medical treatments can help you manage the symptoms, lower your risk of other health conditions and help you get pregnant (if pregnancy is your goal).

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
The physical effects of polycystic ovary syndrome can be frustrating and challenging. Cleveland Clinic’s experts can help you manage the symptoms.
