A glioma is a cancerous (malignant) tumor that forms in your brain or spinal cord. Gliomas can affect children or adults. There are several different types. Some grow very quickly. You’ll probably need a combination of treatments, including surgery, radiation therapy and chemotherapy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
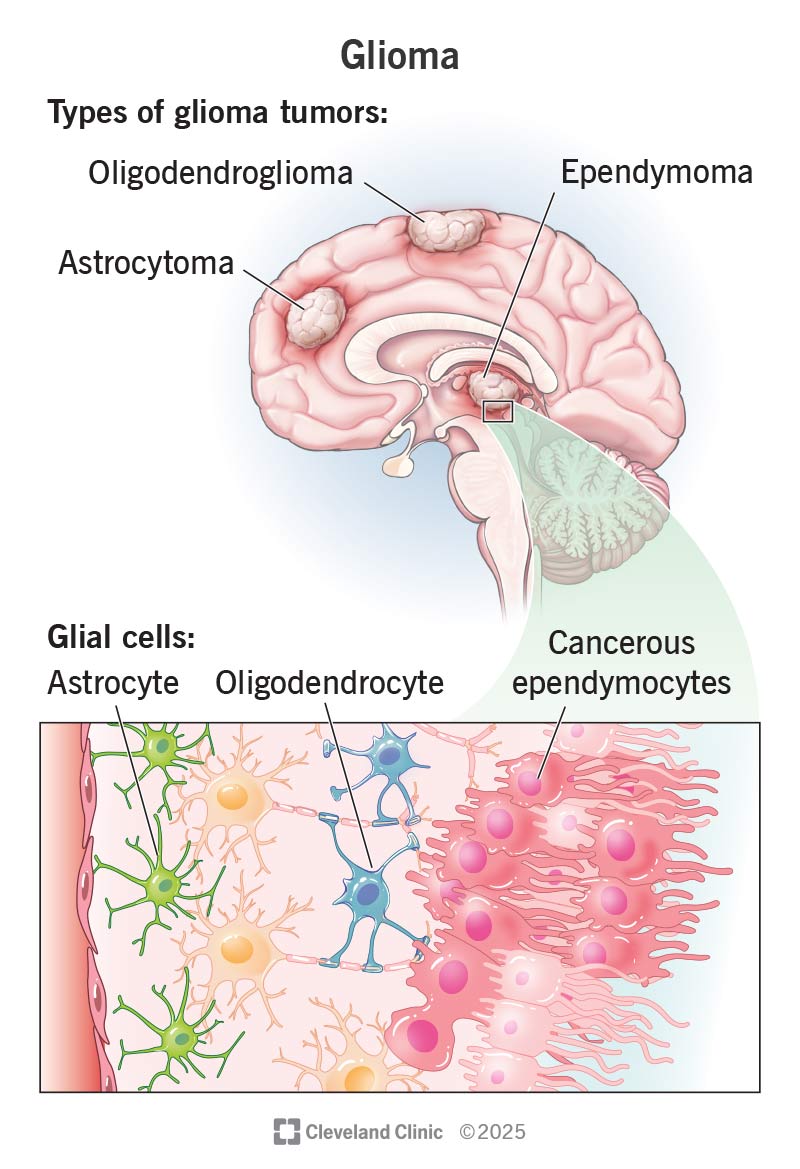
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/glioma)
A glioma is a tumor that forms when your body’s glial cells grow out of control. Glial cells support your nerves and help your central nervous system work. If they grow uncontrollably, they can form tumors in your brain or spinal cord.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Gliomas are primary tumors. This means they form directly in your brain or spinal cord. They’re serious tumors that can be life-threatening. But treatments are available to help manage the disease.
Your care team will make a treatment plan that’s unique to your body, health and needs. They’ll help you understand the best next steps.
Healthcare providers grade gliomas by how quickly they grow. They define grade by:
Four grades range from grade 1 (the slowest growing) to grade 4 (the most aggressive that grow fastest). Providers also group grades together as low (grades 1 and 2) or high (grades 3 and 4). Early detection and treatment of low-grade gliomas may slow or prevent them from becoming high-grade.
Another way to classify gliomas is by the type of glial cells they form in, including:
Advertisement
All these terms help providers communicate to each other exactly what’s happening inside your body. Your provider will help you understand everything you need to know.
A glioma can cause different symptoms depending on where it forms. Some of the most common glioma symptoms include:
Genetic changes in glial cells cause gliomas. Providers don’t always know why these changes occur.
While you can’t prevent gliomas, staying informed and seeking care early if you notice symptoms may improve outcomes.
Anyone can develop a glioma. But some factors may increase your risk, including your:
If brain or spinal cord tumors run in your biological family, you may want to consider genetic testing for cancer risk. Talk to a healthcare provider about genetic counseling.
But you don’t need to worry because most gliomas aren’t linked to clear risk factors.
A healthcare provider will diagnose a glioma by reviewing your medical history and running tests. They’ll give you a physical and a neurological exam.
You’ll need imaging tests like an MRI or a CT scan. These tests will show the tumor in your brain or spinal cord. If your provider sees signs of a tumor on imaging tests, they’ll do a biopsy. This will tell them which type of tumor it is and its grade.
Molecular testing on biopsy tissue is a standard to make a glioma diagnosis.
You may see a neuro-oncologist, a specialist in brain and spinal cord cancers, to manage this condition.
The best treatments for you will depend on a few factors, like:
You’ll need a combination of:
Surgery is often the first treatment for gliomas, when the tumor is accessible. A surgeon may be able to remove all of the tumor. But gliomas can be hard to remove completely because they may form in hard-to-reach areas.
Advertisement
A craniotomy (open brain surgery) is the most common type of removal brain surgery. If the glioma is in your spinal cord, you may need stereotactic radiosurgery or another type of spinal surgery.
Depending on the size and location of the tumor, you may be a candidate for laser ablation. This minimally invasive surgery uses heat from a laser to destroy all or part of the tumor.
You’ll probably need radiation therapy and chemotherapy (chemo) after surgery. These treatments destroy any remaining cancer cells or parts of the tumor your surgeon couldn’t safely remove.
Radiation kills cancer cells. You may get radiation from an external beam machine. It uses high-powered X-rays to target cancer.
Chemo is a group of medications your providers will give you that stop cancer cells from growing and multiplying.
Your providers might use radiation and chemo as your main treatments if it’s not safe to surgically remove the glioma.
Almost everyone has side effects from cancer treatments. Some treatments cause side effects that last for years. Ask your providers about palliative care that can help you manage glioma symptoms and treatment side effects. The most common treatment side effects are:
Advertisement
You’ll need to visit your healthcare providers for follow-up visits to monitor for any changes. Your provider will order regular imaging scans to see if the cancer spreads or comes back (recurs).
You might need physical therapy to strengthen your body during and after treatment. Your providers may suggest occupational therapy to help you adjust to changes in your body.
Survival rates for gliomas vary. It depends on the tumor type, grade and your age. Usually, the younger you are when you’re diagnosed and treated, the better the outlook.
The five-year survival rate is how many people with a type of cancer are alive five years after diagnosis.
Glioblastoma has the lowest five-year survival rate compared to other gliomas. Low-grade ependymomas, oligodendrogliomas and astrocytomas tend to have the highest five-year survival rate.
Your healthcare providers will tell you what to expect. Your case may or may not match statistics.
Living with cancer can be stressful and scary. It affects your body and your mind. Be honest with your care team about how you feel. They can help you adjust to changes in your health and daily life.
Advertisement
Support groups can help you and your loved ones cope with the challenges of a spinal cord or brain tumor. Your care team can connect you to local or online resources.
A glioma diagnosis brings changes, but you can still take steps forward. Work with your care team and focus on what helps you feel informed and cared for.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
A brain tumor diagnosis can change your life. At Cleveland Clinic, we know what it takes to treat glioma and glioblastoma and give you the support you need.
