Normal pressure hydrocephalus (NPH) is a condition that happens when cerebrospinal fluid builds up inside your skull and presses on your brain. This condition is most likely in people over 65. It’s often treatable and sometimes even reversible. Treating this condition involves surgery to implant a shunt to drain excess fluid from the inside of your skull.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
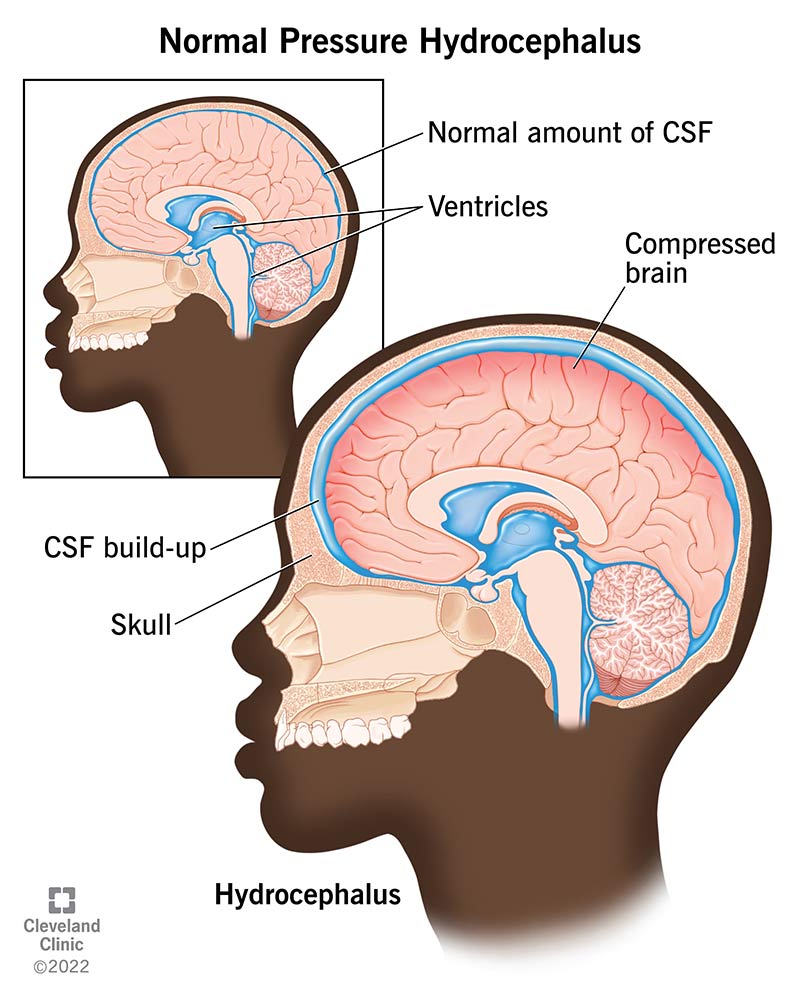
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15849-hydrocephalus-normal-pressure)
Normal pressure hydrocephalus (NPH) is a brain condition that happens when fluid buildup inside or around your brain disrupts your brain function. That can affect several brain-related abilities, including thinking and concentrating, memory, movement and more. The symptoms of NPH look very much like those of dementia, but NPH is sometimes reversible.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
NPH is most common in people over 65, becoming more and more common the older a person gets. The average age for this condition to start is around age 70.
Increasing age is the only factor that makes this condition more likely to happen. The odds of it happening don’t change depending on a person’s ethnicity, race, sex, etc.
NPH is a relatively uncommon condition but is widely known. It affects about 0.2% of people between the ages 70 and 80, and about 5.9% of people over 80. That means it affects about 8.4 million people over the age 80 worldwide. Experts estimate NPH is very rare in people under 65, only affecting about 0.003% of people in that age group.
NPH happens because of cerebrospinal fluid (CSF) buildup in your brain. CSF is a fluid that provides nutrients to and removes waste products from your brain. Adults typically only have about 5 fluid ounces (150 milliliters) of CSF, less than half the volume of liquid in a standard beverage can. Your body constantly creates, circulates and reabsorbs CSF to keep that amount of fluid constant.
While it might not seem like that much fluid, it still has a big effect. That small amount of CSF surrounds your brain and spinal cord, and your brain actually floats in it. The CSF also cushions your brain and spinal cord from outside forces. When your body can’t circulate or reabsorb CSF correctly, that can cause too much of this fluid to accumulate inside your skull.
Advertisement
With NPH, this fluid buildup usually happens gradually enough that the pressure inside your skull (intracranial pressure) increases but stays within the normal range (hence the name, “normal pressure hydrocephalus”). That’s partly because there are fluid-filled spaces inside your brain known as ventricles, which can hold some fluid buildup.
However, if CSF keeps accumulating, the fluid has nowhere else to go. When that happens, your brain starts to compress and give way, causing this condition’s symptoms. If the compression of your brain lasts too long, the pressure can permanently damage or destroy brain tissue.
The symptoms of NPH usually start gradually, developing and worsening over three to six months. The three main symptoms of NPH are known as Hakim’s triad. Between 50% and 75% of people with NPH show all three symptoms at the same time. Hakim’s triad includes three types of symptoms (with more information about each symptom type immediately below):
Gait issues are when you have trouble with walking-related movements. This is the most likely of the three symptom types to happen. About 80% to 95% of people with NPH show symptoms of this kind. Some of these symptoms may resemble movement-related symptoms of Parkinson’s disease, but a key difference is that NPH symptoms typically only affect your legs and feet.
If you have NPH, it often causes the following:
Urinary incontinence is when you lose control of your bladder, causing you to pee (urinate) unintentionally. Early on, this can cause you to need to pee often or to feel an urge to pee that’s unusually strong, difficult to control or both.
People with this symptom may feel embarrassed if they lose bladder control. However, some people don’t seem to notice or feel embarrassed by this. Not feeling embarrassed or bothered may happen because of the third type of symptom in Hakim’s triad, cognitive difficulties.
Advertisement
The third key symptom type of NPH is cognitive difficulties. This is a symptom that can appear as or cause any of the following:
There are two forms of NPH, and they happen at equal rates. The two types are:
Primary NPH means it isn’t happening because of another medical condition. Another word for this is “idiopathic,” a term experts use for conditions that happen for unknown reasons. Experts suspect idiopathic NPH can involve one or more age-related issues with how your body makes, circulates and reabsorbs CSF. About half of NPH cases are idiopathic.
Under ordinary circumstances, your body makes about 400 to 600 mL of CSF daily. That’s far more than you need, so your body constantly has to reabsorb older CSF to make room for new CSF. If there’s a problem with how CSF circulates or reabsorbs, this fluid can build up because your body is making more than it needs.
Advertisement
There’s also evidence that NPH might have a connection to degenerative brain conditions like Alzheimer’s disease, Lewy body dementia or similar conditions. Researchers are continuing to explore exactly how and why NPH happens and whether or not other conditions can contribute to it. Answers to those questions could eventually help prevent or better treat this condition.
Secondary NPH happens when another medical condition affects how your body makes, circulates or reabsorbs CSF. Some examples of conditions that can cause secondary NPH include:
NPH is often tricky to diagnose because this condition shares several symptoms with dementia and similar age-related conditions. It’s also common for NPH to happen at the same time as age-related conditions. About 30% of people with NPH also have Alzheimer’s disease or a similar degenerative brain disease.
Advertisement
A healthcare provider can diagnose NPH using a combination of the following methods:
Depending on your symptoms, your healthcare provider may recommend other tests. This is usually to rule out other conditions with similar symptoms to NPH. Your provider can tell you more about the tests they recommend and why they think those will help.
Overall, NPH is usually a treatable condition. The treatment approach varies depending on whether it’s primary/idiopathic or secondary NPH. Unlike most brain-related conditions, treating NPH rarely involves medications. That’s because NPH doesn’t respond to medications (though medications may treat some symptoms related to NPH).
Primary/idiopathic NPH is usually treatable. The most common — and most effective — treatment for idiopathic NPH is surgery to implant a device called a shunt. A shunt involves two tubes (known as catheters), one for fluid to enter and the other for fluid to flow out of, with a valve between them. If the ventricle fills with too much fluid, the increased pressure pushes fluid into the inflow catheter, opens the valve and allows excess fluid to exit through the outflow catheter.
Some modern shunt valves are programmable, letting your provider adjust the settings without surgery. They also appear on X-rays, so your provider can see the valve and make sure the settings are correct. Some modern shunts are even MRI-safe, meaning you can still undergo an MRI even if you have one of these valves.
The outflow catheter passes through a small hole in your skull (your provider makes this opening during surgery to place the shunt). After the catheter exits your skull, it turns downward, running underneath your skin. The outflow catheter lets fluid drain into your chest or your abdomen.
If the tube drains into your abdomen (which is more common), the peritoneum (a membrane that surrounds many of the organs inside your abdomen) can absorb the fluid once it leaves the drain tube. If it drains into your chest, the pleural membrane (which surrounds your lungs) absorbs the CSF.
Secondary NPH may be curable, but only if it happens because of a curable condition. The treatment for secondary NPH can vary widely depending on the underlying cause. Your healthcare provider is the best person to tell you about the possible treatments and what they recommend.
The side effects of treating NPH depend on the treatment. With primary/idiopathic NPH, the most common treatment is surgery to implant a shunt to drain any excess CSF from inside your skull. The possible side effects of that surgery include (but aren’t limited to):
With secondary NPH, the potential treatments can vary. Likewise, the side effects and complications can also vary. Because of this, your healthcare provider is the best person to tell you what kind of complications or side effects you can (or should) expect and what you can do about them.
NPH is a condition that you can’t diagnose or treat on your own. Because of that, you shouldn’t ignore the symptoms or try to care for yourself or someone else who has them.
NPH shunting tends to help relieve the symptoms of this condition fairly quickly. The odds of this are better when diagnosis and treatment happen sooner.
Most people will show improvements from shunting within hours or days after the procedure. However, placing a shunt involves major surgery, so most people will also need several days or weeks to recover from the procedure. Many factors can affect the recovery time from the surgery, so your healthcare provider is the best person to tell you about the likely timeline for recovery.
NPH is unusual among dementia-like conditions because it’s often reversible. However, the chances of reversing this condition are highest with early diagnosis and fast treatment. Delays in diagnosis and treatment make it more likely that the damage to your brain from the pressure will be permanent, severe or both.
Because NPH commonly affects your thinking abilities, many people with this condition don’t know they have it. Family, friends and other loved ones may be the ones who notice the symptoms of NPH. That means loved ones can play a key role in the early diagnosis and treatment of NPH.
NPH is a chronic (long-term) condition. The symptoms also tend to develop slowly over three to six months. However, NPH doesn't go away on its own and will continue to worsen. As it worsens, it eventually causes severe and permanent brain damage.
While NPH usually isn’t deadly on its own, it does cause symptoms that make it harder — and eventually impossible — for a person to live independently. It can also contribute to severe complications, such as falls, that can be dangerous or deadly.
With treatment, the main symptoms of NPH are likely to improve. With treatment, those three symptoms have the following probabilities of improving:
The outlook for NPH can vary widely. The reasons for that include:
A few factors make a positive NPH outcome more likely, including:
Factors that make a positive outcome less likely include:
Because so many factors can contribute to the outcome, your healthcare provider is the best person to tell you about the likely outcome for you or a loved one with this condition. The information they provide can account for medical history, the severity of symptoms, possible treatments and other important details.
NPH happens unpredictably, and half of the cases are idiopathic, meaning they happen for unknown reasons. Idiopathic NPH isn’t preventable, and you can’t reduce your risk of it happening.
However, it’s possible to reduce your risk of secondary NPH by avoiding conditions or circumstances that can cause this condition. Some things you can do include:
If you have NPH, the most likely treatment you’ll receive is surgery to place a shunt to keep fluid from building up inside your head. If you have a shunt, there are a few things you’ll typically need to do to help avoid any issues:
You should see your healthcare provider as recommended. You should also see them if you notice any symptoms of NPH returning or if you experience new symptoms (even ones that don’t seem related).
Your healthcare provider can tell you about symptoms that indicate possible problems or complications. Some of the symptoms that most likely need quick medical attention include:
There may be other signs and symptoms you’ll need to watch for, and your healthcare provider can tell you more about these. They’re also the best ones to answer questions about what you can do to avoid these issues.
NPH is hydrocephalus that happens slowly and gets worse over time. The term “normal pressure” means that the pressure inside of your skull (intracranial pressure, or ICP) isn’t unusually or dangerously high. In these circumstances, your ICP levels are more likely to be at the high end of the expected range. This happens slowly, compressing and crowding your brain tissue. The pressure stays relatively normal because your brain has time to give way to the fluid, which eventually causes symptoms.
Normal pressure hydrocephalus (NPH) is a rare condition that most often affects people over age 65. This condition can happen for idiopathic (unknown) reasons or due to another condition, such as an infection like meningitis or an injury to part of your brain. This condition causes dementia-like symptoms, affecting walking, thinking and your ability to control when you pee (urinate).
Most dementia-like conditions only get worse over time and are difficult to treat and manage. However, NPH is often treatable or even reversible. Chances of reversing the effects of NPH are best with early diagnosis and treatment. Because of this, it’s important not to ignore the symptoms in yourself or a loved one. With prompt care, many people with NPH can recover and regain most — if not all — abilities they had before developing this condition.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Hydrocephalus in children can be serious. And you want your child to have the best care. Cleveland Clinic Children’s is here for them — and you.
