Brachytherapy (internal radiation therapy) treats prostate, breast and other cancers. Healthcare providers place tiny radioactive pellets inside or near a tumor. The pellets release radiation that destroys cancer cells. The treatment spares surrounding healthy tissue. Brachytherapy is an effective treatment for tumors that haven’t spread.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
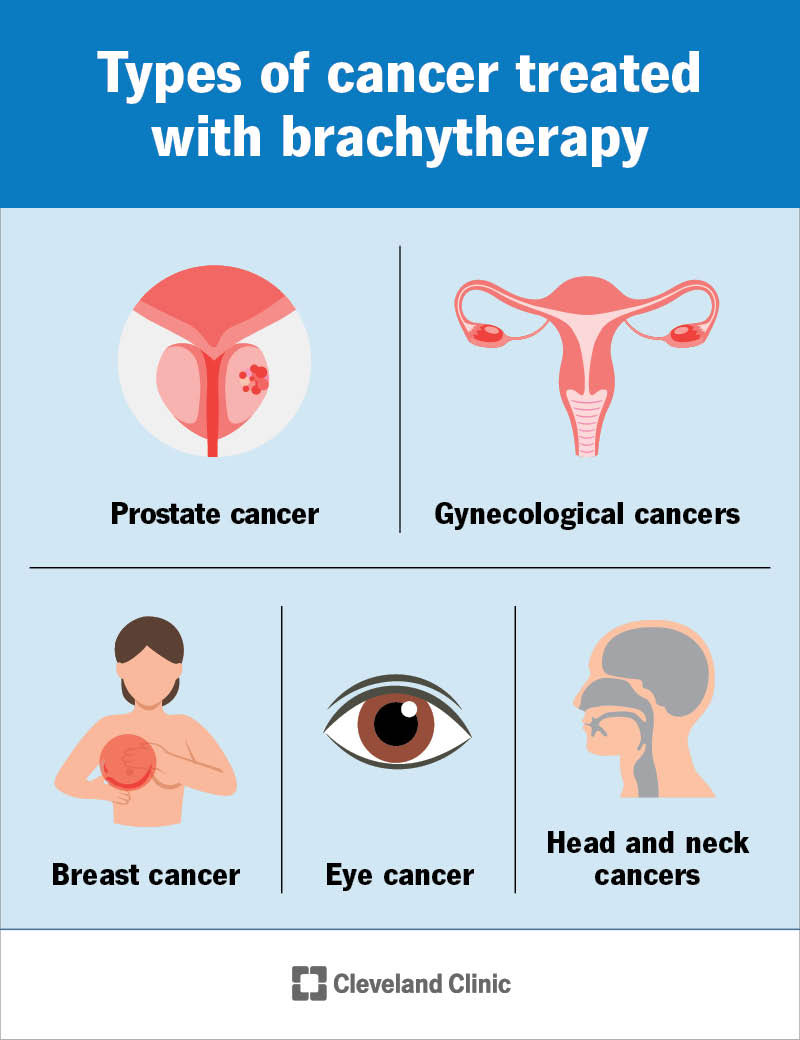
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/brachytherapy)
Brachytherapy (pronounced “bray-kee-THEH-ruh-pee”) is a form of radiation therapy that treats various cancers. Treatment involves placing radioactive seeds, or pellets, capsules or other implants inside or near a tumor. The implants give off radiation for a short time.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Brachytherapy can deliver large amounts of radiation that shrink or destroy tumors while sparing healthy surrounding tissue. You may only need brachytherapy. Or you may get it alongside other cancer treatments, like external beam radiation therapy (EBRT) or surgery.
Brachytherapy is also called internal radiation therapy.
Types of brachytherapy include temporary and permanent implants.
Low-dose rate (LDR) brachytherapy
LDR implants release low doses of radiation continually for one to seven days. Then, a provider removes them.
High-dose rate (HDR) brachytherapy
HDR implants release high doses of radiation during treatment sessions that last for 10 to 20 minutes. Providers remove them at the end of each session. Sessions vary from twice a day for up to five days to once a week for up to five weeks.
These implants release low doses of radiation continually over several weeks or months. The level of radioactivity decreases over time until the implant becomes inactive. The implants remain in your body. This treatment is also called “seed implantation.”
Brachytherapy is effective at destroying tumors that haven’t spread. Brachytherapy treats:
Advertisement
Your healthcare provider will do a physical exam and review your medical history. You may also need blood tests and imaging procedures to help your provider plan treatment.
Your healthcare provider will explain things you should do leading up to brachytherapy. Depending on your situation, you may need to:
The procedure depends on the cancer and the type of brachytherapy (LDR, HDR or permanent). It also depends on where the radiation oncologist places the implant:
If appropriate and necessary, you’ll receive medicines, like anesthesia, to prevent pain during brachytherapy. Once you’re comfortable, the radiation oncologist will:
If appropriate, you’ll receive pain medicine to ease any discomfort once it’s time to remove the catheter or applicator device.
Brachytherapy procedures take anywhere from 30 minutes to a few hours. How long the treatment lasts in total depends on the type of brachytherapy:
Advertisement
After the procedure, healthcare providers will take you to a recovery room. They’ll monitor you and help manage any pain.
You may get to go home on the same day as your procedure. If you do, you’ll need someone to drive you if you received pain medications or anesthesia as part of your procedure. Or, you may need to stay in the hospital overnight to recover from the procedure. Sometimes, you’ll stay in the hospital if you have treatments spread out over several daily sessions.
Brachytherapy is an effective cancer treatment for localized tumors. The implants give off a powerful dose of radiation that blasts tumors without harming healthy tissue away from tumors. Less damage means there’s a reduced risk of side effects related to radiation exposure. The recovery time for brachytherapy can be shorter than some other types of cancer treatment.
Brachytherapy is a successful treatment for tumors that haven’t spread. For example, a recent study shows healthcare providers are increasingly using brachytherapy to help people with cervical cancer live longer. Research also shows that in some cases, brachytherapy can get rid of prostate cancer and keep it from coming back.
Still, no two cancer diagnoses are the same. Ask your healthcare provider about the likely outcomes of brachytherapy treatment based on your unique diagnosis.
Advertisement
Potential side effects depend on the cancer type and the type of brachytherapy you receive. Side effects typically improve once the radiation leaves your body. But some are long-term or don’t appear until after treatment ends.
Potential side effects include:
Usually, side effects occur in the body part where the implant is. For example, with a prostate gland seed implant, you may experience symptoms impacting how you pee or poop, but not nausea and vomiting.
Brachytherapy may involve a shorter recovery time than other cancer treatments, like surgery. Depending on the procedure, you may feel better within a few days up to a week.
You may need to limit your activity and get extra rest after treatment. Follow your healthcare provider’s guidance on when it’s safe to return to your usual routine.
Follow your provider’s instructions on how to interact with others safely after brachytherapy. For example, if you have permanent brachytherapy, you may expose other people to radiation for several weeks or months. The exposure risk is small. But you should limit your contact with young children and pregnant women as directed by your healthcare provider. With temporary brachytherapy, there isn’t any exposure to other people around you.
Advertisement
Still, it’s important to know that the radiation the implant releases doesn’t usually travel beyond the tumor. This is why it kills tumors without harming nearby tissue.
Call your healthcare provider if you experience any of the following symptoms during or after treatment:
Brachytherapy places radiation close to a tumor to destroy it. The good news is that it spares healthy tissue from harmful radiation exposure. It’s also excellent at treating local tumors, like those found in prostate, cervical and uterine cancer.
Follow your healthcare provider’s guidance about caring for yourself and managing any side effects of brachytherapy. Ask about likely outcomes based on your treatment timeline.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you’re diagnosed with cancer, you want expert and compassionate care right away. At Cleveland Clinic we personalize your treatment to match your needs.
