Aphasia is a language disorder that affects your ability to speak and understand what others say. You might have trouble reading or writing. It usually happens suddenly after a stroke or traumatic brain injury. Treatment options are available to help you adapt if symptoms are permanent.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
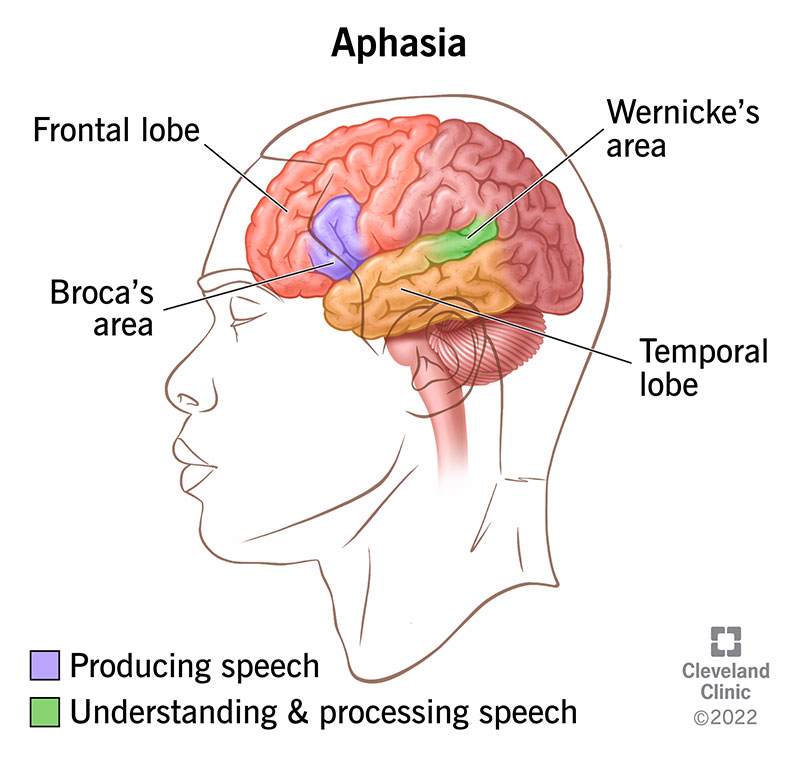
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/aphasia)
Aphasia is a disorder that affects how you communicate and understand language. It makes it difficult to:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You might think about the challenges you’d face trying to communicate when traveling to another country. But what if the language you use every day suddenly becomes foreign? You might not be able to ask for a glass of water if you’re thirsty. You wouldn’t be able to understand a story that your friend is telling you. And frighteningly enough, you wouldn’t be able to tell someone that you’re hurt. For many people, this is what it might feel like to have symptoms of aphasia.
This condition happens after damage to the language center of your brain, usually after a stroke. It can also happen with conditions that disrupt how your brain works. The effects of aphasia can be temporary, like during a migraine, or more long-lasting, after a traumatic brain injury.
While aphasia affects your ability to communicate, it doesn’t affect your intelligence. Treatment options are available to help you communicate and better understand different forms of language.
There are multiple types of aphasia, including:
Advertisement
In the United States, an estimated 180,000 people are diagnosed with aphasia each year. This equals about 1 in every 272 people.
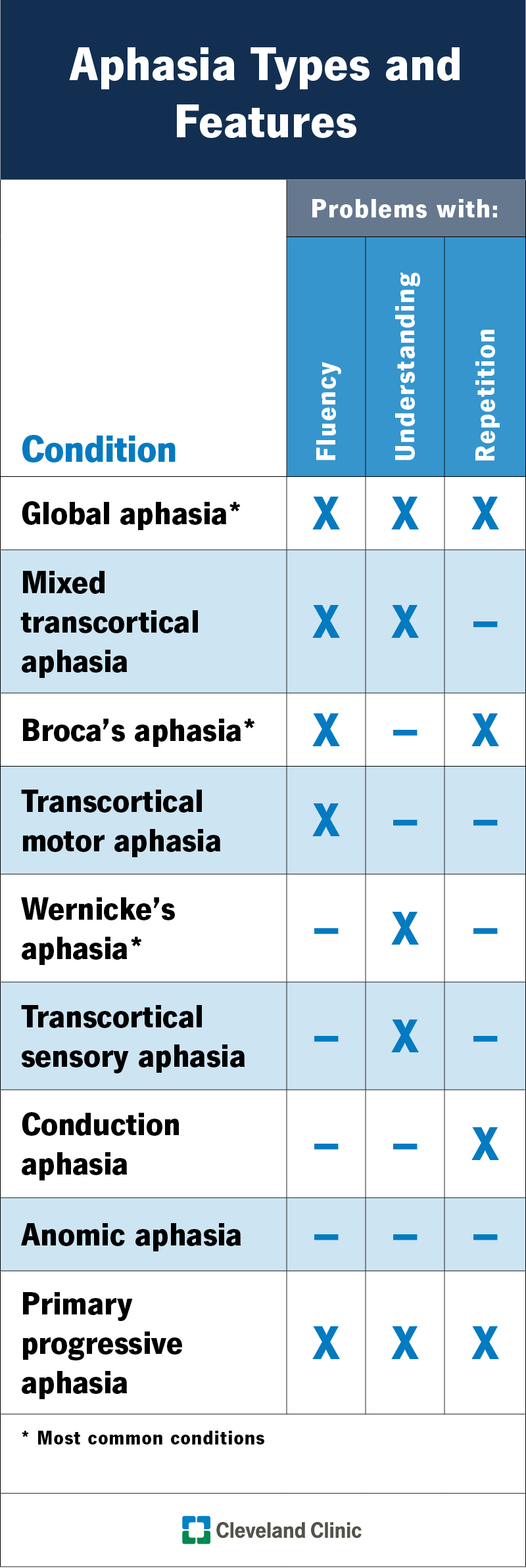
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/aphasia-table-final)
The symptoms of aphasia vary based on what type you have. However, most types cause difficulty in finding, understanding and recognizing different forms of language:
Damage to the language center of your brain (areas of your brain involved in language) causes aphasia. The most common causes of aphasia include:
Aphasia can happen with any condition that damages your brain. It can also happen with problems that disrupt how your brain functions. Other possible causes include:
The location of the damage in your brain determines the type of aphasia you have. There are two main parts of your brain that involve language, including:
These two areas of the brain work together to help you speak. Wernicke’s area processes your understanding of words and picks which ones you use. Then, it sends signals to Broca’s area. Once Broca’s area knows what words to use, it sends the signals to the muscles you use when you speak.
Advertisement
Aphasia can affect anyone at any age. It’s more common after age 65, especially after a stroke, event or condition that damages your brain. Aphasia can happen suddenly after these events.
Aphasia affects your ability to communicate your wants and needs. You might not be able to tell someone you’re hungry or tired, that you need help or something’s wrong. This can lead to:
Because there’s a language barrier, caregivers may also feel frustrated and upset that they can’t effectively communicate with their loved ones.
A healthcare provider will diagnose aphasia after a physical exam and testing. During the exam, your provider will ask you questions about your health history and symptoms. It can be difficult for you to answer these questions or understand what your provider is asking you. It helps to have a caregiver or loved one with you during your exams to help fill in the blanks if you need it.
If your provider suspects aphasia, they may refer you to a speech-language pathologist (SLP). A speech-language pathologist will offer a comprehensive exam to learn more about your ability to understand language (listen), speak and hold a conversation, express your thoughts, read and write. This helps your provider determine what type of aphasia you have.
Advertisement
Your provider will also evaluate the following factors to make a complete diagnosis:
Your provider will recommend running several tests to diagnose aphasia or rule out conditions with similar symptoms. The tests may even determine what kind of treatments will work best.
Testing may include:
Your healthcare provider will treat the underlying cause of aphasia to manage your symptoms. For example, if you experienced a stroke, quickly restoring blood flow to the affected area of your brain can sometimes limit or prevent permanent damage. The aphasia usually gets better as you recover and your brain heals.
Some causes of aphasia don’t need treatment, since they’re temporary, like with concussions or migraines.
Advertisement
If you have long-term or permanent brain damage, speech therapy can improve your language abilities. Speech therapy builds or rebuilds your understanding of language and teaches you skills to adapt to specific symptoms. Speech therapy can also involve caregivers and loved ones, so they know how best to communicate with and help you.
Medications may help treat the cause of aphasia. These vary widely. Your healthcare provider will recommend possible treatments specific to your situation. They’ll also consider any underlying health conditions or preferences that might impact your care.
The time it takes to recover from aphasia depends on what caused it, how severe it is and available treatment options. Your healthcare provider is the best person to tell you more about your recovery timeline.
In some cases, aphasia is short-term and will go away completely over time. For others, aphasia may be a lifelong condition if the language center of your brain has permanent damage. Speech therapy may improve aphasia symptoms but can’t fully reverse this condition’s effects.
The outlook for aphasia depends on several factors like your general health and what caused your symptoms. Your healthcare provider will explain more about your outlook, specifically.
Aphasia happens unpredictably, so it’s not possible to prevent it. However, you can try to reduce your risk of developing conditions that cause it. Some of the things you can do include:
Aphasia may make some everyday tasks more difficult, but it doesn’t have to take over your life. Here are some ways that you can take care of yourself:
Your provider can give you additional recommendations specific to your situation.
If you gradually notice you have symptoms of aphasia, you should talk to a healthcare provider as soon as possible. You should also talk to your provider if you have aphasia symptoms that get worse over time.
If aphasia symptoms appear suddenly, you should get emergency medical attention. When aphasia symptoms happen quickly or without warning, it can be a sign of a stroke, for example. You should call 911 (or your local emergency services number) immediately.
You should also get help if you notice any of the symptoms of stroke (regardless of whether or not they happen along with symptoms of aphasia) in yourself or someone near you. Those symptoms include:
There are several conditions that involve or look like aphasia. But these conditions have different underlying causes and symptoms. Other conditions may include:
It can be a scary and frustrating experience to receive an aphasia diagnosis. The language skills you once mastered need to be relearned. You may find it difficult to participate in a monthly book club or give a presentation at work after an event like a stroke or brain injury. This can significantly impact your mental health and your ability to socialize.
While aphasia might go away on its own, it’s sometimes a permanent condition. Your healthcare providers can help you adapt and learn new ways to communicate and build or reestablish a connection with others.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a neurological condition, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
