Kaposi sarcoma is a rare type of soft tissue sarcoma. It causes cancerous spots on your skin and in the tissue that lines your GI tract. You’re more likely to develop it if you carry human herpesvirus 8 (HHV-8) and have a weakened immune system. Healthcare providers can treat Kaposi sarcoma, but it may come back.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
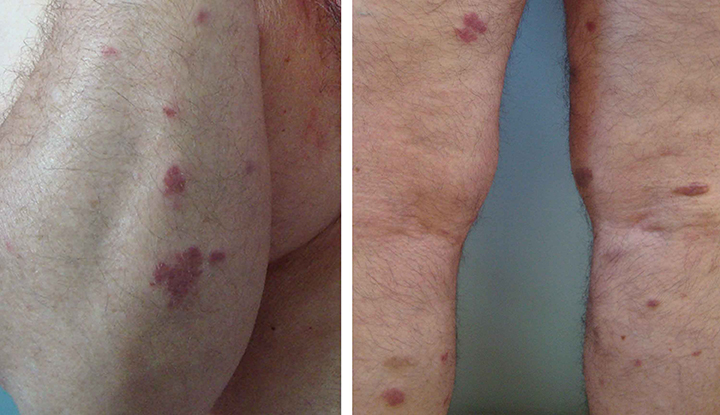
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/21830-kaposi-sarcoma)
Kaposi sarcoma (KS) is a type of soft tissue sarcoma. It causes lesions that can form on your skin or mucus membranes that line the inside of your mouth, nose and anus. These tumors may also develop in the lining of internal organs like your liver, belly and lungs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You can get KS if you carry human herpesvirus 8 (HHV-8) and have a weakened immune system. KS is rare. Fewer than 5,000 people living in the United States have it.
There are four types of Kaposi sarcoma. From most to least common, they are:
Kaposi sarcoma symptoms can vary depending on the location of the lesions. You might develop:
Advertisement
Kaposi sarcoma happens when HHV-8 infects the cells that line your blood and lymphatic vessels. HHV-8 is a rare disease that turns healthy cells into cancerous cells. Certain factors increase the risk of HHV-8 becoming Kaposi sarcoma.
Risk factors for Kaposi sarcoma include:
Kaposi sarcoma can lead to complications, which may include:
A healthcare provider will start with a physical examination. They’ll check your skin for lesions and ask about your symptoms and health history.
Because Kaposi sarcoma is so rare, it can take a while to get an accurate diagnosis. You may need to see several different types of healthcare providers and specialists. Ask your care team what to expect in your situation.
To get an accurate diagnosis, your healthcare provider will need to run tests, which may include:
It depends on your situation. Your healthcare team will create a personalized plan unique to you. Treatments may include:
Advertisement
The treatment that’s right for you depends on a few different factors, like the type of KS you have, the number and location of lesions, and your overall health. Your oncologist can tell you what to plan for in your case.
Kaposi sarcoma can come back (recur) after treatment. So, you’ll have regular follow-ups so your healthcare provider can monitor your health and check for signs of new cancer.
If you’re living with HIV/AIDS or have had an organ transplant, your regular check-ups will include screenings for recurring KS.
Your outlook depends on many factors. But like most cancers, early detection and treatment give you the best chance for long-term survival.
The overall five-year survival rate for Kaposi sarcoma is 75%. That means that 75% of people who have KS are still alive five years after their diagnosis.
Keep in mind that cancer survival rates are only estimates. They can’t predict how long you’ll live or how well you’ll respond to treatment. To learn more about survival rates and what they mean for you, talk to your healthcare provider.
If you have Kaposi sarcoma, maintaining a healthy immune system is the best thing you can do to take care of yourself. You can support your immune system by:
Advertisement
According to the American Cancer Society, taking steps to reduce your HIV risk may help prevent Kaposi sarcoma.
If you have HIV, highly active antiretroviral therapy can reduce your risk of developing Kaposi sarcoma and AIDS.
Talk to your healthcare provider if you have HHV-8. There are immunosuppressant medications that protect your transplanted organ without increasing your risk of Kaposi sarcoma.
Kaposi sarcoma isn’t an autoimmune disease. It’s a type of cancer that usually affects people with weakened immune systems.
In other words, it happens when your immune system is already weak, not when your body attacks its own tissues.
Kaposi sarcoma (KS) is a complicated illness that affects different people in different ways. It can come back years later, even after treatment. It might help to know that there are several therapies that can lessen your symptoms. It’s important to stay in close communication with your healthcare provider. Ask them for personalized recommendations.
Advertisement
You may also want to join a local or online support community. Talking with others who have shared experiences can help you process your emotions and make health decisions you can feel good about.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Sarcomas are a rare form of cancer affecting your bones and soft tissues. Our specialists use the latest treatments to care for these types of tumors.
