Brachioradial pruritus is a neurological condition that causes itchiness and other abnormal sensations in your forearms. A combination of cervical radiculopathy and ultraviolet radiation exposure causes it. There’s a variety of treatment options, including avoiding sun exposure and oral and topical medications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
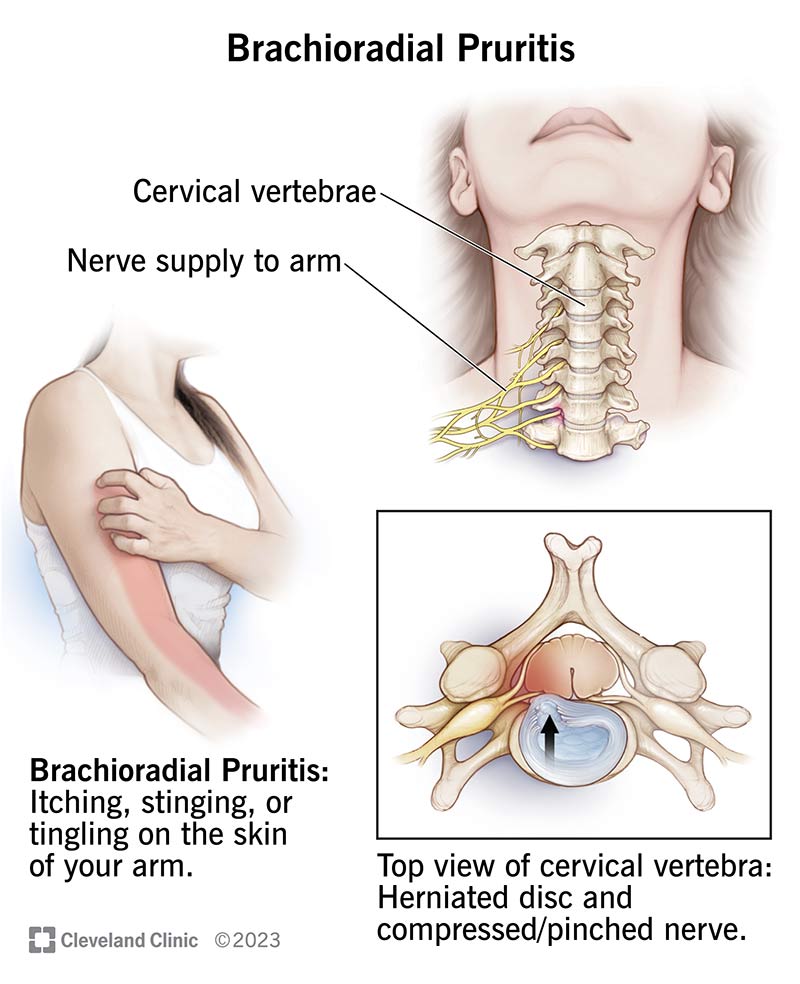
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21181-brachioradial-pruritis)
Brachioradial pruritus is a nerve condition that causes itching, stinging or tingling sensations in your outer forearm. It isn’t a rash or a contagious condition.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Brachioradial” refers to the brachioradialis muscle in the lower part of your arm that helps it bend at your elbow. “Pruritus” is the medical term for itching.
Brachioradial pruritus usually affects both arms, but it can occur in only one arm.
Irritation of your cervical nerves can lead to brachioradial pruritus. In your neck (cervical spine), you have eight pairs of spinal nerves labeled C1 to C8. These nerves supply sensation to your neck, shoulders, arms and hands. Irritation of any of the nerves between C5 and C8 can cause brachioradial pruritus.
The main sign of brachioradial pruritus is itchiness on your outer forearm. The condition doesn’t involve a skin rash, but you may develop marks or skin discoloration from excessive scratching.
You may also have itching on your:
Some people also experience the following sensations in the affected area:
In 75% of cases, the itching and other sensations affect both arms. But it can also affect just one arm.
Researchers believe a combination of cervical radiculopathy and ultraviolet (UV) radiation causes brachioradial pruritus.
A pinched nerve in your neck (cervical radiculopathy) can cause abnormal sensations (paresthesia) in various parts of your upper body, including your arms. You may feel tingling, numbness, pain and itching.
Advertisement
Several spinal issues can lead to a pinched nerve in your neck, including:
People with brachioradial pruritus often don’t realize they have a pinched nerve in their neck because they often don’t experience pain from it. However, studies show that neck imaging tests of people with brachial pruritus show evidence of spinal issues and pinched nerves.
Researchers aren’t exactly sure why, but they believe UV (ultraviolet) radiation is a contributing factor to brachioradial pruritus because:
Sun exposure typically triggers flare-ups of brachioradial pruritus. The symptoms are often worse after being outside without sun protection.
Risk factors for brachioradial pruritus include:
A healthcare provider will ask you about your symptoms, medical history and lifestyle. They’ll perform a physical exam and assess your arms to be sure you don’t have a rash that’s causing the itching.
Providers can usually diagnose brachioradial pruritus with the ice pack test. Your provider will place an ice pack on the affected area. If your symptoms immediately stop and then return once your provider removes the ice pack, it usually means you have brachioradial pruritus.
In rare cases, your provider may recommend imaging tests to assess your cervical spine and spinal nerves, such as an MRI scan or X-rays.
In most cases, a primary care physician (PCP) can diagnose brachioradial pruritus and recommend treatment.
But they may refer you to a neurologist if your case is severe or there may be other underlying neurological issues.
Treatment methods for brachioradial pruritus include:
Using ice packs on the affected area can also alleviate symptoms temporarily.
In very rare cases, healthcare providers may recommend surgery to correct cervical spine conditions.
Methods of avoiding UV radiation include:
Advertisement
Healthcare providers most commonly prescribe an oral tricyclic antidepressant called amitriptyline for brachioradial pruritus. This is because tricyclic antidepressants are known to help treat nerve issues, like neuropathic pain.
Other oral medications include:
Topical medications (like creams and lotions) for brachioradial pruritus include:
For many people with brachioradial pruritus, symptoms go away in a few weeks to a few months after taking medication and reducing exposure to sunlight.
For some, the itching and burning sensations come and go for the rest of their lives. In many cases, healthcare providers can successfully manage these flare-ups.
Many people with the condition find that symptoms improve during the winter months.
Some people with brachioradial pruritus experience skin complications due to excessive scratching. They include:
There’s no known way to prevent brachioradial pruritus. But you can reduce your risk of developing the condition by protecting your skin from exposure to sunlight and UV radiation. Wear protective clothing when you go outside. Always use sunscreen with a sun protection factor (SPF) of at least 30.
Advertisement
Contact your healthcare provider if you feel a constant urge to scratch your arms or experience other signs of brachioradial pruritus.
If treatment isn’t helping your symptoms, reach out to your provider for other options.
If you have brachioradial pruritus, you may want to ask:
Brachioradial pruritus is a nerve condition that causes itching and other abnormal sensations in your forearm. While this condition isn’t a danger to your health, it can cause unpleasant and uncomfortable symptoms. If brachioradial pruritus is interfering with your quality of life, talk to a healthcare provider. They can recommend treatments and answer any questions.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
