Cervical radiculopathy (also known as “pinched nerve”) is a condition that results in radiating pain, weakness and/or numbness caused by compression of any of the nerve roots in your neck. Most cases of cervical radiculopathy go away with nonsurgical treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
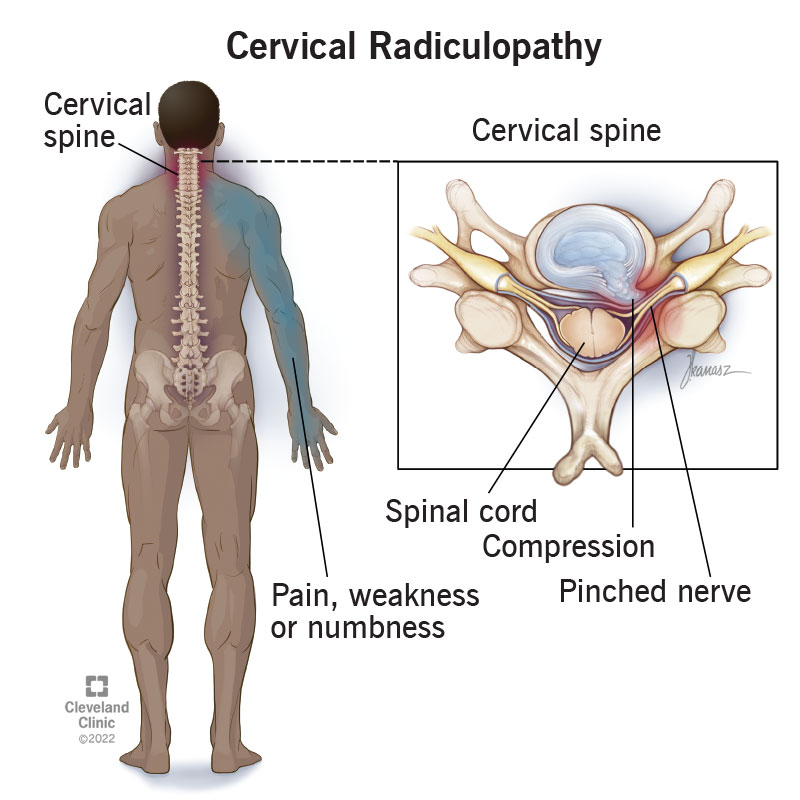
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22639-cervical-radiculopathy)
Cervical radiculopathy (also known as “pinched nerve”) is a condition that results in neurological dysfunction caused by compression and inflammation of any of the nerve roots of your cervical spine (neck). Neurological dysfunction can include radiating pain, muscle weakness and/or numbness.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Cervical” comes from the Latin word “cervix,” which means “neck.” In the case of cervical radiculopathy, the issue is in your neck, not your cervix. (The cervix, the narrow passage forming the lower end of the uterus, is called so because it’s a neck-like passage.)
Your spine (backbone) is the long, flexible column of bones that protects your spinal cord. It begins at the base of your skull and ends in your tailbone at your pelvis. Your cervical spine is the neck region of your spine. It consists of seven bones (C1-C7 vertebrae).
Vertebrae help protect your spinal cord from injury. Between your vertebrae in your spine are round cushions called disks. They have soft, gel-like centers and a firmer outer layer, like a jelly doughnut. These disks provide cushioning for your vertebrae and flexibility for you.
Your spinal cord acts like a highway that connects the nerves located all over your body to your brain so that your brain can send signals and communicate with the rest of your body. A nerve root is the initial segment of a nerve that leaves your spinal cord. It’s the root for the nerves that extend out to other parts of your body. Different nerve roots along your spine extend to different parts of your body.
Advertisement
When a nerve root becomes pinched, it can affect the nerves that are attached to it. This is why a pinched nerve (cervical radiculopathy) in your neck can cause pain that radiates down your arm.
Anyone can get cervical radiculopathy, but it’s more common in adults.
Cervical radiculopathy caused by a herniated disk is more common in people up to 50 years old. And cervical radiculopathy caused by disk degeneration is more common in people in their 50s and 60s.
People in their 70s or older tend to get cervical radiculopathy from foraminal narrowing as a result of arthritis. The foramen is the bony hollow opening between vertebrae through which spinal nerve roots travel.
Cervical radiculopathy is somewhat common. Cervical radiculopathy affects approximately 85 out of 100,000 people. In over half of cervical radiculopathy cases, the C7 nerve root is affected. Approximately a quarter of cases affect the C6 nerve root.
The nerves that connect to your cervical spine (neck) extend out to your following body parts:
Because of this, the neurological symptoms that result from cervical radiculopathy can radiate down from your neck to any one of or a combination of these body parts, depending on which nerve root is affected. Cervical radiculopathy typically only affects one side of your body — for example, your right arm, not both arms.
Neurological symptoms from cervical radiculopathy that can radiate down from your neck include:
Cervical radiculopathy affects people differently. You may have any combination of the above neurological symptoms or only one.
People with cervical radiculopathy typically describe the pain as sharp or burning. Moving your neck in certain ways, like extending or straining it, may increase the pain.
Some people with cervical radiculopathy notice that their pain decreases when they place their hands on top of their head. This may temporarily relieve pressure on the affected nerve root.
Cervical radiculopathy happens when a nerve root in your neck (cervical spine) becomes compressed (pinched) and inflamed.
This compression has two main causes:
The majority of cases of cervical radiculopathy are due to cervical spondylosis.
Cervical spondylosis is a general term for age-related wear and tear (degenerative changes) in your cervical spine (neck) that can lead to neck pain, neck stiffness and other symptoms. Sometimes, this condition is called arthritis or osteoarthritis of the neck.
Advertisement
As you age, the disks in your spine between your vertebrae lose height and begin to bulge. They also become less jelly-like and become stiffer. This problem causes the collapse of the disk spaces and loss of disk space height.
As the disks lose height, your vertebrae move closer together. Your body responds to the collapsed disk by forming more bone — called bone spurs (osteophytes) — around the disk to strengthen it. These bone spurs can narrow the foramen — the small openings on each side of your spinal column where the nerve roots exit — and pinch the nerve root. This is called foraminal stenosis. The pinched nerve root causes cervical radiculopathy.
Through aging or an injury, the outer layer of a vertebra disk can weaken and crack. A herniated disk happens when the inner “jelly” substance of the disk pushes through the crack.
A herniated disk causes cervical radiculopathy when the leaked material from a disk in your neck presses on nearby spinal nerves.
Several factors can contribute to a cervical herniated disk, including:
Advertisement
Cervical radiculopathy caused by a herniated disk is more common in people up to 50 years old.
You’ll want to visit your healthcare provider about your pinched nerve if it’s not responding to conservative treatment at home.
Your healthcare provider will ask about your:
They’ll then examine your neck, shoulder, arms and hands. They’ll look for muscle weakness, check for changes in reflexes and ask about the different sensations you’re feeling. Since cervical radiculopathy almost always affects one side of your body (is unilateral), your healthcare provider will compare the sensations you feel on one side of your body to your other side.
Your healthcare provider may also ask you to perform certain neck and arm movements to try to recreate and/or relieve your symptoms.
Cervical radiculopathy can be difficult to diagnose, as many other neurological conditions, such as neuropathy, can cause pain and numbness. Because of this, you may need to undergo certain imaging tests so your healthcare provider can confirm a cervical radiculopathy diagnosis.
Aside from a physical exam, healthcare providers use the following tests to diagnose cervical radiculopathy or to rule out other possible causes of your symptoms:
Advertisement
Fortunately, over 85% of cervical radiculopathy cases resolve (get better) without any specific treatments within eight to 12 weeks.
If your symptoms persist, cervical radiculopathy has several treatment options. As the condition affects everyone differently, your treatment plan will be unique to your situation.
Treatment options include:
Healthcare providers almost always start with nonsurgical therapies to treat cervical radiculopathy. About 90% of people with cervical radiculopathy have good to excellent outcomes with nonsurgical therapy.
If nonsurgical treatment isn’t working, your healthcare provider may recommend surgery.
For short-term management and to alleviate symptoms, your healthcare provider may recommend wearing a soft cervical collar (neck brace) to minimize neck movement and reduce nerve root irritation. A soft cervical collar is a padded ring (collar) that wraps around your neck and is held in place with Velcro®.
Healthcare providers typically don’t recommend wearing a cervical collar for more than one to two weeks because it can lead to muscle atrophy (muscle loss) in your neck.
In some cases, certain medications can help alleviate (relieve) symptoms of cervical radiculopathy, including:
Physical therapy and specific exercises focused on strength training and stretching your neck muscles can help treat cervical radiculopathy. Again, your physical therapy regimen will be unique to you and depend on several factors, such as which area of your neck is affected and your overall physical health and abilities.
In general, a physical therapy regimen for cervical radiculopathy will progress you through different stages as your pain improves, beginning with gentle range-of-motion exercises and adding strengthening and conditioning activities once the acute (severe and sudden) symptoms fade.
Your physical therapy may also include learning ways to have good posture and perform your job safely and comfortably.
A cervical epidural steroid injection (cervical ESI) is an injection of anti-inflammatory medicine — a steroid or corticosteroid — into the epidural space around your spinal nerves in your neck. The main goal of cervical epidural steroid injections for cervical radiculopathy is to help manage pain caused by irritation and inflammation of the spinal nerve roots in your neck.
Although cervical ESIs don’t relieve the pressure on the nerve caused by a narrow foramen or by a bulging or herniated disk, they may lessen the swelling and relieve the pain long enough to allow the affected nerve to recover.
Approximately 40% to 84% of people who receive a cervical epidural steroid injection experience at least partial pain relief. But some people don’t experience any pain relief.
Cervical ESIs have potentially serious side effects and complications. Be sure to ask your healthcare provider about the benefits and risks of getting a cervical ESI.
Your healthcare provider may recommend surgery if you’re experiencing severe and persistent pain despite trying nonsurgical therapy for at least six to 12 weeks or if you’re experiencing severe or worsening neurological issues due to cervical radiculopathy.
Several different surgical procedures can treat cervical radiculopathy. The procedure your healthcare provider recommends will depend on many factors, including what symptoms you have, your overall health and the location of the affected nerve root.
While nonsurgical treatment options usually successfully treat the symptoms of cervical radiculopathy, there isn’t a cure for the degenerative changes (age-related wear and tear) in your cervical spine that can cause cervical radiculopathy.
The prognosis (outlook) for cervical radiculopathy depends on several factors, including:
In most cases, people who go through nonsurgical treatment have a good prognosis and their symptoms disappear. In fact, many people who have cervical radiculopathy can treat it at home with time and rest.
However, symptoms of cervical radiculopathy recur (come back) in up to one-third of people after initial improvement.
If your symptoms come back, it’s important to talk to your healthcare provider.
While you can’t always prevent cervical radiculopathy, there are certain things you can do to reduce your risk, including:
Specific risk factors for developing cervical radiculopathy include:
If any of these risk factors apply to you, it’s important to talk to your healthcare provider about specific things you can do to try to prevent cervical radiculopathy.
If you have symptoms of cervical radiculopathy, such as pain that radiates down your neck, that don’t go away after a week or more of rest, contact your healthcare provider. If you have more serious symptoms, such as muscle weakness or weakened reflexes in your arm, contact your healthcare provider as soon as possible.
If you’re experiencing neck pain after an accident, such as a fall, contact your healthcare provider or go to the nearest hospital.
Having cervical radiculopathy (“pinched nerve”) can be uncomfortable and annoying. The good news is that most cases of this condition go away with at-home rest over time. If your symptoms persist for more than a week, talk to your healthcare provider. Several nonsurgical therapies can treat cervical radiculopathy. To prevent cervical radiculopathy, ask your healthcare provider about ways to keep your spine happy and healthy.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.