Broken heart syndrome (Takotsubo cardiomyopathy) is a sudden weakness in your heart muscle. This happens right after a physically or emotionally stressful event. The condition can last a few days or weeks. With medicine, most people recover completely. But some people have serious complications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
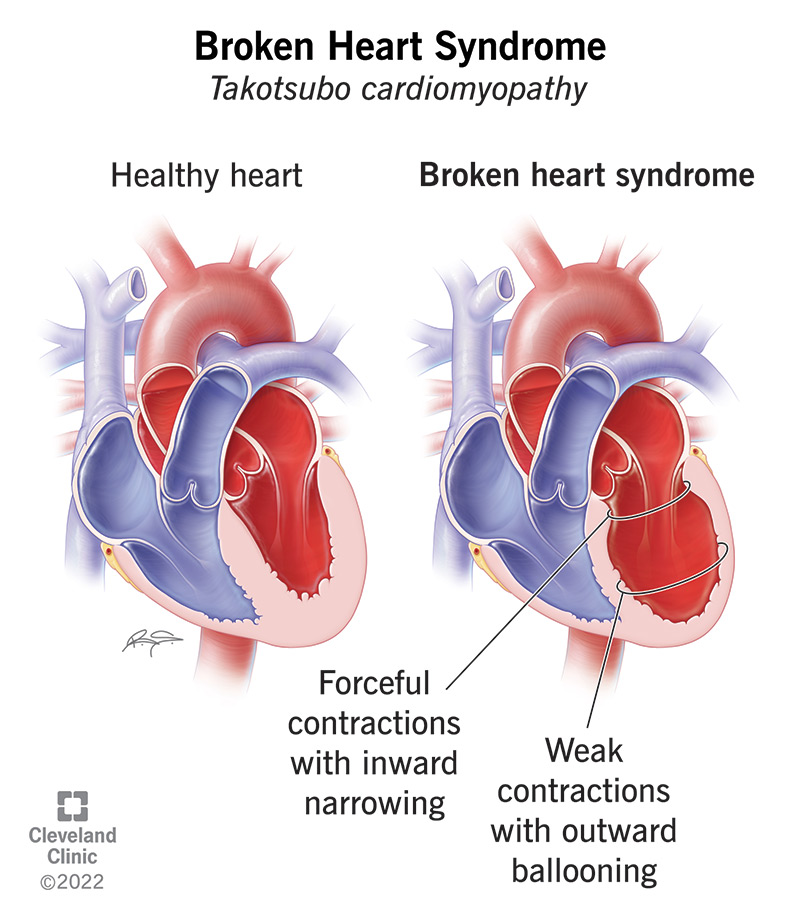
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17857-broken-heart-syndrome-illustration)
Broken heart syndrome is a short-term condition where some of your heart muscle weakens rapidly. This typically happens after a sudden physical or emotional stressor. Chest pain and shortness of breath can make it feel like a heart attack.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A weak heart muscle can disrupt your heart’s supply of blood and its ability to pump. If your heart isn’t pumping well, that harms your whole body. Every cell in your body relies on the steady supply of oxygen that your blood carries. And when part of your heart isn’t working well, the other parts of your heart may work harder.
There are many other names for, and types of, broken heart syndrome, including:
The four different types of broken heart syndrome are:
Advertisement
Most often, you may feel broken heart syndrome symptoms within minutes up to hours after the stressful event. These symptoms are like those of a typical heart attack.
Symptoms of broken heart syndrome include:
Because broken heart syndrome has symptoms like those of a heart attack, you may think you’re having one. Both conditions cause shortness of breath and chest pain. But with broken heart syndrome, you don’t have blocked coronary arteries and typically don’t have lasting heart damage. And you usually make a fast and full recovery.
Researchers think adrenaline and other chemicals your body makes during stress are the cause. When you react to physical or emotional stress, your body releases stress hormones in your blood. An event like a divorce, car accident or job loss can cause a release of these hormones. Experts think that these hormones stun or injure your heart muscle.
A small percentage of people with broken heart syndrome (Takotsubo cardiomyopathy) can’t name any stressors that may have triggered their episode.
Examples of sudden stressors include:
You’re more likely to get broken heart syndrome if:
One possible reason this affects women over 50 is that they may be less protected from the effects of sudden stress as they lose the hormone estrogen. This hormone protects your heart against any harmful effects of other hormones your body releases in response to stress.
There are no known ways to prevent Takotsubo cardiomyopathy. But learning how to manage stress and solve problems can help you limit physical and emotional stress.
Relaxation techniques can also be helpful. Some examples include:
Advertisement
Depending on the source of your stress, you may be able to join a support group to talk about your stress and share coping skills. A professional counselor can help, too.
In addition, healthy habits can help you manage physical or emotional stress. These habits include:
Broken heart syndrome complications are rare, but may include:
A healthcare provider will do a physical exam and review your medical history. Then, they may order several tests to look for weakening of the left ventricle of your heart — a main sign. Tests may include:
Advertisement
Imaging can show damaged heart areas, but a coronary angiogram can show blocked arteries in your heart. If you don’t have these, it helps rule out a heart attack. Unlike a heart attack, broken heart syndrome doesn’t involve these blockages.
Although there’s no cure for Takotsubo cardiomyopathy, most people make a full recovery after taking medicine.
Medications for treatment of broken heart syndrome include:
If your heart needs help pumping and you’re very sick from this syndrome, you may need an intra-aortic balloon pump or left ventricular assist device. This is rare.
Most people with Takotsubo cardiomyopathy start to feel better as they receive treatment. That can happen while you’re in the hospital or within hours or days of starting treatment.
Because broken heart syndrome shares symptoms with a heart attack, you should call 911 or emergency services if you have any heart attack symptoms. Those include:
Advertisement
If you have any of the symptoms of broken heart syndrome, seek emergency care. Tests are the only way to know if you have broken heart syndrome, a heart attack or another medical issue.
Contact your provider if you notice any new symptoms or changes in existing symptoms, especially if they affect your normal routine. Otherwise, your provider will schedule follow-up visits as needed. Your first visit will likely be within three months of diagnosis.
Questions to ask your provider may include:
Broken heart syndrome (Takotsubo cardiomyopathy) is a short-term condition for most people. You’ll likely recover without any long-term heart problems. People usually make a full recovery in a few days to a few weeks after a stress-induced event.
But many people have low energy levels for months after getting broken heart syndrome. This can lead to depression. If this happens to you, be sure to ask your provider for help.
If an ongoing health problem — like stroke, asthma or seizures — triggered your broken heart syndrome event, check with your healthcare provider for help managing these health issues.
You can get broken heart syndrome again or have other health problems weeks or years after the first event. In some cases, your provider may want to do a follow-up echocardiogram about four to six weeks after your event. They’ll want to make sure you don’t have any heart health problems and that the left ventricle of your heart is working normally again.
People who get broken heart syndrome from a medical issue (like illness or surgery) tend to have a worse outcome than those who get the condition from an emotional event. This is why men are more likely to have a worse prognosis. Although men are less likely to have broken heart syndrome, they’re more likely to get it from a critical illness.
You may need to keep taking prescribed medicines for three to six months. If you have broken heart syndrome, the best thing to do to take care of yourself is to take your medication and go to scheduled visits with your provider.
Researchers have linked taking ACE inhibitors or ARBs with better survival.
Most likely, no. Symptoms start after a sudden or extremely stressful event. If you have frequent chest pain or shortness of breath when facing day-to-day moderate stress, see a healthcare provider.
Ongoing symptoms usually aren’t a sign of broken heart syndrome. Your provider can help you figure out how to cope with stress, prescribe medication if anxiety is a problem, or order tests if they suspect an undiagnosed health problem.
Rarely, yes. If your condition is severe or unstable, you’ll need close monitoring and more advanced types of care. This may include mechanical support devices.
Depending on how weak your heart muscle is, your healthcare provider may also recommend cardiac rehab.
It’s unlikely that you’ll die from broken heart syndrome. Estimates of death from it range from 0 to 8 out of 100 people.
It’s common to hear people talk about a “broken heart” when they’re talking about their emotions. But broken heart syndrome (Takotsubo cardiomyopathy) is real and can happen after sudden emotional or physical stressors affect you.
The good news is that it’s a temporary condition that usually doesn’t cause any permanent heart damage. But because its symptoms are like those of a heart attack, never try to self-diagnose and convince yourself that you have broken heart syndrome. Always get checked at an emergency care center. Only tests can determine if your heart symptoms are a heart attack, broken heart syndrome or some other health issue.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
