Tularemia is a highly infectious disease you get from the bacterium F. tularensis. It commonly spreads from infected animals to people through insect bites, animal tissues or bodily fluids, and contaminated food or water. Treatment includes antibiotics.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
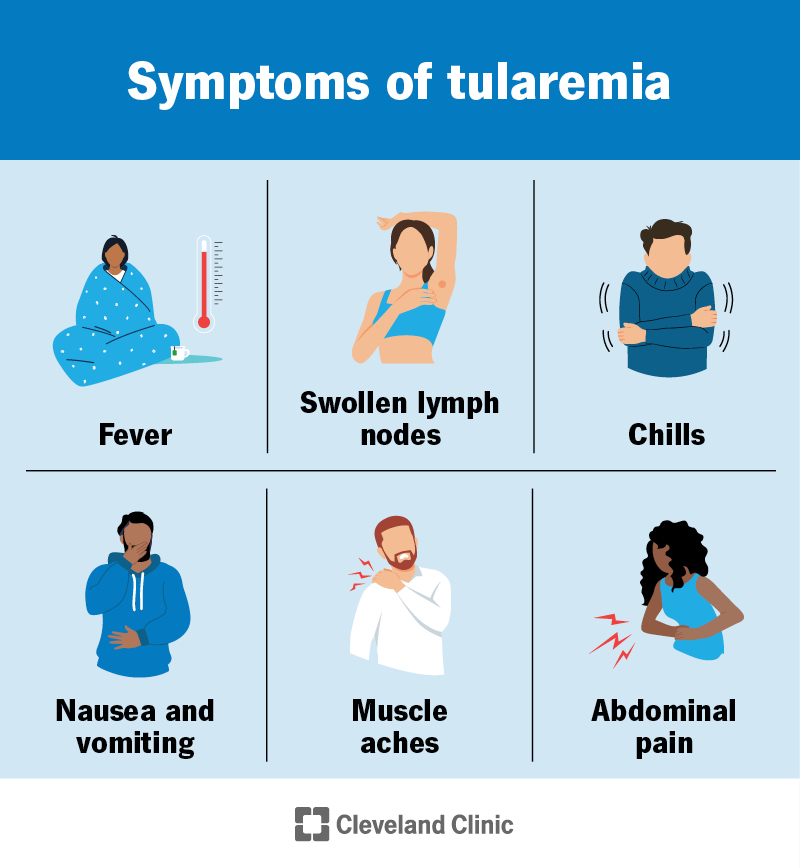
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/tularemia)
Tularemia is an infection you get from the bacterium Francisella tularensis (F. tularensis). It’s a zoonotic disease. That means it spreads between infected animals and people. It isn’t common — there were fewer than 200 cases in the U.S. in 2023. Most infections occur in the southcentral U.S., the Pacific Northwest and parts of Massachusetts. But experts have identified cases in other states, too. They believe climate change may be responsible for this spread.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Tularemia (pronounced “too-luh-REE-mee-uh”) can infect your:
Your symptoms may vary depending on where the bacteria infect you. But it generally causes a fever and painfully swollen lymph nodes. These symptoms may appear a few days or up to two weeks after exposure. The infection may range from mild to life-threatening.
Other names for tularemia include:
Tularemia has many forms. They vary according to how you got the F. tularensis infection and what your symptoms are. They include:
Advertisement
Symptoms depend on what form you have. Most forms cause general symptoms, such as:
Depending on the type you have, you may also have symptoms like:
The bacterium F. tularensis causes tularemia. There are two main types:
The most common ways in which tularemia bacteria spread from infected animals to humans are through:
Tularemia isn’t contagious — there’s no evidence that it can spread directly from person to person. But it’s highly infectious. That means even coming across a small amount of bacteria can make you sick.
Anyone can get tularemia. But you may be at a higher risk if you:
You’re also at a greater risk of illness if you have a weakened immune system. You may have a weakened immune system if you have:
Tularemia complications may include:
These complications are more likely to develop if you have pneumonic tularemia or typhoidal tularemia.
A healthcare provider will:
If they suspect tularemia, they may recommend tests to make an official diagnosis.
Advertisement
Your provider may recommend the following tests to look for F. tularensis or see if it grows from a sample:
Your healthcare provider will prescribe broad-spectrum antibiotics to kill Francisella tularensis bacteria. These may include:
You may need to take them as pills by mouth. Your provider may also inject them with a needle.
It’s important to treat tularemia as soon as possible. Your provider may give you antibiotics before your test results are back. This can help keep you from getting seriously ill. Take all of your antibiotics as recommended by your provider. If you don’t finish your full course, the infection may come back and be more challenging to treat.
Some people might recover from tularemia without antibiotics. But the risk of severe complications is high. Without treatment, tularemia may be fatal in 10% to 50% of cases.
You’ll need to take antibiotics for two to three weeks. But even after completing your full course of antibiotics, it may take some time before you feel completely better.
Sometimes, your symptoms may come back after you start to feel better. If this happens, you may need another course of antibiotics.
Advertisement
Schedule an appointment with a healthcare provider if you have tularemia symptoms, especially if you spend a lot of time around animals. Get to the nearest emergency room (ER) if you have symptoms of serious complications, including:
During your appointment, you may want to ask questions like:
With a quick diagnosis and prompt treatment, the outlook for tularemia is good.
The illness can be deadly. But it’s rare. The overall mortality rate is about 4%. But if you receive quick antibiotic treatment, the mortality rate is around 1%.
Advertisement
Depending on your symptoms, your provider may monitor you for the first few days of treatment. If you had symptoms for days or weeks before starting antibiotics, you’re at risk of developing serious complications.
The best ways to avoid getting sick are by protecting yourself and your pets:
It has similar symptoms to Lyme disease. But they affect your body in different ways.
Unlike tularemia, Lyme disease usually isn’t life-threatening.
It can be easy to dismiss swollen lymph nodes, a fever, a sore throat or stomach problems as symptoms of a minor infection. But if you spend a lot of time outside or around animals, these may be telltale signs of tularemia. It isn’t common. But it can have serious complications without treatment. Schedule an appointment with a healthcare provider. They can diagnose and treat tularemia. They can also suggest ways to help avoid getting it again.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
