Ticks are small bugs that can be hard to spot when they’re crawling on you. Tick bites can sometimes spread dangerous diseases, like Lyme disease and Rocky Mountain spotted fever. You can reduce your risk of tick bites by wearing bug spray, covering your skin and checking yourself and your pets for ticks.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
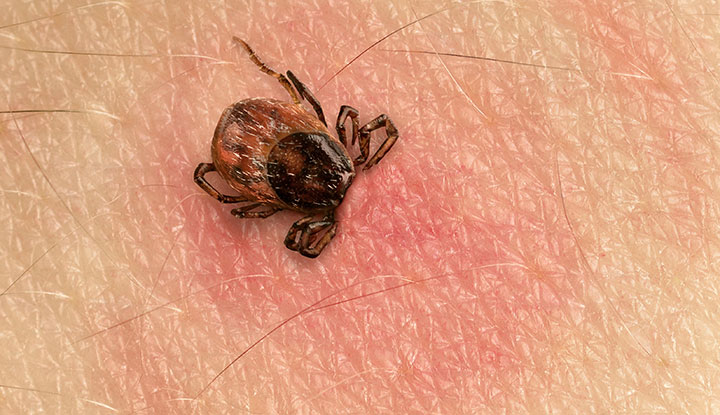
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/tick-bites)
Tick bites are areas on your skin where a tick has latched onto you with its mouthparts. This can sometimes leave a mark or rash. But often, the bite isn’t noticeable at all, unless you catch the tick while it’s still attached. Tick bites can be dangerous because they can spread potentially serious diseases.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Ticks are small, wingless bugs that usually live in the woods or tall grass. They bite people and animals to feed off of their blood. They’re tiny — sometimes as small as a poppy seed — and hard to see on your skin. And you probably won’t feel them bite you, either.
Unlike mosquitoes, ticks don’t just bite and run. They bury their heads into your skin. Then, they feed off your blood for hours or even days. As they fill with blood, they go from flat to rounded. The bites aren’t always harmful on their own. But while a tick is feeding on you, they can transmit bacteria, parasites and viruses into your blood.
Tick bites can cause:
Advertisement
Symptoms of conditions caused by tick bites could include:
The rash might look like a circle or a bullseye. Or it might be small, red or purplish spots that are actually spots of blood under your skin (petechiae).
Tick bites themselves often don’t cause noticeable symptoms like mosquito bites do. Sometimes, they might cause a bump, swelling or itching. You most often know you were bitten by a tick because you catch them attached to you.
Ticks can climb onto any part of your body. But they often move to warm, moist areas to latch on. Common places on your body to find ticks include:
Ticks bite because blood is their source of food. Young ticks (nymphs) hatch in spring and find an animal or person to feed off of. They mature into adults and take another meal in the fall. Tick bites are most common in spring, early summer and fall, but you can get bitten anytime.
Healthcare providers don’t usually diagnose tick bites directly. You might not have any markings on your skin or remember being bitten. But if you begin to have symptoms of a tick-borne illness, your provider may be able to use blood tests to check for diseases. Tests can sometimes take a few weeks. So, your provider may start treating you before the results come back.
If you found a tick biting you, be sure to take a photo or write down notes about what the tick looked like (any markings it had or if it was flat or rounded). This can help your provider treat you if you get sick. If you have symptoms of a tick-borne illness, make sure to tell your provider if you’ve been in an area that could have ticks, even if you don’t remember being bitten.
If you notice a tick biting you, you can remove it with these steps:
Don’t use kerosene, petroleum jelly (like Vaseline®) or a lit match to remove the tick.
Advertisement
Certain tick-borne illnesses are treated with antibiotics or antiparasitics. For others, there are no specific treatments.
See a healthcare provider if:
You can reduce your risk of tick bites by:
Advertisement
Some of the most common ticks in the U.S. include:
There are lots of things to like about spring and summer: The weather, vacations, flowers blooming. Tick bites don’t make anyone’s list. Fortunately, there are simple habits that can prevent tick bites or catch them early. If you find a tick on yourself, don’t panic. Remove it carefully and contact your provider if you have any questions about whether you need treatment.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
