Hypoxia is low levels of oxygen in your body tissues. It causes symptoms like confusion, restlessness, difficulty breathing, rapid heart rate and bluish skin. Many chronic heart and lung conditions can put you at risk for hypoxia. Hypoxia can be life-threatening. If you’re experiencing symptoms of hypoxia, call 911 or go to the nearest ER.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
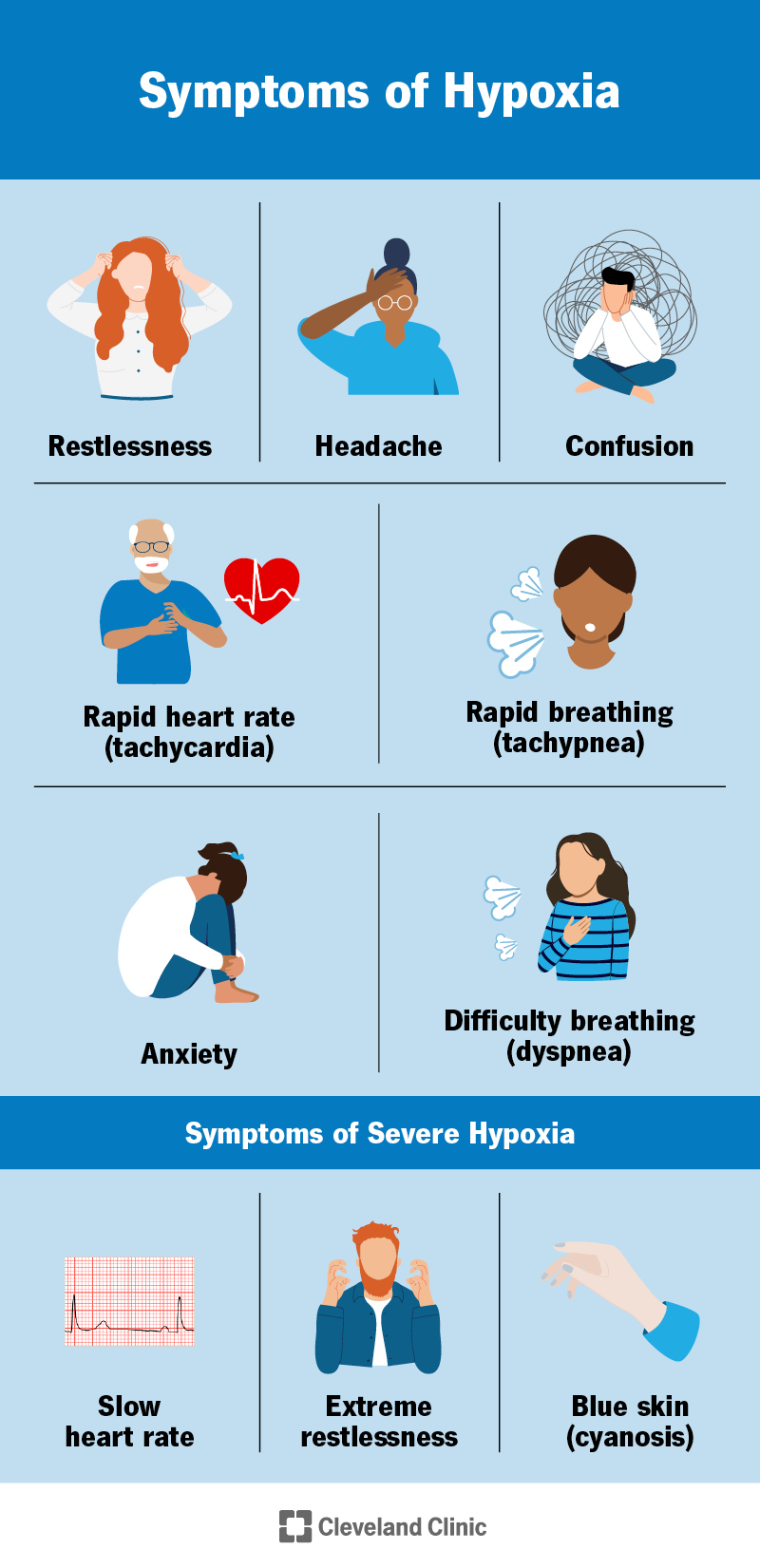
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23063-hypoxia.jpg)
Hypoxia is when the tissues or organs in your body don’t have enough oxygen. When you breathe, you take oxygen into your lungs, where it travels through your airways. It goes into small sacs called alveoli deep in your lung. In small blood vessels that surround alveoli, blood picks up oxygen and carries it. Oxygen remains in your blood until it arrives at other tissues in the rest of your body.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You can think of oxygen as billions of passengers flying into your lung “airport.” They get picked up at the gate by red blood cell “taxis” and get on blood vessel “highways” to reach your tissues. As blood vessels drop off oxygen, they pick up carbon dioxide. This is a waste product that goes back to your lungs and leaves your body when you breathe out.
If not enough oxygen gets through at any place on the journey, it can lead to hypoxia. Airflow and blood flow are both important to the process. This is why lung disease and heart disease both increase your risk of hypoxia. Someone who experiences hypoxia is called hypoxic. This condition can happen suddenly or be a long-term problem.
The four different types of hypoxia are hypoxemic, circulatory, anemic and histotoxic. They happen because you don’t have:
Low amounts of oxygen in your blood (hypoxemia) can lead to hypoxemic hypoxia. It’s the most common cause of hypoxia. Hypoxemia can come from lung and heart diseases, heart defects present at birth, and medications or health conditions that slow your breathing. Traveling to a high altitude, where levels of oxygen are lower, can also cause hypoxemia.
Advertisement
Your blood can have plenty of oxygen, but not enough of it reaches your tissues if your heart doesn’t pump enough blood or there’s a blockage in a blood vessel. This is called circulatory hypoxia (also called stagnant hypoxia or ischemic hypoxia). Congestive heart failure, blood vessel diseases and blood clots can increase your risk of this type.
Anemic hypoxia happens when you don’t have enough red blood cells to carry oxygen from your lungs to other tissues. You can become anemic if your body doesn’t make enough red blood cells or if it makes deformed or ineffective red blood cells.
Histotoxic hypoxia happens when your cells aren’t able to use oxygen properly. In this case, you can have plenty of oxygen coming into your lungs and entering your blood. But when it arrives at your tissues, something keeps your cells from being able to use it. This can happen with cyanide poisoning.
Hypoxia symptoms vary depending on the severity, underlying cause and which parts of your body it affects. Some conditions may cause long-term (chronic) hypoxia with less severe symptoms. When your oxygen is low, you might feel like you can’t breathe or think properly. Some general hypoxia symptoms include:
Severe hypoxia can cause a slow heart rate (bradycardia), extreme restlessness and bluish skin (cyanosis).
Hypoxia to certain tissues or organs can have symptoms specific to that area. This is most commonly associated with blockage of blood flow (ischemia), like the chest pain that occurs with heart attacks.
Any condition that reduces the amount of oxygen in your blood or restricts blood flow can cause hypoxia. It happens most often because of an underlying illness that affects blood flow or breathing. Conditions that can lead to hypoxia include:
People living with heart or lung diseases like COPD, emphysema or asthma are at an increased risk for hypoxia. Some infections — like pneumonia, influenza and COVID-19 — can also increase your risk of becoming hypoxic.
Advertisement
The best way to reduce your risk of hypoxia is to manage any conditions that can lower your oxygen levels. If you live with a heart or lung problem, talk to your healthcare provider about your concerns and specific ways to lower your risk. These could include medications, inhalers, devices that assist breathing or supplemental oxygen, to name a few.
Be aware that certain medications and situations — like traveling to a higher altitude — might increase your risk of hypoxia. Ask your provider about any special precautions you need to take while traveling or changing medication.
If you have an underlying condition that led to — or could lead to — hypoxia, managing that condition is the best way to lower your risk of it happening again. Here are some tips:
Advertisement
Your cells need oxygen to produce energy and help your organs and tissues to do their jobs. Some of your tissues can adjust to short-term dips in oxygen levels. But prolonged hypoxia can cause organ damage. Brain and heart damage are particularly dangerous. They can be fatal. Lack of oxygen to your brain is called cerebral hypoxia.
Your healthcare provider will perform a physical exam, including listening to your heart and lungs. They may check your skin, nails and lips to see whether they look bluish. Your provider may also order tests to check your oxygen levels and find the underlying cause of hypoxia. Tests may include:
Advertisement
The treatment for hypoxia depends on the underlying cause. The cause might be a one-time event or a long-term condition. Treatments might include:
If you have symptoms like severe shortness of breath, confusion, rapid heart rate or rapid breathing — or if you notice your nails, lips or skin appear bluish — seek medical help right away. You need prompt treatment for hypoxia to prevent permanent organ damage.
Hypoxia can be a life-threatening condition. Go to the emergency room if you have any symptoms of hypoxia or if others notice that you’re suddenly confused, restless or have a change in consciousness. Go to the ER if the typical symptoms of a chronic condition get worse suddenly, or you have new symptoms that you think might be hypoxia.
Some people test their oxygen levels with devices they purchased for home use. While these can sometimes be helpful, they’re not always accurate. You shouldn’t rely on them to rule out the need for emergency care. Not all breathing problems cause drops in oxygen levels.
If you or a loved one gets a hypoxia diagnosis, you may want to ask your healthcare provider:
Hypoxia usually requires prompt medical treatment. Your healthcare provider will talk to you about the underlying cause and how to manage it going forward.
The prognosis (outlook) for hypoxia depends on how severe it is, how healthy you are and what caused it. Some conditions that cause hypoxia are easier to treat than others. In some cases, treating the underlying issue takes care of the hypoxia. The need for extra oxygen goes away.
In other cases, you may need chronic supplemental oxygen to make sure there’s no ongoing hypoxia or tissue damage from low oxygen levels. Your provider will discuss your options with you.
When you can’t breathe and feel restless, it’s a scary feeling. Hypoxia is a life-threatening condition that’s treatable with prompt medical care. If you have a heart or lung condition that puts you at risk for hypoxia, talk to your healthcare provider about the signs and symptoms to look for and what to do if you think your oxygen is too low. Trust that you know your body best, and don’t hesitate to call your provider or go to the nearest ER if you have any worrisome symptoms.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Whether you need stitches, a broken bone set or think your appendix might be causing your abdominal pain, Cleveland Clinic’s emergency medicine team is here to help.
