Gastritis is inflammation in the soft mucous lining of your stomach. This lining is a protective barrier in your stomach. When it’s inflamed, it means it’s under attack. It might be from an infection, a substance you ingested or digestive chemicals.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
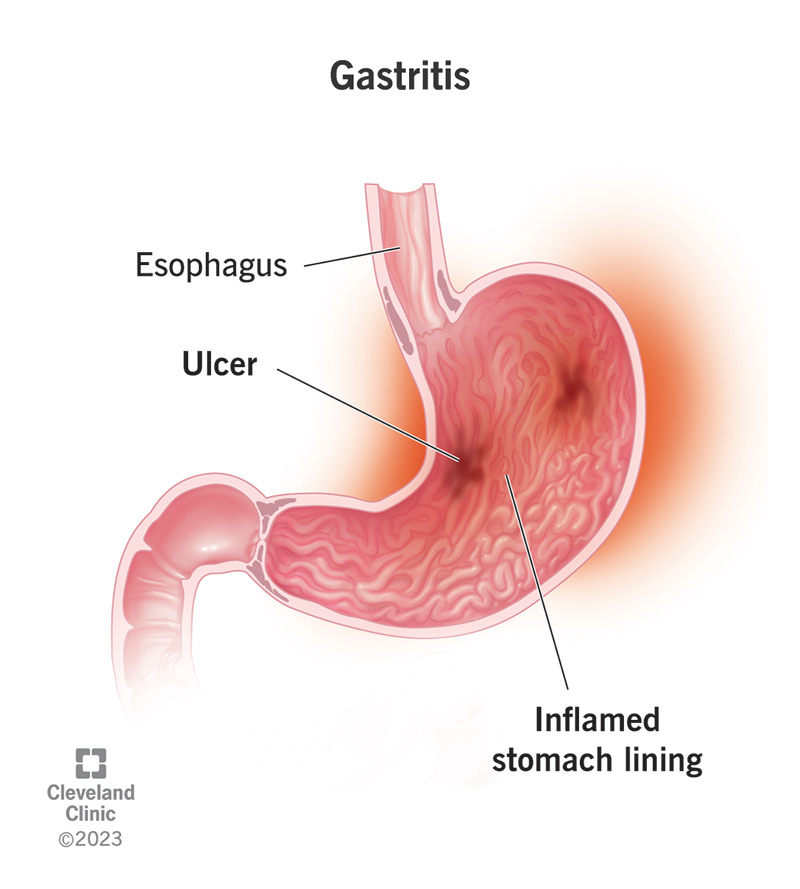
Gastritis is inflammation in the lining of your stomach. This lining (a soft tissue called mucosa) protects your stomach from the acids, enzymes and microorganisms that pass through it every day. Gastritis happens when your immune system detects a threat to this barrier. Your immune system triggers inflammation in the tissues to help fight infections and promote healing.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You can have acute gastritis or chronic gastritis.
Gastritis can also be erosive or nonerosive.
Gastritis may go by a more specific name, based on the cause. Some examples are:
It’s very common. In the U.S., acute gastritis affects about 8 out of every 1,000 people. It’s usually related to common short-term infections, alcohol and medication use. Chronic gastritis affects about 2 out of every 10,000 people in the U.S. But worldwide, as much as half of the population has chronic gastritis associated with a widespread, chronic bacterial infection called H. pylori.
Advertisement
Gastritis may not cause any noticeable symptoms. If it does, it may mean that it’s more severe or it’s been going on for a long time. Symptoms may happen when your stomach lining is worn down enough that it can’t defend itself against its own acids and enzymes anymore. The acids may cause symptoms of indigestion, or they may cause stomach ulcers, which can hurt and bleed. Symptoms may include:
If you have a bleeding ulcer, you may find:
Gastritis pain is in your stomach, which is located in your upper middle abdomen (“epigastric” region). General pain from inflammation will feel like it’s somewhere in this area (upper abdominal pain), but you might not be able to pinpoint the exact spot. If you have an ulcer, you might be able to pinpoint the pain more precisely. It might have a burning or gnawing quality. It might feel better when you eat.
Gastritis is a response from your immune system to something already going on inside your stomach. Your immune system sends inflammatory cells to your stomach lining to fight infections and help repair the tissues. Inflammation causes the symptoms of gastritis, if you have any. But the original offender is something else — something that’s threatening your stomach lining. There are many possibilities.
Infections are among the most common causes of gastritis, especially acute gastritis. Bacterial infections and viral infections associated with the stomach flu can cause a short-term reaction that usually clears by itself. H. pylori infection is a common, chronic bacterial infection that can cause chronic gastritis. Less commonly, parasite infections and fungal infections can also cause acute or chronic gastritis.
Alcohol and certain drugs can cause either acute or chronic gastritis, depending on how much and how often you use them. They can cause chemical erosion of your stomach lining (erosive gastritis). Overuse of NSAIDs (nonsteroidal anti-inflammatory drugs), such as aspirin and ibuprofen, is one of the most common causes of acute gastritis. Some recreational drugs, like cocaine, may also cause it.
Autoimmune diseases cause chronic inflammation. In autoimmune disease, your immune system mistakenly attacks your body’s own cells with inflammation. Chronic autoimmune gastritis can happen spontaneously. Or, more rarely, you may have gastritis as a side effect of another autoimmune disease.
A major surgery, trauma or critical illness can cause acute gastritis. Severe physiological stress causes your body to withdraw blood supply from your digestive system to redirect it toward your more vital organs. This lowers your stomach lining’s defenses, making it more vulnerable to the chemicals inside.
Advertisement
Other causes of gastritis include:
Most of the time, gastritis is temporary and not serious. But if gastritis goes on for a while, it can eventually begin to damage your stomach lining. This can lead to complications.
Erosive gastritis can proceed to peptic ulcer disease. Ulcers can cause gastrointestinal bleeding, leading to anemia. Frequent ulcers can also cause scarring. Scar tissue in your stomach can become a problem if it narrows or blocks the openings at the bottom (pylorus). This is called gastric outlet obstruction (GOO).
An ulcer that doesn’t heal may eventually wear a hole all the way through your stomach wall (gastrointestinal perforation). This can allow bacteria from your stomach to escape into your abdominal cavity (peritonitis). Peritonitis can lead to further complications, including septicemia and sepsis.
Nonerosive gastritis causes complications much more slowly. But after many years, it can cause your stomach mucosa to diminish (atrophy) and to lose some of its functionality. You may have trouble digesting and absorbing certain nutrients, such as iron, folic acid and vitamin B12 (pernicious anemia).
Advertisement
Rarely, long-term gastritis can cause the cells in your stomach lining to restructure themselves to look like a different sort of tissue altogether. This is called gastric intestinal metaplasia. Healthcare providers consider this cellular change precancerous, meaning it can raise your risk of developing stomach cancer.
A healthcare provider will start by asking you about your symptoms and health history. They might suspect gastritis based on your answers, but they won’t know for sure if you have it without testing for it. They might begin with an imaging test, such as an upper GI series, a series of X-rays of your upper GI tract. This test can detect ulcers or erosion in your stomach lining, though not always gastritis itself.
The real proof of gastritis is microscopic, so a healthcare provider will need a tissue sample to confirm it. They can take a sample (biopsy) during an upper endoscopy exam. This exam goes inside your upper GI tract with a tiny camera on the end of a long catheter (endoscope). An endoscopist can take a biopsy through the endoscope. They’ll usually recognize gastritis visually even before the biopsy confirms it.
You might need additional tests to isolate the cause of gastritis or to check for complications. Your provider may order:
Advertisement
Acute gastritis goes away after the acute cause of it does. If you have an infection, in most cases your immune system will clear it out shortly, and then the inflammation will go down. If you briefly overdosed on alcohol or pills, your stomach lining will soon repair itself. If blood flow to your stomach was temporarily reduced but is now restored, your stomach lining will begin the healing process.
Chronic gastritis doesn’t go away by itself, but treatment can help it go away. Chronic gastritis is linked to another chronic condition that you have. Specific treatments can cure some of these conditions. Other conditions aren’t curable, but long-term treatments can reduce the inflammation they cause. Chronic gastritis may have done deeper damage to your tissues, so they may take longer to heal.
You can treat your symptoms with over-the-counter (OTC) medications that soothe irritation and neutralize stomach acid, like proton pump inhibitors (PPIs) or Pepto Bismol®. These can bring temporary relief while your stomach is healing. You have to make sure that the cause of your gastritis has been eliminated, though. So, make sure to see a healthcare provider even if you’re self-medicating.
Curing chronic gastritis requires professional care. The treatment will depend on the cause.
It might mean:
Most cases of gastritis improve quickly with treatment. Medication relieves symptoms for most people. For some, recovery may also involve permanent lifestyle changes. You may need to change the way you manage other conditions and quit or reduce substance use to prevent gastritis from coming back. If you’ve discovered an underlying chronic condition, you may have a new long-term treatment plan for it.
Gastritis itself isn’t contagious, but the infections that cause it are. H. pylori, in particular, has infected most of the world’s population, and it’s caused chronic gastritis in about half. It spreads by the fecal-to-oral route. You can help prevent spreading infections by practicing good hygiene, such as handwashing after going to the bathroom and before handling food. This could prevent many cases of gastritis.
An occasional episode of acute gastritis is nothing to worry about, and you can usually treat it at home. But if it doesn’t go away, or if you have symptoms of gastritis often, you should see a healthcare provider. Chronic symptoms point to a chronic condition that needs attention. Most gastrointestinal symptoms overlap with many different conditions, so it’s important to get an accurate diagnosis.
If you have issues with your digestive system, you need a team of experts you can trust. Our gastroenterology specialists at Cleveland Clinic can help.

Last reviewed on 07/14/2023.
Learn more about the Health Library and our editorial process.