Bile reflux occurs when the valves that keep bile from backwashing into your stomach and esophagus aren’t working properly. Bile can erode the delicate linings of your stomach and esophagus, causing inflammation and tissue damage.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
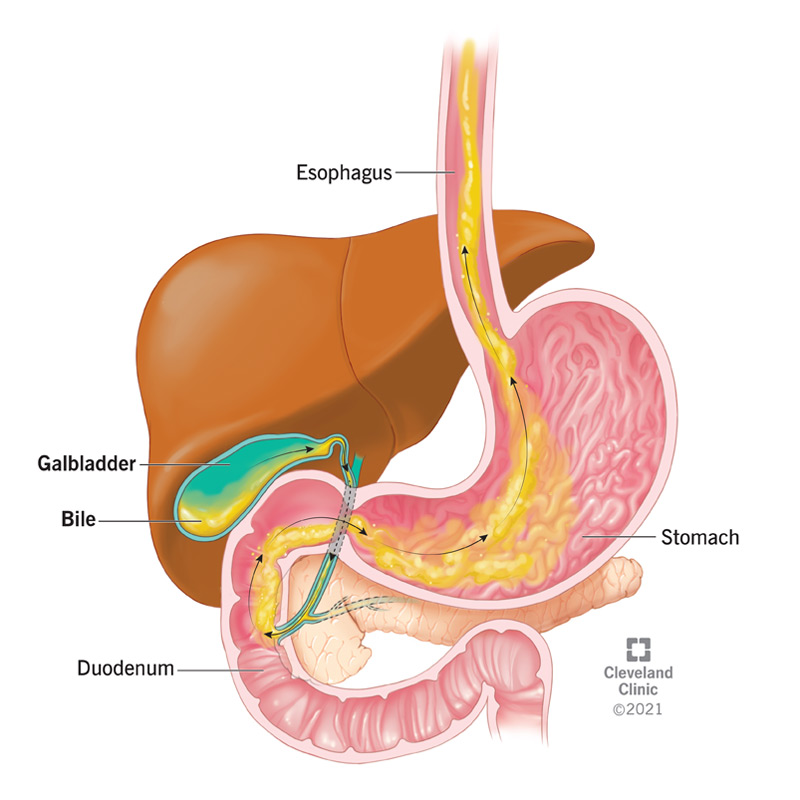
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22056-bile-reflux-web.ashx)
Bile reflux occurs when the bile that’s released into your small intestine to help digest food washes back into your stomach, and sometimes into your esophagus.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Normally, everything involved in the digestive process should only flow one way — down. As food progresses along the digestive tract, valves at the end of each organ open just enough to let food and digestive juices through into the next, without letting anything flow back the other way. But if these valves (sphincters) aren’t functioning right, reflux can happen, and digestive juices like bile can flow back into organs where they don’t belong.
Bile is produced in your liver, stored in your gallbladder and released into your small intestine when there are fats there to digest. The pyloric valve lets food out of your stomach and into your small intestine, where it mixes with bile. If the pyloric valve is too relaxed, or maybe obstructed, it doesn’t close properly, and bile can flow back into your stomach.
If the valve that lets food into your stomach from your esophagus — the lower esophageal sphincter — doesn't close properly, stomach juices can wash back into your esophagus. This is commonly known as acid reflux. But if you have bile reflux, those juices may contain bile, too. Sometimes, bile is the bigger problem irritating your esophagus.
Bile is composed of ingredients designed to digest fat. While it isn’t an acidic formula, it’s harsh on the sensitive linings of your stomach and esophagus. Chronic bile reflux can erode these protective linings, causing painful inflammation and, eventually, tissue damage (esophagitis). You’ll feel it as a burning kind of stomach ache, heartburn or sore throat, or as regurgitation of stomach contents into your esophagus. You may also have frequent nausea, indigestion or even bile vomit.
Advertisement
Chronic inflammation of your stomach lining (gastritis) can lead to stomach ulcers and is associated with a higher risk of stomach cancer. Inflammation of your esophagus (esophagitis) can cause ulcers, scarring and cellular changes to your lining (Barrett’s Esophagus), which is occasionally a precursor to esophageal cancer. These risks are also associated with chronic gastroesophageal acid reflux (GERD), but studies show that bile reflux multiplies the risk.
Bile reflux is not thought to be common in otherwise healthy individuals. However, acid reflux is very common, and some cases of acid reflux may also be bile reflux. Symptoms of bile reflux and acid reflux are practically identical, and doctors can’t tell if you’re regurgitating bile without actually sampling and analyzing the fluid you regurgitate. This is considered unnecessary when diagnosing acid reflux. But if you’ve been treated for acid reflux and still have symptoms, you might be a candidate for further testing.
Bile reflux is most commonly recognized as a complication of surgery, particularly stomach surgery that bypasses, damages or replaces the pyloric valve. Gallbladder removal surgery (cholecystectomy) may also be associated with bile reflux. When your gallbladder is removed, your liver is redirected to release bile directly into your small intestine. But when bile isn’t stored and concentrated in the gallbladder first, it can overflow into your stomach.
If you have bile reflux in your stomach, you may notice:
If you have bile reflux in your esophagus, you may notice:
Symptoms of acid reflux and bile reflux in your esophagus are virtually the same. If your symptoms include vomit, check the color. Bile has a tell-tale yellow tint. If you also have symptoms of bile reflux in your stomach, such as abdominal pain and indigestion, that might be an important clue.
In general, acid reflux is considered more common and more likely than bile reflux. But if medications to treat acid reflux don’t relieve your symptoms, let your healthcare provider know. They can test the reflux fluid in your esophagus to detect the presence of bile.
Bile reflux is most commonly caused by a problem with the pyloric valve that’s supposed to keep bile from escaping into your stomach. This might be a result of:
Advertisement
Bile reflux will usually involve abdominal symptoms and sometimes esophagus symptoms. While reflux into your esophagus is easy to diagnose based on your symptoms alone, reflux into your stomach will need to be confirmed by imaging tests. Your healthcare provider will probably order an upper endoscopy exam to look inside of your esophagus, stomach and upper small intestine. The endoscope can take tissue samples while it takes images, to test for inflammation, tissue damage and the presence of bile. For reflux into your esophagus, they may take additional tests to distinguish acid reflux from bile reflux.
Advertisement
Healthcare providers prescribe a variety of medications to treat bile reflux and its symptoms, but these have not been well studied. You’ll have to see if they work for you. When they don’t work, and your symptoms remain severe, your healthcare provider may recommend surgery.
Medications to treat bile reflux include:
Surgical interventions to treat bile reflux include:
Unlike acid reflux, bile reflux can’t be treated with over-the-counter antacids or diet changes. Bile reflux is difficult to treat even with prescription medications. Sometimes, surgery is necessary. However, some small lifestyle adjustments, including raising the head of your bed, losing some excess weight and eating dinner earlier, may help ease your symptoms a little.
Advertisement
Prolonged exposure to bile can damage the linings of your stomach and esophagus. This can result in chronic inflammation, pain, and side effects such as ulcers.
Treating bile reflux can be challenging, but healthcare providers have a few things up their sleeve that you can try. If medications don’t work, and your symptoms are severe, surgery may be a solution.
Reflux of any kind is serious. If you have frequent symptoms of reflux, your stomach or esophagus may be suffering systematic erosion. You might be able to manage acid reflux with over-the-counter antacids, diet and lifestyle changes. But if your symptoms persist, or if they include abdominal symptoms, you might have bile reflux. This will require further medical testing and treatment.
Bile (or non-acid) reflux is not common, but it’s a known complication of certain surgeries. If you experience bile reflux following gastric or gallbladder surgery, you may be able to treat it with medications, but you may need a follow-up surgery to fix it. Other causes of bile reflux are just beginning to be recognized and understood. Non-surgery bile reflux, or “primary biliary reflux,” may take some testing to identify. But its symptoms — including inflammation and pain — will always be taken seriously. Talk to your healthcare provider if you have symptoms or concerns.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have issues with your digestive system, you need a team of experts you can trust. Our gastroenterology specialists at Cleveland Clinic can help.
