Sciatica is pain caused by irritation or compression of your sciatic nerve. You can feel it in your lower back, butt and leg. It’s a common condition that may cause pain, numbness or tingling. Most people recover with stretching, medication or physical therapy. Severe cases may need surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
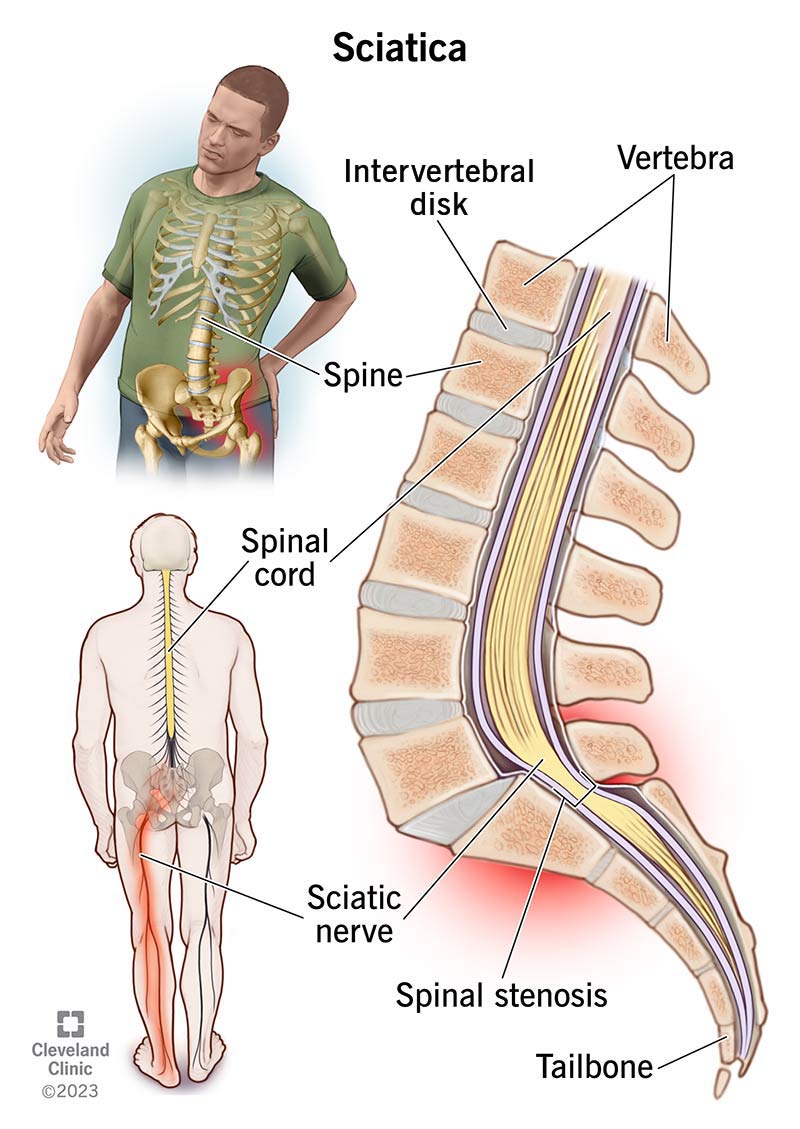
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/12792-sciatica)
Sciatica is nerve pain from an injury or irritation to your sciatic nerve. In addition to pain, it can involve tingling or numbness in your back or butt that may radiate down your leg. You may also feel symptoms in your feet or toes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Sciatica is very common. Many adults will experience it at some point in their lives. It’s one of the most common causes of leg pain seen in medical care.
There are two main types. No matter which type you have, the symptoms often feel the same. These include:
Healthcare providers often use the term “sciatica” for both types. The difference usually matters most when your provider recommends treatment.
The sciatic nerve is a long nerve in your lower body. It’s the largest nerve you have. There’s one on each side.
The nerve plays a major role in how your lower body feels and moves. It connects your lower back to your hips, butt and legs.
The sciatic nerve starts near the base of your spine in your lower back. It passes through your pelvis and butt. It then runs down the back of each thigh and into your lower leg.
The nerve begins narrow in your lower back and gets slightly wider as it travels down your leg. At its widest point, it’s about the size of a penny.
Advertisement
It helps your legs and feet move. It also helps you feel sensations like touch, pain and temperature in your legs. Even though it passes through your butt, it doesn’t control those muscles.
Your sciatic nerve provides two types of functions:
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_pk8qgs91/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Chiropractor, Andrew Bang, DC answers some of the most common questions about sciatica.
You may feel sciatica pain in your lower back, butt or legs. Symptoms range from mild to severe and may include:
Serious symptoms to look out for include:
Sciatica happens when something pinches, presses on or irritates your sciatic nerve or its nerve root. It can also happen when conditions affect the group of nerves in your lower back that form the sciatic nerve.
Conditions that can cause sciatic nerve pain include:
In some cases, providers can’t find a clear cause.
Certain factors may increase your risk. These include:
With treatment, most people recover fully. In some cases, symptoms can last longer and lead to ongoing pain.
If a nerve is badly damaged, muscle weakness may occur. One example is foot drop. This makes it hard to lift the front of your foot when walking.
Advertisement
In rare cases, nerve damage may be permanent. This could cause lasting numbness or loss of feeling in your affected leg.
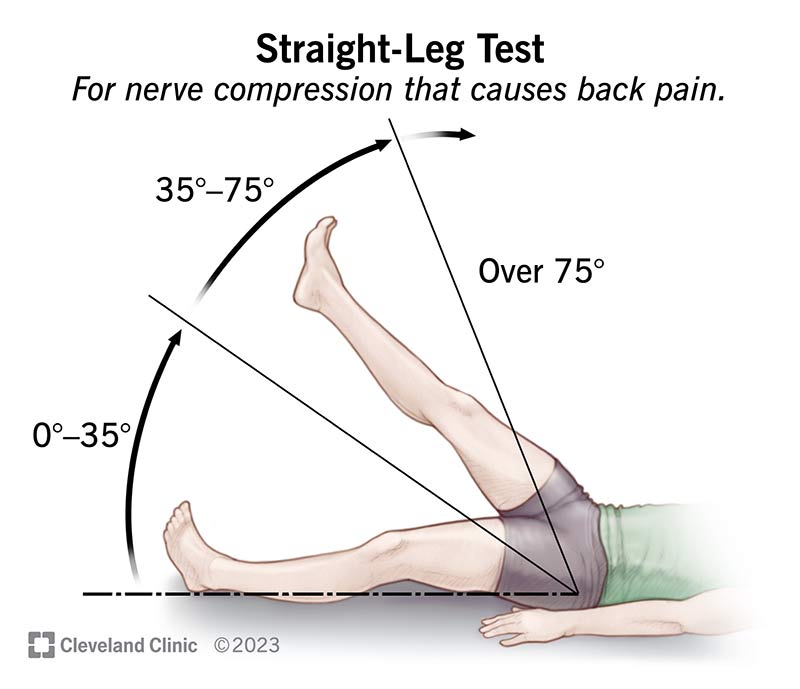
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/12792-sciatica-straight-leg-test)
A healthcare provider uses several steps to diagnose sciatica. First, they’ll ask about your symptoms and review your medical history. Then, they’ll perform a physical exam.
The physical exam may include:
Your provider may order tests to confirm the diagnosis or rule out other conditions. Tests usually aren’t done right away unless you have severe or worsening symptoms. Tests may include:
Treatment for sciatica focuses on easing pain and helping you move more easily.
If symptoms are mild, you can start with self-care. Moderate to severe pain, numbness, tingling or muscle weakness needs medical care.
Advertisement
Many people start treatment with steps they can do at home. Your provider might recommend the following for mild symptom management:
If symptoms don’t improve after a few weeks, talk with a healthcare provider.
If self-care doesn’t help or symptoms are more severe, your provider may recommend:
During physical therapy, your therapist may teach you exercises to do in their office and at home. They’ll show you how to perform them safely. Here are some examples:
Advertisement
Surgery is usually a last option. Providers may suggest it if pain is severe, nerve damage is a concern or if other treatments don’t help.
Common procedures include:
Recovery time varies based on your symptoms and their cause. It can also depend on the type of treatment you use.
Many cases improve within four to six weeks without medical treatment. More severe cases may take longer and can last several weeks or months.
If symptoms last longer than a few weeks or get worse, it’s important to talk with a healthcare provider.
Mild cases often improve over time with self-care. Most people feel better without needing surgery.
Talk with a healthcare provider if pain doesn’t improve after a few weeks or if recovery feels slower than expected.
Sciatica often doesn’t last longer than six weeks. When it does, your healthcare provider may recommend more involved treatments, like therapy or surgery.
The outlook is usually very good. Most people recover without long-term problems. Ongoing issues are more likely only if symptoms are severe.
Not all causes of sciatica pain can be prevented. These tips may help lower your risk:
Sciatica usually affects one leg at a time. In rare cases, it can affect both legs.
Sciatica is common during pregnancy, but it’s not usually caused by weight changes alone.
Pregnancy hormones can loosen ligaments in your spine. This can make your spine more flexible and increase pressure on your nerves. The growing fetus can also press on your sciatic nerve.
There are ways to ease pain during pregnancy. Options may include:
Pain often improves after birth.
Hip problems often cause pain in your groin. Pain may also occur when you put weight on your leg or move your hip.
Sciatic pain usually starts in your lower back. It may travel into your hip or down your leg. Numbness, tingling and weakness also point more toward sciatica.
Short periods of rest may help during the first day or two. Too much rest may make pain worse and slow recovery.
Light movement can help you stay flexible and strong. A healthcare provider can help you find the right balance between rest and activity.
Sciatica can catch you off guard. One moment, you feel fine. The next, you’re dealing with sharp, shooting pain that travels down your leg. It’s more than just back pain; it’s a nerve issue that can impact how you move, rest and go about your day.
Fortunately, most people start to feel better with time and simple steps like stretching or applying heat or ice. If symptoms stick around or get worse, your provider can guide you through options like physical therapy or medications.
You know your body best. If something doesn’t feel right, don’t wait to get care. These are signs to take seriously.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Low back pain can be a constant interruption in your daily life. Cleveland Clinic’s experts can help craft a treatment plan to help you find relief.
