A defibrillator can save your life if you’re in cardiac arrest. This device provides an electrical charge that stops your heart’s abnormal rhythm so your heart can get back to a normal rhythm. Even with defibrillation, cardiac arrest is fatal for many people. It’s not unusual for survivors to require multiple types of therapy to recover.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A defibrillator is a device that provides an electric shock to your heart to allow it to get out of a potentially fatal abnormal heart rhythm, or arrhythmia, — ventricular tachycardia (with no pulse) or ventricular fibrillation — and back to a normal rhythm. Both of these arrhythmias happen in your heart’s ventricles or lower chambers.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
People who have the above arrhythmias can get help in a hospital or a place that has an automated external defibrillator available. However, if you have a high risk of a life-threatening heart rhythm, you may need your own defibrillator that’s with you all the time.
A shock from a personal defibrillator can be painless or feel as if someone kicked you in the chest.
People who are at high risk for a life-threatening heart rhythm may have these defibrillator types:
While cardiopulmonary resuscitation (CPR) provides temporary assistance, a defibrillator can help you survive sudden cardiac arrest. You can even use a defibrillator if someone already has a pacemaker or implantable cardioverter defibrillator (ICD).
Advertisement
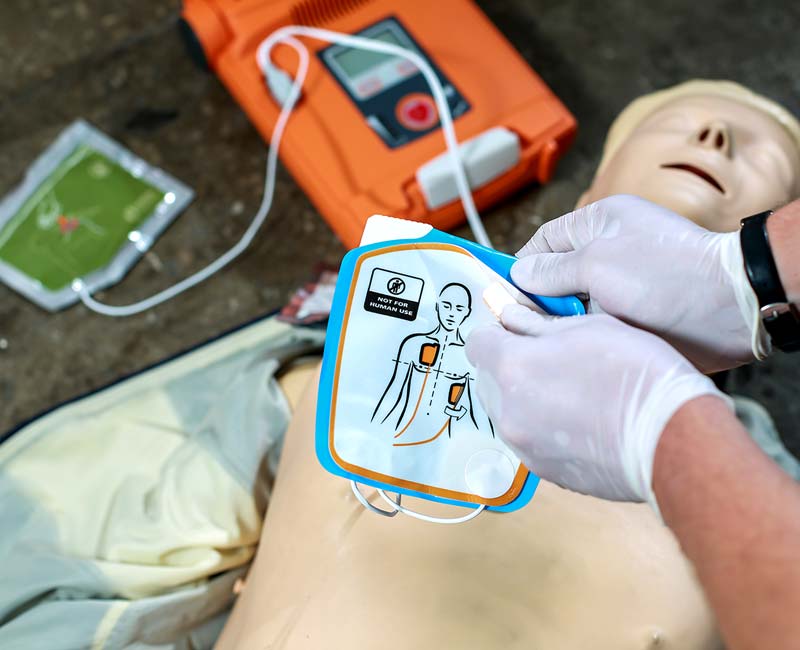
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23020-defibrillator)
You should continue giving CPR while waiting for a defibrillator to be ready to use.
Before you deliver the shock, make sure no one is touching the person who’s about to receive the shock (or their bed).
If you’re using an automated external defibrillator (AED), it can review your heart’s rhythm to decide if it needs a shock. An AED charges itself and provides verbal instructions on how to use it.
A first responder or healthcare provider will do the following:
A defibrillator makes your heart muscle stop moving briefly so your heart can create an electrical impulse that starts a normal rhythm. In essence, defibrillation restarts your heart.
Your first responder or provider will give CPR again for two minutes. Then they’ll check for a pulse and look at whether your heart rhythm is back to normal. If you need it, they’ll give you more CPR and another electrical shock. If defibrillation didn’t work the first time, they’ll also give you medications (epinephrine or amiodarone) to try and correct the abnormal rhythm.
If your blood is flowing, but you’re still not responsive, your provider may need to bring your body temperature down to 89.6 to 96.8 degrees Fahrenheit (32 to 36 degrees Celsius) to help protect and promote recovery of your brain function. Once your condition is stable, your provider may do cardiac catheterization.
A defibrillator can save your life if it’s used for the correct arrhythmia and it’s done within 10 minutes after the abnormal rhythm starts.
A defibrillator needs to be used for ventricular tachycardia (without a pulse) or for ventricular fibrillation. If you use it for any other kind of arrhythmia, it could give someone ventricular fibrillation and cardiac arrest.
After cardiac arrest and defibrillation, recovery is a long-term process that takes months or years. Up to 40% of cardiac arrest survivors have some impairment that doesn’t allow them to go back to work or do regular activities after leaving the hospital. Fatigue may limit your ability to do what you want. It may take time to recover from a rib fracture that happened during CPR and to manage other problems, such as trouble walking or seizures. It’s possible that you’ll need occupational, physical and/or speech therapy.
Advertisement
If you witness someone collapsing, call 911.
After surviving ventricular fibrillation, you have a high risk of experiencing it again. Your provider will treat the cause of your ventricular fibrillation, which may include giving you an ICD. Regular checkups are important to make sure your ICD continues to work properly. After five years or so, you’ll need to get a new ICD battery.
If you have an ICD or someone used a defibrillator to help you, keep taking medicines your healthcare provider prescribed for you. Be sure to see your provider regularly to ensure that your ICD is working correctly. If your provider used a defibrillator for you in an emergency situation, it may take months or years for your body to recover. Physical therapy and other types of therapy can help you rehabilitate, but it’ll take patience and time.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart rhythm is out of sync, the experts at Cleveland Clinic can find out why. We offer personalized care for all types of arrhythmias.
