Caudal regression syndrome is a condition that affects how the fetus develops in the uterus. This condition targets your child’s bones, renal system and gastrointestinal tract. Children diagnosed with this condition may have trouble peeing and pooping. Treatment is symptomatic and usually involves surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
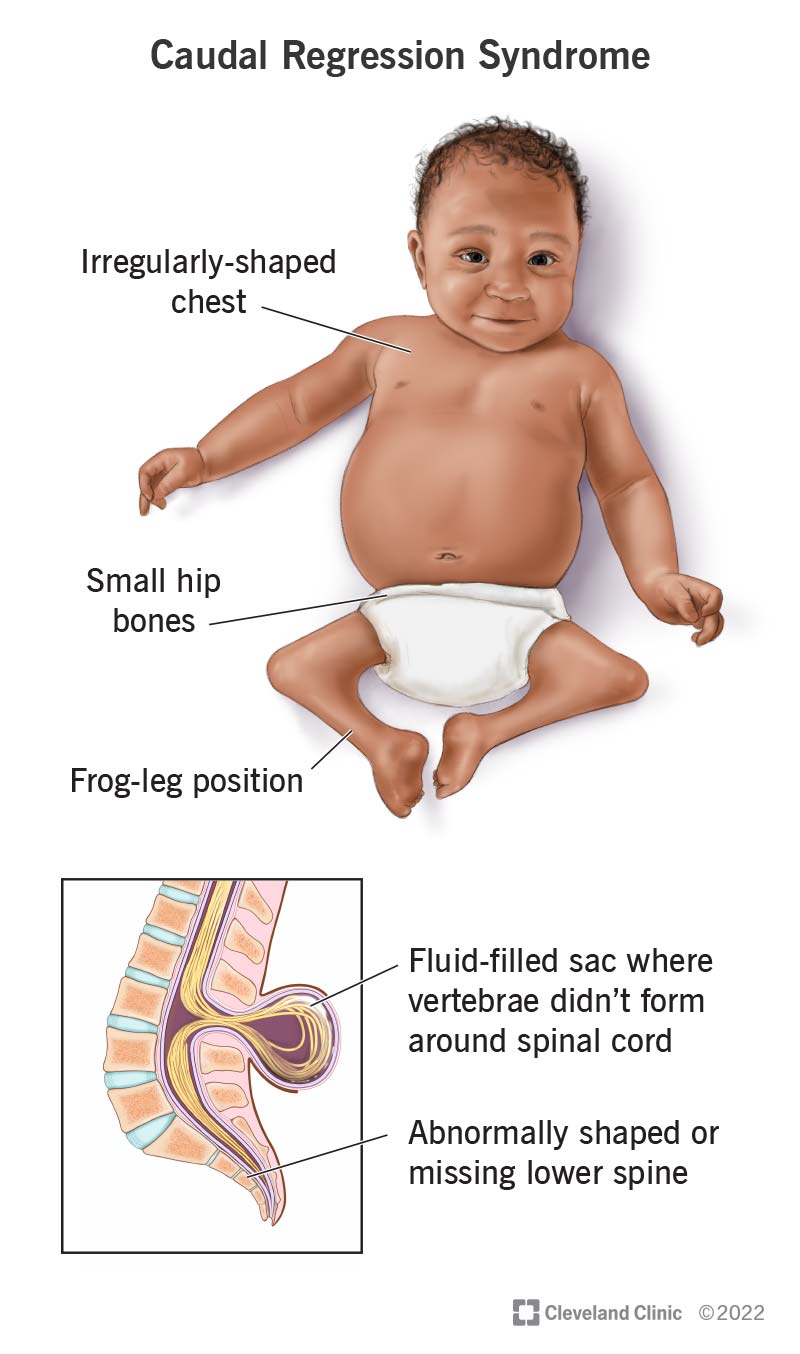
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23425-caudal-regression-syndrome)
Caudal regression syndrome (CRS) is a condition that affects how the fetus develops in the uterus. This condition can affect the:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Infants diagnosed with this condition might experience challenges walking, pooping and peeing.
Caudal regression syndrome can affect anyone. Some causes are genetic, and the genetic mutation usually happens sporadically. This means CRS typically occurs even if you don’t have a history of the condition in your biological family.
Caudal regression syndrome affects an estimated 1 to 2 out of every 100,000 newborns worldwide. CRS is more common among infants born to parents who have diabetes, where it affects an estimated 1 in 350 newborns.
Symptoms of caudal regression syndrome affect the lower half of your child’s body and range from mild to severe. Your child could experience a few symptoms or several symptoms depending on the severity of their diagnosis.
Symptoms of caudal regression syndrome can affect how your child’s bones develop, including:
Advertisement
Infants with underdeveloped bones in their legs caused by caudal regression syndrome may have an irregular stance that can affect how they walk. This could include:
Symptoms of caudal regression syndrome can affect the development and function of your child’s renal system, digestive and urinary tract. Symptoms could include:
Caudal regression syndrome can also affect the development and function of your child’s reproductive organs. Symptoms that affect their reproductive organs include:
Symptoms of caudal regression syndrome can also affect other internal organs in your child’s body, including:
Multiple genetic and environmental factors can cause caudal regression syndrome in a newborn including:
Advertisement
Some cases of caudal regression syndrome happen sporadically, or randomly, where a cause isn’t clear. Research is ongoing to learn more about the possible causes of this condition and how it affects newborns.
Your healthcare provider can sometimes diagnose caudal regression syndrome before your child is born during a prenatal ultrasound. During this test, they’ll look for symptoms of the condition that affect the development of the lower half of your child’s body.
Once your child is born, your provider might offer additional tests to learn more about the extent of their diagnosis. Tests could include an imaging test, like an X-ray or an MRI, to examine the effects of the condition on your child’s bones and organs.
Treatment for caudal regression syndrome is symptomatic and unique to each child diagnosed with the condition and could include:
Advertisement
Your child may need more than one surgery to manage their symptoms as they grow. Based on your child’s symptoms, they might need to start treatment with medications or surgery soon after they’re born or during early infancy.
Caudal regression syndrome can affect your child’s ability to pee and poop. If your child receives a CRS diagnosis, they may need help going to the bathroom. Your child’s healthcare provider will offer possible treatment options to help your child by:
Your child’s bowels might not be able to function as expected throughout their life. This can be a challenging situation to navigate. Your child’s healthcare team will create a treatment plan to help you and your child manage, adapt and adjust to their condition to improve your child’s quality of life.
Your child will receive care from a variety of specialists who are experts in specific areas of your child’s body. Their healthcare team could include:
Advertisement
Caudal regression syndrome is a lifelong condition without a cure. Symptoms affect several different parts of your child’s body and require a team of specialists to treat and manage the condition throughout your child’s life. Your child may need surgery early during infancy to improve any growth abnormalities that occurred during their development. Your child may spend a few weeks in the hospital after they’re born to make sure they’re healthy. Your healthcare team will work with you and your child’s caretakers to help you learn more about your child’s diagnosis, what symptoms you should monitor at home and how you can help your baby grow and thrive.
You can’t prevent caudal regression syndrome because some of the causes are the result of random genetic changes that you can’t predict or prevent. You can take steps to reduce your risk of having a child with caudal regression syndrome by working with your healthcare provider to manage your blood glucose levels if you have diabetes during pregnancy.
Visit your child’s healthcare provider if:
Visit the emergency room if your child has trouble breathing or if their heart beats irregularly, or for any other concerning symptoms.
Learning that your child has a caudal regression syndrome diagnosis can be challenging and overwhelming. Your child may have difficulty with mobility and using the toilet. Their symptoms could require several surgeries to repair parts of their body that didn’t develop in the uterus. Adapting these changes can be difficult. Some families find comfort by joining support groups or speaking with a mental health professional. Your child’s healthcare team will work closely with you to make sure you understand what’s happening with your child so you can help them grow.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a neurological condition, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
