Dermatillomania, also known as skin picking disorder or excoriation disorder, is a mental health condition where you compulsively pick at your skin. This can cause injuries, infections and scarring, leading to stress, anxiety and a reduced sense of well-being. This condition is often treatable with a combination of medication and therapy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
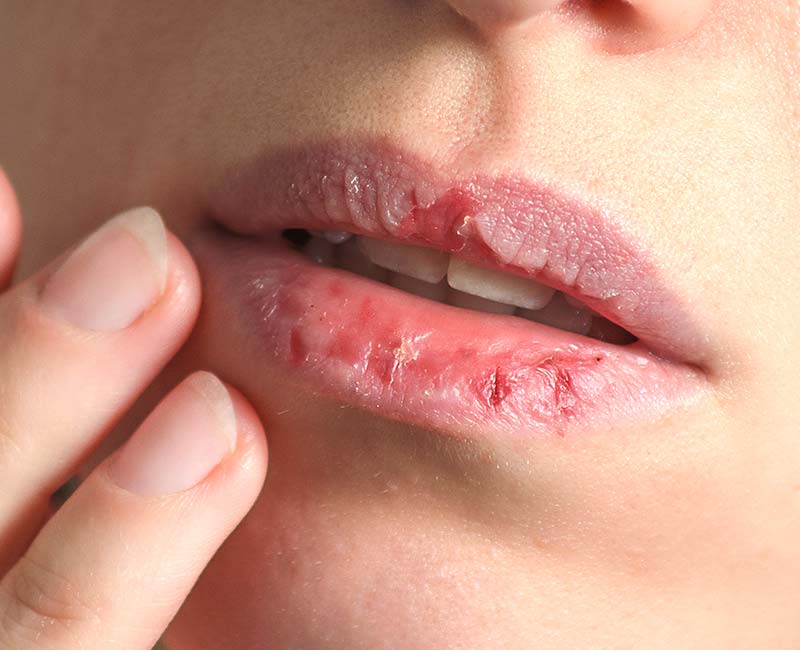
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22706-dermatillomania)
Dermatillomania is a mental health condition where a person compulsively picks or scratches their skin, causing injuries or scarring. Also known as excoriation disorder or skin-picking disorder, this condition falls under the category of obsessive-compulsive disorders (OCDs). When it leads to significant scarring and injuries, this condition can severely affect a person’s mental health, well-being and quality of life.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This condition (pronounced derm-ah-till-oh-main-ee-ah) gets its name from three Greek words:
Obsessive-compulsive disorder (OCD) is a specific condition that also lends its name to a category of mental health conditions. While dermatillomania falls under the overall category of obsessive-compulsive disorders, it still has some key differences from the specific condition of OCD.
In years past, experts believed this condition was much more common in women. However, recent research shows that only about 55% of people with this condition are women. Women are also more likely to seek treatment for this problem.
The condition usually starts during puberty but can happen at any age. The condition is also more likely to happen to people who have “triggering” conditions like acne or eczema.
Advertisement
Dermatillomania is an uncommon condition, with an estimated 2% of people having it at any time and up to 5.4% of people having this condition at some point in their life.
Dermatillomania causes a person to pick at their skin compulsively. For some people, picking is an automatic movement, and they might not even realize they’re doing it. Others are aware that they’re doing it but can’t stop themselves.
For some people, picking focuses on areas of skin that are rough or already have some kind of blemish or irregularity. Examples include picking at pimples, patches of dry skin or scabbed-over cuts and scratches (those wounds can come from picking or from other causes).
Picking can create new wounds or reopen old ones, leading to bleeding and scarring. When this condition is severe, it can lead to skin damage that’s extensive enough that it may need surgery, such as skin grafting, to repair the damage. Infected wounds may also need antibiotic treatment.
In rare cases, infections from these wounds can spread throughout your body, leading to an overwhelming immune system overreaction. That overreaction, a condition called sepsis, is a life-threatening medical emergency.
Often, people with this condition feel embarrassed or ashamed of the visible injuries, trying to hide them with clothing, makeup or other means. Because of that, this condition can be a source of anxiety, depression or social isolation. This condition can also affect people’s work or social lives.
The main symptom of dermatillomania is compulsively — meaning, the impulse or urge is impossible or incredibly difficult to resist — picking at your skin. Experts also describe the act of skin-picking using the following words:
Picking usually involves fingernails and fingertips but can also include biting with your teeth (especially when the skin surface affected is on your lips. It can also involve sharp items like tweezers or pins.
This activity usually happens in one of two ways, “automatic” or “focused.”
Picking tends to focus on certain areas of your body. Those areas are the ones that you can most easily reach with your hands, including:
Advertisement
There aren’t any confirmed causes of dermatillomania, but experts suspect a few different factors might play a role, including:
People with dermatillomania are more likely to have other mental health or medical conditions. Some of these include:
Dermatillomania isn’t contagious and can’t spread from person to person.
Diagnosing dermatillomania involves a combination of a physical exam, where your healthcare provider looks for signs of this condition on your body. They’ll also ask you questions about your medical history, your life circumstances and any behaviors that might relate to this condition. Diagnostic and lab tests can help rule out other causes for skin picking but are rarely needed to confirm this diagnosis.
Advertisement
Diagnosing this condition requires meeting all five of the following criteria:
Medical tests that are used with this condition are almost always to rule out any other medical conditions. Your healthcare provider can best explain what tests they’d like to run for your specific case and why.
Treating dermatillomania usually involves a combination of medication and therapy. Research shows that combining the two tends to help more than just one type of treatment alone.
The most common medications that healthcare providers prescribe to help treat this condition include:
Advertisement
Psychotherapy can help treat this condition in various ways, depending on the therapy method used.
People with severe damage to their skin or their tissue underneath may need additional medical treatment and care. Your healthcare provider is the best person to explain the treatments they recommend, which might include surgery and skin grafting, antibiotics and more.
The possible side effects and complications depend on the circumstances, the severity of your condition and other factors. Your healthcare provider is the best source of information about what you should expect or watch for because they can tailor the information to your specific case.
Dermatillomania isn’t something you should self-diagnose. A trained, experienced mental health provider should be the one to determine if you have dermatillomania or if it’s actually another condition. It also isn’t something you should treat on your own, partly because medication, therapy methods and other types of care need a prescription or other input from a healthcare provider.
Your healthcare provider can tell you more about what you can expect as you undergo treatment and what you can do to help yourself through that process. This is because the recovery time and how long it will take you to feel better depend on many different factors, and your healthcare provider can take all those factors into account when they tell you what to expect.
Dermatillomania usually isn’t a dangerous condition unless it's very severe. The main risk from this condition is from open wounds, which might develop infections because of repeated picking or damage. Though this condition isn’t usually dangerous directly, it still commonly has severe negative effects on your quality of life and overall sense of well-being.
People with dermatillomania often feel ashamed or embarrassed, which is why so many people with this condition avoid treatment. Avoiding or delaying treatment increases the risk of having permanent issues like scarring and further mental health problems.
Dermatillomania is a life-long condition because of the risk of relapse. However, people with this condition can go into remission — meaning, they no longer feel the urge to pick their skin or can avoid doing it for long periods, if not indefinitely.
The outlook for the condition depends on how severe it is and other factors. Most people with this condition don’t suffer physically dangerous effects. But without treatment, most people with this condition will struggle with mental health effects like anxiety, shame or embarrassment.
Dermatillomania is a mental health condition, but experts still don’t fully understand what causes it. That means it happens unpredictably and it isn’t preventable. There isn’t a known way to reduce your risk of developing it either.
If you have dermatillomania, it’s important to see a healthcare provider (or multiple providers, depending on your specific needs) with training and experience in treating this disorder. They can give you the best guidance on caring for yourself and what you can do to improve your outcome.
In general, you should do:
People with dermatillomania usually don’t need emergency medical care unless they have severe injuries because of this condition. You should seek care in cases with severe bleeding or signs of infection. The signs of infection, including dangerous conditions like sepsis, include:
Dermatillomania is a mental health condition that can severely affect your life due to feelings of shame, embarrassment or guilt. These feelings are common, and seeing a healthcare provider can help you overcome them and receive treatment for this condition. Healthcare providers have special training and experience in treating conditions and their effects, and helping you feel comfortable with getting the treatment you need. With treatment, many people can overcome or manage this condition. That means you can focus on what you want to do in life rather than worrying about what people might notice or think about you.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Your mental well-being is just as important as your physical well-being. Cleveland Clinic’s mental health experts can help you live life to the fullest.
