Trichotillomania is a mental health condition where you compulsively pull out your own hair. It often has severe negative effects on your mental health and well-being when it happens in your adolescent, teen and adult years. However, this condition is treatable.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
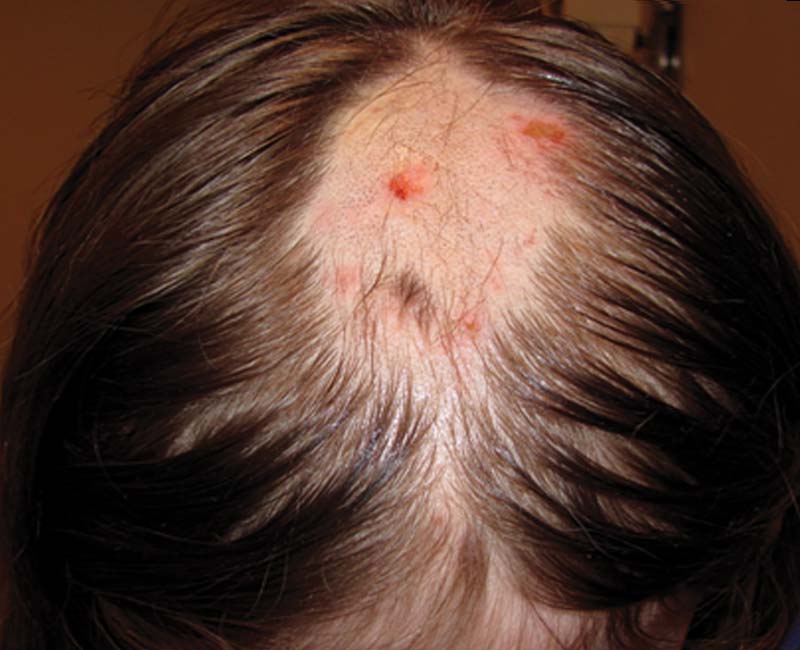
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/9880-trichotillomania)
Trichotillomania (often abbreviated as TTM) is a mental health disorder where a person compulsively pulls out or breaks their own hair. This condition falls under the classification of obsessive-compulsive disorder (OCD). When it’s severe, it often has extremely negative effects on a person’s happiness, well-being and overall quality of life.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Trichotillomania (pronounced trick-oh-till-oh-main-ee-uh) comes from three Greek words:
TTM falls under the overall category of obsessive-compulsive disorder, but it has some key differences from OCD itself.
TTM is especially common in children and adolescents. In young children and infants, it’s usually a short-lived concern and goes away on its own. The more serious form most commonly starts between ages 10 and 13.
In children, it happens equally between men and women. In adults, women outnumber men with this condition by as much as 9 to 1.
TTM is relatively uncommon. Research studies estimate it affects 0.5% to 3.4% of adults at some point in their lifetime.
People with TTM compulsively pull out their hair, usually one strand at a time. Many people will pull hair from the same spot. The most common places people pull hair from are their scalp, eyelashes and eyebrows, and pubic hair.
Advertisement
The effects of trichotillomania also depend on the age at which it happens. Children commonly pull their hair in this way, but that behavior is often a self-soothing act. Children often grow out of this behavior and don’t have any long-term negative effects. Adolescents, teenagers and adults with this condition tend to have much more severe problems.
People with TTM commonly feel anxiety, embarrassment or shame about this condition. This can affect their work and social lives. Many people with this condition don’t seek treatment because they feel embarrassed or ashamed.
About 20% of people with this condition eat their hair after pulling it, a condition known as trichophagia (from Greek words “tricho” for hair and “phagia” for eating). This can lead to hairball-like blockages in their digestive tract. Those blockages are sometimes dangerous and often cause damage that needs surgery to repair.
People with TTM commonly hold back from telling their healthcare provider about this even after revealing details about TTM. This is often because they’re waiting until they feel they can trust their provider more before sharing that amount of detail.
People who pull out their hair often cause damage to their skin and tissue just underneath the skin’s surface, especially if they use any kind of personal care tool like tweezers. Skin and tissue damage sometimes need repair or skin grafting to fix. Damage to skin caused by hair pulling can also cause permanent hair loss in affected areas.
According to the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders Fifth Edition (DSM-5), the diagnosis of TTM requires a person to meet five criteria:
Some people with TTM pull their hair deliberately, such as when they feel a hair is out of place or looks different from others around it. Other people pull their hair automatically without thinking about it.
While experts suspect several possible factors could lead to TTM, there aren’t any confirmed causes of this condition. Some of the suspected factors include:
Advertisement
There are several mental health conditions that a person is much more likely to have along with TTM. These can happen either as separate conditions or because of TTM (especially anxiety and depression). These include:
No, TTM isn’t contagious, and it can’t spread to others. While some experts suspect it might be something you can inherit from your parents, more research is necessary to confirm that.
Diagnosing TTM involves a combination of a physical exam, where your healthcare provider looks for visible signs of the condition. They'll also ask questions about your health history, current circumstances and anything else that might have a connection to a medical problem.
TTM is a relatively straightforward condition to diagnose, but people with this condition often hide it out of shame or embarrassment. That can make it harder for your healthcare provider to diagnose this condition based solely on asking questions. That’s why a specific type of skin test may also help.
In some cases, a “punch biopsy” (where your healthcare provider takes a skin sample for lab analysis) is necessary to confirm a diagnosis of TTM. This test can also rule out other skin conditions that might be the true cause of hair loss or hair pulling.
Advertisement
In cases where your healthcare provider suspects a blockage from swallowed hair, you might also undergo other diagnostic tests. These include imaging tests like a computerized tomography (CT) scan, blood testing for anemia and more.
Treating TTM often involves therapy, medication or a combination of both. Ongoing research shows some medications for other mental health conditions might help TTM, but more research is necessary before any specific medication becomes a part of the standard care.
Medication alone often isn’t enough to treat TTM. Healthcare providers may use combinations of medications, therapy techniques or both.
Medications that may treat, either on their own or in combinations, TTM include:
Advertisement
Therapy methods that may help treat TTM include:
People with TTM with hair loss or scarring may need to see other healthcare providers and specialists. In some cases, a dermatologist can help treat related skin problems or damage. Plastic and reconstructive surgeons may also help with skin grafting for affected areas of your body. Other healthcare providers can also offer solutions related to hair regrowth; though, regrowth isn’t always an option.
The possible side effects that can happen with medications depend on the medications themselves, as well as your medical history and circumstances. Your healthcare provider can tell you more about possible side effects, including potential trouble signs and how you should react if you see those signs. They’re the best source of information about this because they can tailor the information they give you to your specific health needs, situation and circumstances.
TTM isn’t a condition you should diagnose on your own. That’s because a trained and experienced mental healthcare provider is better prepared to determine if you have TTM or another health condition. It’s also not something you should treat on your own, partly because both medication and therapy methods often need a prescription or other input from a healthcare provider.
The time it takes for you to feel better from medication, therapy or a combination of the two can be very different from person to person. Your healthcare provider can tell you more about what you can expect as you undergo treatment and what you can do to help yourself through the process.
TTM isn’t usually a danger to your physical health (except in rare cases, especially when a person develops a digestive tract blockage from hair they’ve swallowed). However, it can be very disruptive and damaging to your mental health and quality of life.
Because people with TTM often feel ashamed or embarrassed of this condition, most avoid treatment. Those who avoid or delay treatment are much more likely to have issues like permanent hair loss, scarring and more severe mental health problems.
The available research, while limited, shows that people with TTM have this condition for an average of about 22 years. In some cases, the condition is a lifelong problem. People also often describe that the condition has phases, becoming more or less severe for periods of time. Overall, early diagnosis and treatment are the best chance for limiting how long this condition lasts and how severely it impacts your life.
The overall outlook for this condition depends partly on the age of the person who has it. Infants and children with TTM often have the best outlook, with the condition commonly going away on its own.
However, the older a person gets — especially from adolescence onward — the greater the odds that treating the condition becomes difficult. TTM on its own is rarely a life-threatening problem. But its impacts on a person’s life, especially their mental health, are often severe. Because of this, early diagnosis and treatment are very important.
TTM is a mental health condition, which means it isn’t preventable. There’s also no known way of reducing your risk of developing it.
If you have TTM, it’s important to see a healthcare provider (or multiple providers) with specialized training and experience in treating this condition. They can best guide you on what you can do to minimize the impact of this condition on your life.
In general, healthcare providers recommend the following:
People with TTM who swallow their hair have a higher risk of blockages in their digestive tract. These blockages often cause severe or even life-threatening complications. The following symptoms are likely with a blockage and mean you should call your healthcare provider or go to the hospital:
Trichotillomania, or hair pulling, can have a severe effect on your mental health. People with this condition often feel ashamed, embarrassed or guilty because of it. If you have TTM or know someone who does, it’s important to remember this is a medical condition and that hair pulling is very difficult to control or stop on your own. But with treatment, it’s possible to limit how often you pull your hair or stop pulling it. That can help you live a life where your hair and appearance don’t make you feel anxious or ashamed, so you can focus on things that matter most to you.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Your mental well-being is just as important as your physical well-being. Cleveland Clinic’s mental health experts can help you live life to the fullest.
