Synovial sarcoma is a rare, slow-growing soft tissue cancer. It doesn’t always cause pain, and symptoms can resemble those of other, more common health conditions like arthritis or bursitis. The outlook is more favorable if a surgeon can remove the entire tumor before it spreads.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
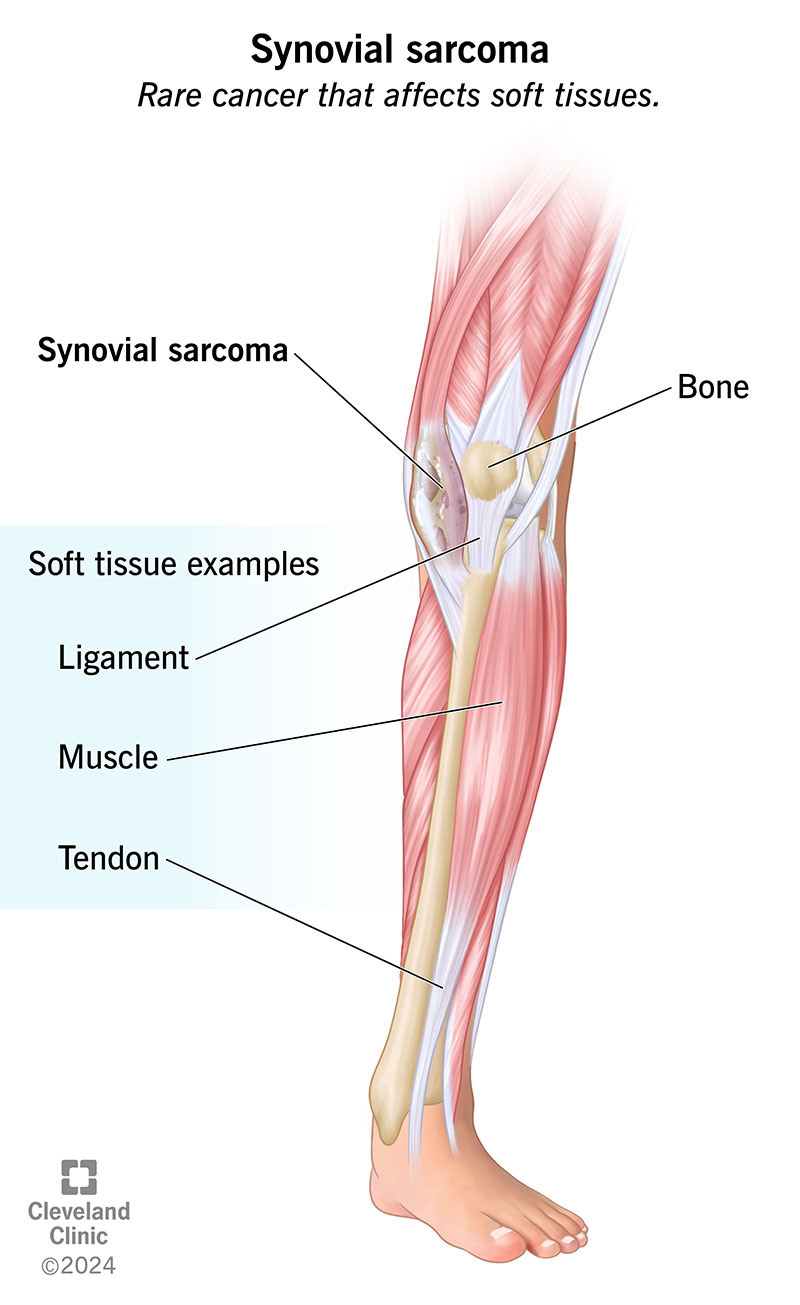
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/synovial-sarcoma)
Synovial sarcoma (synovial cell sarcoma) is a rare type of cancer that affects soft tissues, like your muscles or ligaments. It’s called synovial sarcoma because these cancer cells resemble the cells in your synovial joints (like your elbows, hips and shoulders).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Synovial sarcoma grows very slowly and may not cause pain. Many times, you won’t have symptoms until the tumor grows large enough to create a lump you can see and/or feel. Some people develop pain or numbness, especially if the tumor presses on nerves as it grows.
Early diagnosis and treatment are helping people with synovial sarcoma live longer, with hope for a cure. But a cancer diagnosis can turn your world upside down. What does this mean? What will my life look like now? If these are questions running through your mind, you’re not alone. Your healthcare team will walk with you every step of the way.
This type of cancer can affect several different areas of your body, including your abdomen, arms, feet, legs and lungs.
Synovial sarcoma can also form in joints like your:
Very rarely, synovial sarcoma can form in your chest, head or neck.
Like other soft tissue sarcomas, synovial sarcoma is an uncommon form of cancer. It affects about 1,000 people each year in the U.S. Anyone can get synovial sarcoma, but it’s most common in males under 30.
Synovial sarcoma cancer develops gradually over time. Tumors can grow undetected for up to two years. During this time, you may not have any symptoms at all. Once symptoms occur, they may include:
Advertisement
Synovial sarcoma symptoms can look and feel like symptoms of other, less serious conditions like arthritis or bursitis. Because of this, synovial sarcoma may go undetected for a time. If you notice any kind of lump under your skin, schedule an appointment with a healthcare provider and see them as soon as possible.
Researchers aren’t sure what causes synovial sarcoma. But they know it has something to do with mutations (changes) in your chromosomes. Synovial sarcoma cells always have one mutated gene in common. Sometimes, your chromosomes break into pieces. The pieces rejoin, but not in the same order or sequence.
Imagine your chromosome as a jigsaw puzzle and your genes as puzzle pieces. Now imagine someone jams a puzzle piece into a spot where it doesn’t belong. In synovial sarcoma, a gene called SYT jams up against genes that aren’t the right fit. When this happens, your cells don’t work as they should, and your body develops a mutant gene that causes synovial cell sarcoma.
A healthcare provider will do a physical examination and ask you about your symptoms and health history. If they think you might have synovial cell sarcoma, they’ll refer you to an oncologist for further testing.
An oncologist will examine you and use imaging tests to see the size and location of the tumor.
Imaging tests might include:
Your provider will likely have the tumor biopsied. During this procedure, they’ll take a small tissue sample from the lump under your skin. Once they have the sample, they’ll send it to a pathologist, who will look at the cells under a microscope.
Surgery is the standard treatment for synovial sarcoma. The goal is to remove the tumor and some of the tissue around it to make sure it all comes out. In some cases, this means removing an entire muscle or muscle group. It depends on how far the cancer has spread. Your provider can tell you what to expect in your situation.
Providers may do surgery as a stand-alone treatment or in combination with other therapies like:
Healthcare providers base treatment on several factors like tumor size and location, how long you’ve had the tumor and whether the cancer has spread (metastasized).
Advertisement
Healthcare providers have made huge strides in treating synovial cell sarcoma. But there’s still a chance the condition will recur (return), sometimes, many years after treatment. You’ll likely have checkups for several years so your providers can monitor you closely.
The five-year survival rate for synovial sarcoma is 50% to 60%. That means that 5 to 6 out of 10 people with synovial sarcoma are still alive five years after their diagnosis.
The five-year metastasis-free survival rate is 40% to 60%. That means that within five years after treatment, cancer didn’t spread (metastasize) in 4 to 6 out of 10 people with synovial sarcoma.
Survival rates are only estimates and depend on several factors. Researchers base them on previous outcomes for other people diagnosed with the same condition. Survival rates can’t tell you how long you’ll live or how you’ll respond to a specific treatment. To learn more about survival rates — or to find out what they mean for your situation — talk to your healthcare provider.
You can’t prevent synovial sarcoma because you can’t control the chromosomal changes that cause it.
You can lower your risk of metastasis (Stage 4 synovial sarcoma) with early detection and treatment. Stay aware of changes in your body. Tell a healthcare provider if you develop a lump that causes pain or doesn’t go away in a couple of weeks.
Advertisement
Cancer treatments for synovial sarcoma can take a toll on your body. The following can help boost your immune system and help you stay strong:
You’ll have regular visits with your healthcare provider during and after synovial sarcoma treatment. In addition, you should call your provider if you develop any new or worsening symptoms.
You’ll have different questions during diagnosis, treatment and follow up. Some basic questions might be:
Any cancer diagnosis can launch a tidal wave of emotions. But when it’s a rare cancer like synovial sarcoma, it can feel especially isolating. Give yourself time and space to understand your diagnosis and treatment options. Consider joining a support group so you can get to know others who are going through the same thing. And lean on your healthcare team. They’re here to help.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Sarcomas are a rare form of cancer affecting your bones and soft tissues. Our specialists use the latest treatments to care for these types of tumors.
