Shoulder bursitis happens when something damages or irritates the bursae that cushion space between bones and connective tissue in your shoulders. Injuries, overuse and infections can all cause it. You’ll need to rest your shoulder while it heals. Your provider may also suggest anti-inflammatory medications, an antibiotic or physical therapy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
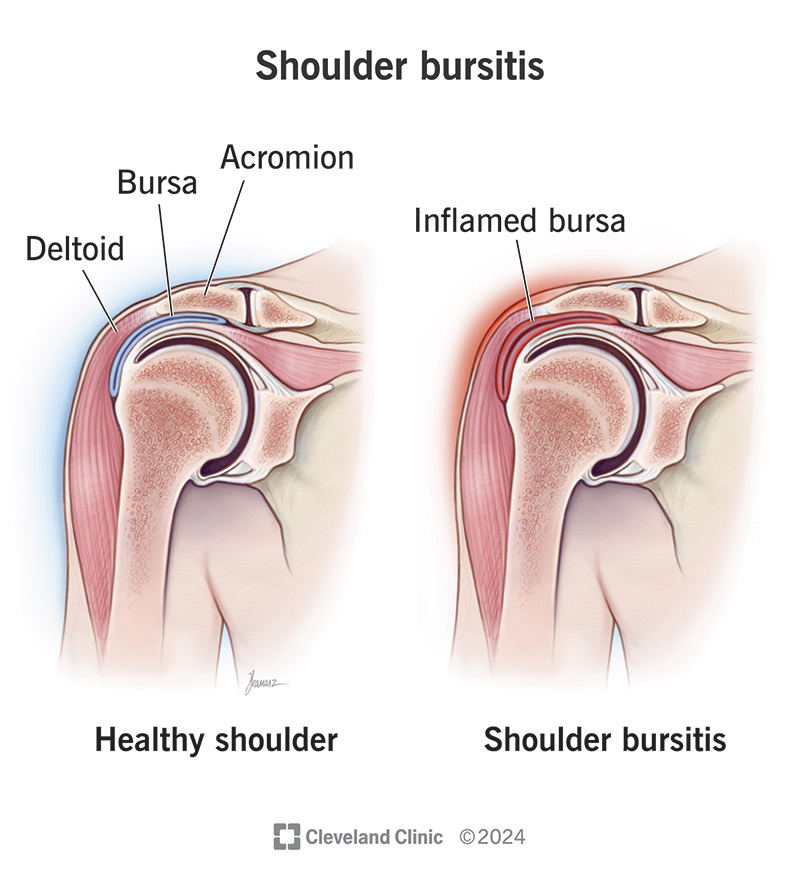
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/shoulder-bursitis)
Shoulder bursitis is bursitis that affects your shoulder joint. The medical name for it is subacromial bursitis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Bursitis is painful swelling in a small, fluid-filled sac called a bursa. Bursae (the plural of bursa) cushion spaces around bones and other tissue.
The subacromial bursae in your shoulder cushion the area between your rotator cuff tendons and the acromion — the highest point of your shoulder blade (scapula).
Shoulder bursitis happens when something damages or irritates the bursae in your shoulder. That causes inflammation that leads to symptoms like pain and swelling.
There are three types of shoulder bursitis:
The most common symptoms of bursitis in your shoulder include:
Advertisement
Shoulder pain from bursitis can come on suddenly or build up gradually. You may feel a dull ache all the time. But the pain may become sharp or feel like a pinch inside your shoulder when you lift your arm over your head.
You’ll probably feel more (or worse) pain if you sleep or lay on your affected shoulder.
Injuries and overusing your shoulder are the most common causes of bursitis. Specifically, sports injuries or repetitive strain injuries are usually what cause chronic and acute shoulder bursitis.
Any injury that damages your shoulder can irritate the bursae and cause inflammation. Using your shoulder for a repetitive motion can irritate your bursae. That’s especially true for movements that require a lot of force — like swinging a hammer or throwing a ball. A motion may not hurt at first, but if you keep doing it often, your shoulder may not have time to heal and irritation can build up over time.
Infections from another place in your body that spread to the bursae in your shoulder cause infectious shoulder bursitis. Bacterial infections (like staph infections) are the most common causes.
Anyone can experience shoulder bursitis. But you have a higher risk if you:
Some conditions that may increase your risk of bursitis include:
Chronic shoulder bursitis and repeated flare-ups (periods of symptoms that come and go) can damage your bursae. Over time, this may affect your shoulder’s mobility (how well you can move it).
Bacteria that cause infectious (septic) shoulder bursitis can spread to organs and other parts of your body if the infection isn’t treated. Severe infections can cause sepsis, which can be fatal. This is rare, but it’s important to see a healthcare provider right away if you think you have an infection.
A healthcare provider will diagnose bursitis in your shoulder with a physical exam to check the pain and your range of motion. Your provider may use a few different tests to diagnose bursitis and rule out other conditions or injuries that cause similar symptoms, including:
Advertisement
Usually, rest is all you’ll need to treat bursitis.
Taking a break from activities that put pressure on your shoulder will give it time to heal. Your provider will tell you how long you’ll need to rest and avoid physical activities.
Other shoulder bursitis treatments include:
Advertisement
It’s rare to need surgery for shoulder bursitis. Your provider will usually only recommend surgery if you have severe symptoms that don’t get better after trying other treatments. You’re more likely to need surgery if you have chronic shoulder bursitis that makes it hard to do all your daily activities.
Shoulder bursitis surgery is usually done with a shoulder arthroscopy. Your surgeon will remove or repair damaged tissue in your shoulder joint. They may also remove the inflamed bursae to create more room inside your shoulder. Your surgeon will tell you what to expect and how long it’ll take to recover.
How long shoulder bursitis lasts depends on which type you have and what caused it. Most people experience symptoms for a few weeks.
Your provider or physical therapist may suggest that you keep managing shoulder bursitis even after your symptoms get better. They may suggest a few months of physical therapy and other treatments to help reduce your risk of the bursitis coming back.
You can reduce your risk of chronic shoulder bursitis by:
Advertisement
You may not be able to prevent acute shoulder bursitis because it happens after sudden injuries you can’t plan for.
It might also be hard to prevent infectious bursitis. You can’t control how an infection spreads inside your body. If you’re taking an antibiotic to treat an infection, take the full dose for exactly as long as your provider prescribes. That’s the best way to make sure it completely kills the infection and reduces the risk of it spreading.
Visit a healthcare provider if you experience:
It may be helpful to ask your provider:
Shoulder pain and a little stiffness are common symptoms after a long day of working in the yard or an intense training session. But if you’re feeling pain that lasts for more than a few days, you might have shoulder bursitis.
You should be able to get back to your usual routine as soon as your shoulder has time to heal. It can be annoying to skip practices, avoid your favorite hobbies or modify how you work, but it’s worth it. Ask your healthcare provider which activities you should take a break from, and which ones are safe to keep doing while you’re resting.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Bursitis can make your hobby or your job a real pain. Cleveland Clinic experts can help you find relief and get you back to doing the things you love.
