Oropharyngeal cancer is a rare cancer that affects your oropharynx (the middle section of your throat). HPV infection, tobacco and alcohol use cause this disease. Symptoms include persistent sore throat, difficulty swallowing and lumps in your neck. Treatment includes surgery, chemotherapy and immunotherapy. Early detection improves survival rates.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
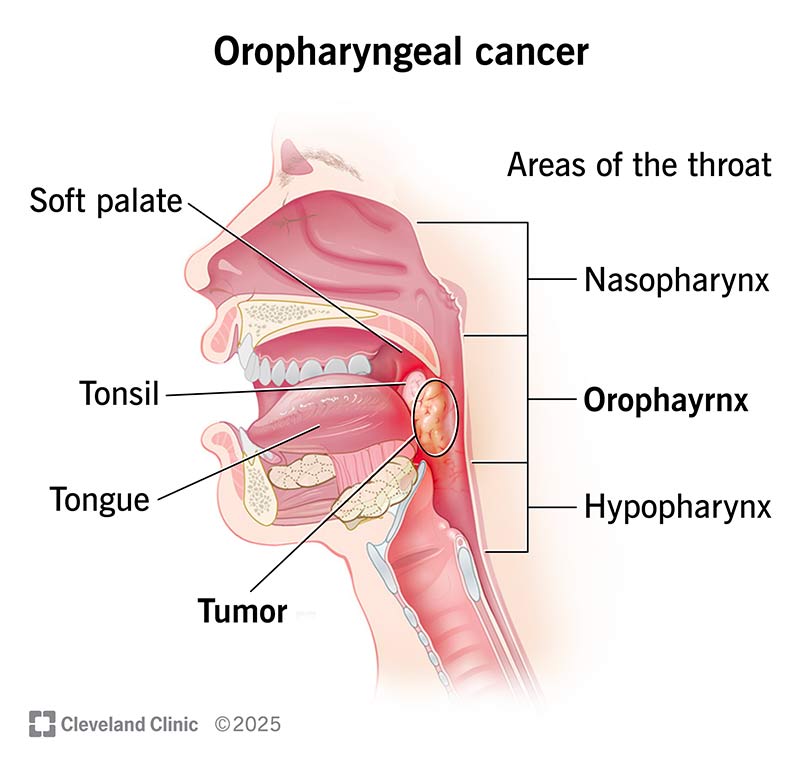
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/12180-oropharyngeal-cancer)
Oropharyngeal (oar-oh-fuh-RIN-jee-uhl) cancer is a rare type of head and neck squamous cell carcinoma. It starts in the squamous cells that line your oropharynx, which is the middle part of your throat. It includes the:
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Oropharyngeal cancer symptoms may feel or look like those that other, less serious conditions cause. Those symptoms include:
Human papillomavirus (HPV) infection is the most common cause. HPV makes proteins that cause changes in certain genes. These genes manage how fast cells divide.
Oropharyngeal cancer develops when the genes stop managing cell growth. Cells then keep dividing and form cancerous tumors. That process takes many years. For example, a teenager with HPV may develop oropharyngeal cancer 30 to 40 years later.
Other causes include:
Advertisement
Other issues may increase your risk, including:
Making some lifestyle changes may help reduce your risk. Changes you can make include:
A provider will ask about your symptoms. They’ll ask about your medical history, including whether you’ve had medical issues that increase your risk, like:
They’ll also ask about your personal habits. For example, they’ll ask if you use tobacco now or have in the past. They may ask how often you drink beverages that contain alcohol, and how much you drink.
Your provider may check the inside of your mouth and throat. They’ll gently feel your neck for lumps.
Your provider may use a thin, flexible tube with small tools to get tumor tissue samples. A medical pathologist will check the samples under a microscope for signs of cancer and HPV.
If tests show you have a cancerous tumor, your provider may do other tests to learn more about it. These include:
Your provider uses test results to stage the cancer. Staging cancer helps them plan treatment and develop a prognosis (outlook).
There are two oropharyngeal cancer staging systems. Both systems set cancer stages based on:
Advertisement
Both systems involve four stages, from Stage I to Stage IV. The difference is whether tests show you have HPV. If you do, your provider may say you have HPV-positive oropharyngeal cancer.
Treatment focuses on ways to remove the tumor so you can speak and swallow as normally as possible. Your treatment may involve:
Go to the emergency room or talk to your healthcare provider if you have surgical wound infection symptoms, like:
Advertisement
Oropharyngeal cancer can come back, so you may need regular checkups for the rest of your life. Your provider may do checkups every six to 12 weeks during the first year after treatment. You’ll have fewer regular checkups over time.
Sometimes, surgery to remove small tumors cures this disease. Survival rates for oropharyngeal cancer vary depending on the tumor location. According to the National Cancer Institute (U.S.), overall, 7 out of 10 people with this disease are alive five years after their diagnoses. Survival rates by tumor location are:
It’s important to remember that cancer survival rates are estimates based on other people’s experiences with specific kinds of cancer. Your experience may be very different. Ask your healthcare provider to explain what survival rate estimates mean in your situation.
Advertisement
Cancer surgery and treatment can be physically and emotionally challenging. If you have oropharyngeal cancer, the following programs may help you manage those challenges:
No. They’re different forms of head and neck cancer. Oral cancer is cancer in your mouth. This includes the:
Oropharyngeal cancer affects the middle of your throat, the back of your tongue and soft palate, and the sides and back of your throat.
Oropharyngeal cancer is a rare, serious complication of human papillomavirus (HPV). This is a common sexually transmitted disease. You can have HPV without knowing it. Many years later, you may learn the virus triggered changes that caused oropharyngeal cancer. Surgery can cure this disease if it’s caught early on.
If you had an HPV infection or tests to detect the virus, ask a healthcare provider about your risk for developing oropharyngeal cancer. They’ll explain the symptoms the disease causes, like a sore throat that doesn’t go away. They’ll also explain what you can do to reduce your risk.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you learn you may have oral cancer, you’ll want the best care. Cleveland Clinic’s head and neck cancer experts offer personalized treatment and support.
