Retinoblastoma is a rare eye cancer that affects children. It happens when cells in the retina at the back of the eye multiply and form tumors. The main symptom is leukocoria, which is when your child’s pupil looks white. You may spot the issue when you look at photographs of your child.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
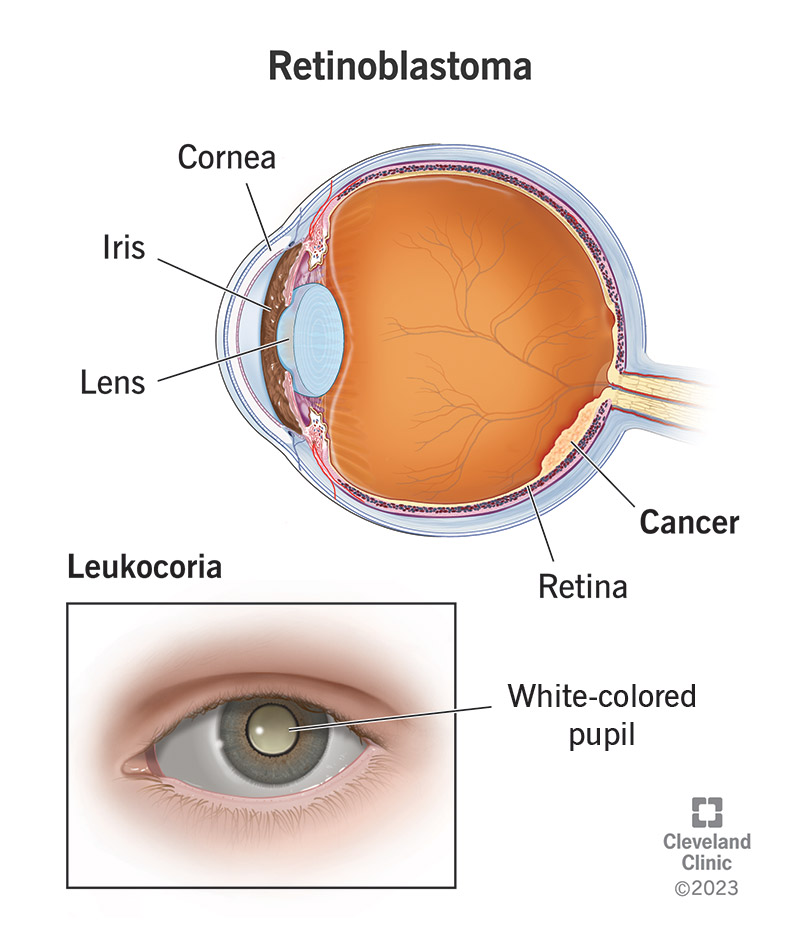
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/10706-retinoblastoma)
Retinoblastoma is a rare eye cancer that starts in your child’s retina. This is the area at the back of your eye that senses light. Most children receive a diagnosis before age 3. Early diagnosis and treatment can cure retinoblastoma. But the disease can lead to vision loss or blindness.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There are three types of this cancer:
Leukocoria is the earliest and most common symptom. Your child’s pupil may look white. You may notice the unusual color in photographs taken with a flash in dim light. Other symptoms include:
A genetic change (mutation) causes this disease. Retinoblastoma happens when the RB1 gene changes (mutates). The RB1 gene manages how quickly retinal cells multiply. In retinoblastoma, the cells multiply and form tumors.
The genetic change may happen for no known reason. Some children inherit the change from their biological parents. Healthcare providers may call this heritable or hereditary retinoblastoma. Children with hereditary retinoblastoma typically have it in both eyes.
Retinoblastoma has autosomal dominant inheritance. If both parents have the changed gene, there’s a 75% chance that their child will inherit it. If one parent has the gene, the chance drops to 50%.
Advertisement
Retinoblastoma complications include:
Ophthalmologists or eye care specialists will do an eye examination. They’ll use medication that dilates your child’s pupil so they can look at the inside of your child’s eye. They may do imaging tests like:
There are several ways to treat retinoblastoma. Your child may have a combination of treatments, including:
Contact your child's pediatrician if you notice any signs of retinoblastoma or any changes in their eyes or vision. They’ll check your child’s eyes for issues like leukocoria. Diagnosing retinoblastoma early on may help protect your child’s vision. If your child has retinoblastoma, let their ophthalmologist know if they have new symptoms.
Talk to your healthcare provider if you or your partner has a biological family history of retinoblastoma or you know you have the RB1 gene mutation. You may want to consider genetic counseling before having children.
The prognosis for retinoblastoma is good. According to the American Cancer Society, treatment cures retinoblastoma in 9 out of 10 children with the disease. But your child will need regular eye exams and physical exams. Their ophthalmologist will look for signs that retinoblastoma has come back. Their pediatrician will check for any long-term side effects from cancer treatment.
Your child may be a toddler when tests show they have retinoblastoma. They’ll be too little to understand what’s happening. But they’re likely to be upset and scared by all the changes in their life. Even if your child seems fine, it’s a good idea to talk to a child life specialist. They can help your child manage the stress that medical care can cause. They also offer emotional support to you and other family members.
Advertisement
Cancer treatment can cause side effects that may be hard on your child and on you. Your child’s healthcare team can recommend ways to ease side effects. More than that, they can help you and your child manage the stress of dealing with a serious disease like retinoblastoma.
Research shows retinoblastoma survivors often experience anxiety, especially during adolescence. Individuals who inherited the changed RB1 gene that causes retinoblastoma may worry about passing it on to their children. Adolescence is tough in the best of times. Talking to a counselor may help your child.
Treatment often cures retinoblastoma, the rare eye cancer that starts in childhood. Even so, this disease can have a long-term impact on children and those who care for them. Share your concerns with your child’s healthcare team. They’ll recommend programs and services that can support your child as they manage the lifelong changes that retinoblastoma may cause.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Your eyes are one of your most important senses. If something goes wrong, it can change your world. Cleveland Clinic can help treat all types of retinal disease.
