During an EGD procedure (upper endoscopy), a digestive tract specialist (gastroenterologist) uses a scope to view the inside of your esophagus, stomach and duodenum (the upper part of your small intestine). Providers use the procedure to diagnose and treat acid reflux, stomach ulcers, celiac disease and other digestive tract problems.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
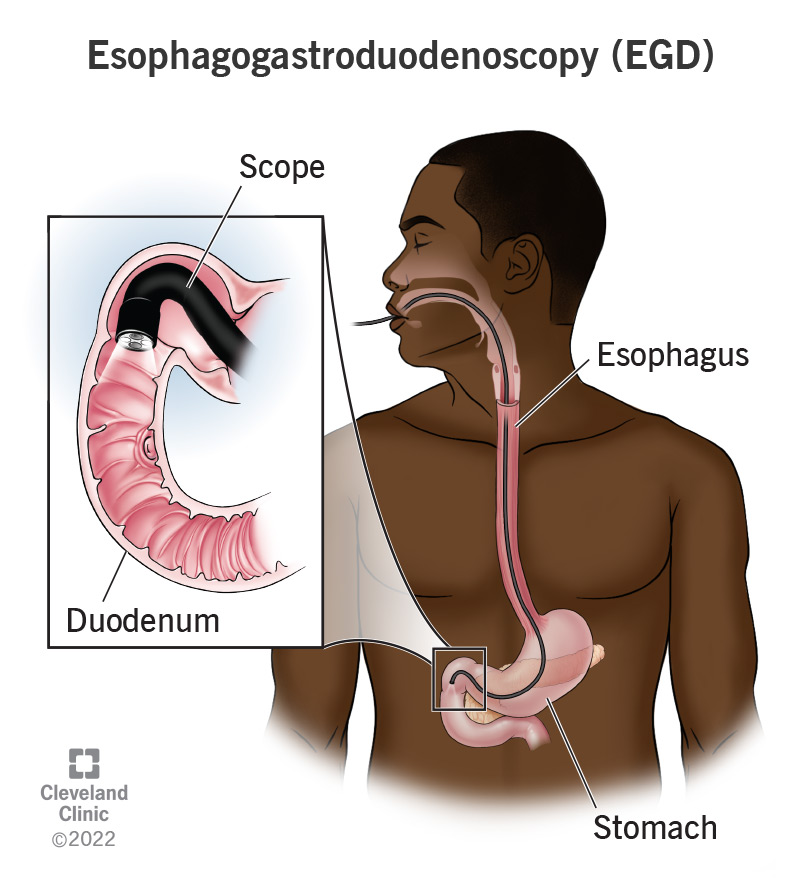
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22549-esophagogastroduodenoscopy)
An EGD, or upper endoscopy, is a procedure to examine the upper part of your digestive tract. EGD stands for “esophagogastroduodenoscopy.” Phew! Let’s break that down.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Working backward through the word, “-scopy” means an examination with a visual instrument. A “scope” is that instrument (as in “telescope” or “microscope”). During an EGD procedure, a gastrointestinal (GI) doctor (gastroenterologist) uses an instrument called an endoscope to examine the inside of your body. The endoscope is a small, lighted camera on the end of a long, flexible tube.
After a healthcare provider gives you medication to make you comfortable, your gastroenterologist passes the endoscope down your mouth, then your throat, through your esophagus (swallowing tube), into your stomach and then into your duodenum (the upper part of your small intestine). The camera sends images to a computer screen showing your esophagus, stomach and duodenum. Similarly, your gastroenterologist can visually examine these areas of your body.
That’s where the rest of the word comes from. “Duodeno-” means duodenum, “gastro-” means stomach and “esophago-” means esophagus.
You may need an upper endoscopy if you have unexplained symptoms like:
An upper endoscopy allows for a direct view into your upper digestive system. It can be more accurate than X-rays in diagnosing problems. These problems include:
Advertisement
Healthcare providers can also do treatments with an endoscope. They might want to take a tissue sample to examine in the lab (biopsy). They can do these things with the endoscope.
By attaching tiny tools to the endoscope, EGD technicians can often fix small problems on the spot. For example:
EGD is a simple outpatient procedure that shouldn’t take more than an hour of your day. But you’ll have to prepare in a few ways ahead of the appointment:
When you arrive for your EGD, a provider will lead you to the endoscopy suite. A nurse will check your vital signs to make sure you’re in good condition for the procedure. Then, your nurse will install an intravenous (IV) catheter into a vein in your arm to deliver your medicine.
If you have general anesthesia, the medication will put you completely to sleep. You won’t feel anything. But most people will have conscious sedation instead. A provider who specializes in anesthesia (anesthesiologist) will give you a sedative to make you feel sleepy and relaxed, but you may not be completely asleep. With the sedative, a provider will also spray a local anesthetic spray into your mouth and throat. This has a numbing effect.
Your nurse will place a mouthguard in your mouth to protect your teeth, tongue and the scope. They’ll position you on your left side on the procedure table.
To perform the procedure, your provider:
Advertisement
An upper endoscopy is typically an outpatient procedure, meaning you go home the same day. The procedure may be uncomfortable, but it shouldn’t be painful.
The procedure takes about 30 to 60 minutes.
Your provider will suction the air out of your stomach after withdrawing the endoscope. But there may be some gas left in there. This will pass over the next day or so. Side effects may include bloating and passing gas (burping and farting).
You may also have a sore throat for a day or two as the numbing agent wears off. Cold foods and drinks can help soothe your throat. Your healthcare provider may recommend some more specific food-related guidelines for the days following the test.
You may not remember the test afterward. You’ll need to stay at the medical office until you’re alert enough to be discharged. In some cases, your healthcare provider may be able to discuss the test results with you right away. In other cases, you may need to make a separate appointment.
An EGD is a minimally invasive procedure that allows a healthcare provider to examine the inside of your upper digestive tract. They’re able to diagnose, biopsy or treat conditions without the risks of traditional surgery. The procedure is painless, and you can go home the same day.
Advertisement
An upper endoscopy is a relatively low-risk procedure. Potential complications include:
If you don’t have results immediately after the test, it might be because your healthcare provider needs to wait for biopsy results. This can take up to two weeks. As soon as your healthcare provider has results to share, they’ll be able to discuss what they found, what it means and what comes next.
You should call your healthcare provider if you experience:
There are many types of endoscopy procedures. Esophagogastroduodenoscopy (EGD) is just one of them. All endoscopies use the same tool — the endoscope — to examine different parts of your body. The exams have different names to describe the different parts they’re looking at.
An EGD test looks at what healthcare providers sometimes call the upper gastrointestinal (GI) tract: your esophagus, stomach and duodenum. This is the part of your digestive system that the endoscope can reach from the top down. Sometimes, providers call an EGD an upper endoscopy.
Advertisement
Esophagogastroduodenoscopy may have a whopper of a name, but it’s a simple procedure. It’s normal to worry about it, but you should know that it’s short and painless. Healthcare providers appreciate how well the endoscope visualizes your internal organs, and even allows them to take samples and make quick repairs. You and your healthcare provider can learn a lot from an EGD about what’s going on in your body, and sometimes even fix it.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Having an endoscopy can be lifesaving. Cleveland Clinic’s providers will help you feel comfortable with the process so you can get the care you need.
