Together, your superior vena cava and inferior vena cava collect deoxygenated blood from your whole body and bring it back to your heart for new oxygen. This is why the vena cava veins are the largest veins in your body. Your upper body veins send blood to your superior vena cava and your lower body veins empty blood into your inferior vena cava.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
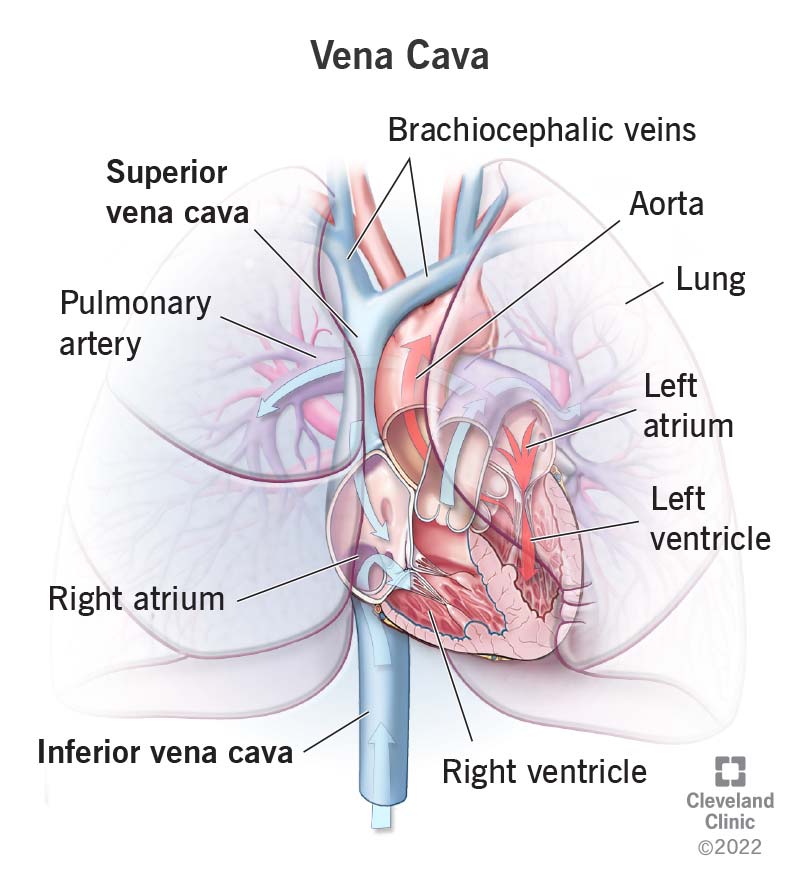
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/22619-vena-cava)
The superior vena cava and inferior vena cava are very large veins that bring deoxygenated blood to your heart to get oxygen. Your inferior vena cava, your body’s largest vein, carries oxygen-depleted blood back to your heart from the lower part of your body (below your diaphragm). Your superior vena cava, your second biggest vein, brings oxygen-poor blood from your upper body to your heart.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Think of it like a bus line. The downtown line is like the smaller veins from your lower body (such as veins from your kidneys, liver and lower back area) that bring deoxygenated blood into your inferior vena cava. Blood from those other veins gets on the inferior vena cava bus to go to your heart.
Your uptown line (upper body) veins, such as the veins in your upper back and chest, take deoxygenated blood onto your superior vena cava bus for return to your heart. Your heart is the hub or destination where all the deoxygenated blood from the uptown and downtown bus lines (veins) goes.
Your superior vena cava and inferior vena cava have the important function of carrying oxygen-poor blood to your heart’s right atrium, where it moves into your right ventricle and then to your lungs (through your pulmonary artery) to trade in carbon dioxide for oxygen. Oxygenated blood comes back through your pulmonary veins to your heart’s left atrium. From there, blood that now carries fresh oxygen goes to your left ventricle and to your aorta for distribution to your body.
Your inferior vena cava and superior vena cava are both on your heart’s right side. Your right and left innominate (or brachiocephalic) veins merge to form your superior vena cava.
Advertisement
Your superior vena cava is next to the right side of your sternum and goes into your right atrium, where all the oxygen-poor blood goes. Your inferior vena cava is a little longer. It starts where the right and left common iliac veins come together in your belly area and goes up into the right atrium of your heart.
Your superior vena cava is a large vein that doesn’t have a valve.
Your inferior vena cava is a large and long vein that has one valve where it meets your right atrium.
These are your body’s largest veins. Your superior vena cava is 7 centimeters long (almost 3 inches) and 2 centimeters (less than 1 inch) wide.
Your inferior vena cava is about 100 millimeters (4 inches) long and 22 millimeters (less than 1 inch) in diameter.
Your superior vena cava and inferior vena cava include:
You can get an obstruction in your superior vena cava and inferior vena cava that makes it hard for blood to flow through them. When this happens, you can also call it superior vena cava syndrome or inferior vena cava syndrome, depending on which part of the vena cava has a blockage.
Causes of these obstructions include:
When something is pushing against your superior vena cava or inferior vena cava or blocking blood flow inside them, these symptoms can happen:
Your healthcare provider has several ways to get images of your superior vena cava and inferior vena cava, including:
Your healthcare provider can use similar treatments for problems with your superior vena cava and inferior vena cava. They can:
Advertisement
If you have a deep vein thrombosis (DVT) with a risk of the blood clot going from your legs or pelvis to your lung (pulmonary embolism), your healthcare provider may put in a vena cava filter to catch blood clots and keep them from going to your lungs.
You can care for your vena cava like you care for the rest of the many blood vessels you have in your body.
If you have an obstruction in your superior vena cava or inferior vena cava, your healthcare provider has a number of options to treat it. Talk to them about which treatment is best for your situation. If they prescribe medicines, be sure to keep taking them according to the instructions. Go to all of your follow-up appointments to ensure a good recovery from any procedures you may have.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
