Many things can cause blood in your urine, including urinary tract infections, vigorous exercise and chronic kidney disease. But you shouldn’t ignore it. Healthcare providers can diagnose the cause and recommend the best treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
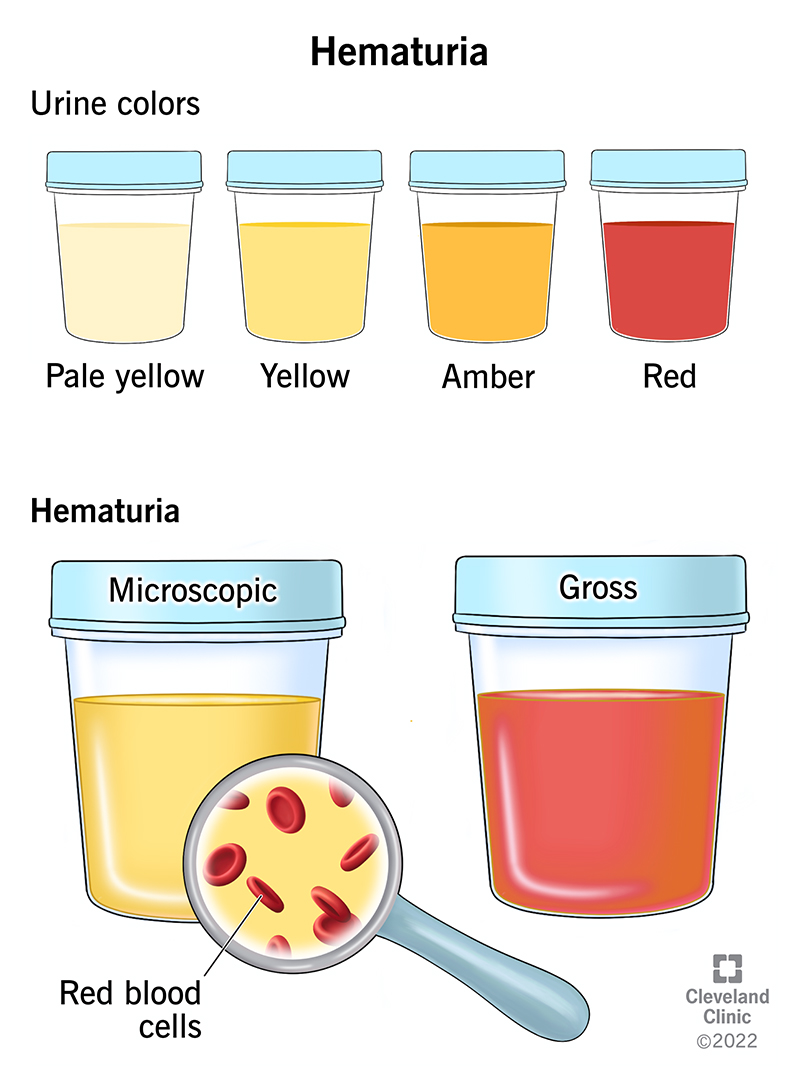
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/hematuria)
Hematuria (hee-muh-TOOR-ee-uh) is the medical name for the presence of blood cells in your urine (pee).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It’s pretty common for blood to be in your pee. But you may not even know it because it doesn’t always turn your pee pink or red. Sometimes, there’s only a small amount of blood in your pee that you can’t see — healthcare providers discover it during a urine test.
But if you notice your pee looks pink or red or you have other hematuria symptoms, it might be a sign that something is wrong. You should reach out to a healthcare provider.
Healthcare providers label blood in pee as:
Dipstick tests have relatively high false-positive rates. A false-positive rate is when the dipstick test says you have blood in your pee, but you don’t. Providers need to confirm dipstick hematuria with a microscopic urinalysis.
Advertisement
Hematuria is common. Medical experts estimate that more than 20% of people who receive an evaluation from a urologist have blood in their pee. Microscopic hematuria affects an estimated 2% to 31% of people. Microscopic hematuria is more common than gross hematuria.
Many times, there are no symptoms except blood in your pee. When this happens, a healthcare provider may say you’re “asymptomatic.”
If you have other symptoms, they may include:
You may have other associated symptoms, too, including:
Having blood in your pee doesn’t always mean you have a condition. But it can be an important warning sign that something is wrong with your body. Don’t ignore it. Contact a healthcare provider as soon as you find blood in your pee.
There are many different causes of hematuria. Some conditions are more serious than others. Serious conditions may include:
Certain cancers can also cause blood to appear in your pee.
Other conditions that may lead to blood in your pee include:
Different types of cancer can cause blood to appear in your pee. These include:
No, hematuria isn’t contagious. But a common cause of hematuria is UTIs. Healthcare providers don’t consider UTIs contagious. But sometimes, you can spread the bacteria that cause UTIs to a partner during sexual intercourse.
Advertisement
Anyone of any age can have blood in their pee. But you may be more likely to have hematuria if you:
You may experience side effects of hematuria treatments, including medications and procedures. They vary by treatment, and a healthcare provider will review any possible side effects with you.
But untreated hematuria can lead to bigger problems, especially if the cause is serious. A provider should treat any condition that causes blood in your pee. Early detection of a serious condition leads to early treatment. Your chances of successful treatment increase the sooner you get treatment.
A healthcare provider will review your medical history, ask you questions about any other symptoms and perform a physical examination, which may include a pelvic exam or digital rectal exam. They may also recommend additional tests to help confirm a hematuria diagnosis.
Advertisement
A healthcare provider may recommend the following tests to help diagnose hematuria:
Hematuria treatment depends on its cause. A healthcare provider will use the information they collect from your medical history, physical exam and any test results to find the best treatment.
Depending on the cause, a healthcare provider may recommend the following medications to treat hematuria:
| Cause | Medication |
|---|---|
| Infections | Antibiotics can treat an infection. |
| Enlarged prostate | Providers typically use alpha-blockers and 5-alpha-reductase inhibitors, including finasteride (Proscar®) and dutasteride (Avodart®). |
| Cancer | Treatment will be appropriate to the staging and your goals of care. It may include surveillance, surgery, radiation therapy, immunotherapy, chemotherapy, hormone therapy or a combination of these options. |
| Sickle Cell Disease | A provider may prescribe disease-modifying agents like hydroxyurea, pain medications, antibiotics and drugs that prevent blood cells from dying or forming into sickles. |
| Chronic kidney disease | A provider may prescribe different types of medications, including diuretics, blood pressure medication (antihyperintensives), cholesterol-lowering drugs (antihyperlipidemics) and erythropoietin to build red blood cells if you have anemia. |
| Endometriosis | Hormone-related medications, including hormonal birth control, gonadotropin-releasing hormone (GnRH) antagonists or agonists and danazol (Danocrine®). |
| Cause | |
| Infections | |
| Medication | |
| Antibiotics can treat an infection. | |
| Enlarged prostate | |
| Medication | |
| Providers typically use alpha-blockers and 5-alpha-reductase inhibitors, including finasteride (Proscar®) and dutasteride (Avodart®). | |
| Cancer | |
| Medication | |
| Treatment will be appropriate to the staging and your goals of care. It may include surveillance, surgery, radiation therapy, immunotherapy, chemotherapy, hormone therapy or a combination of these options. | |
| Sickle Cell Disease | |
| Medication | |
| A provider may prescribe disease-modifying agents like hydroxyurea, pain medications, antibiotics and drugs that prevent blood cells from dying or forming into sickles. | |
| Chronic kidney disease | |
| Medication | |
| A provider may prescribe different types of medications, including diuretics, blood pressure medication (antihyperintensives), cholesterol-lowering drugs (antihyperlipidemics) and erythropoietin to build red blood cells if you have anemia. | |
| Endometriosis | |
| Medication | |
| Hormone-related medications, including hormonal birth control, gonadotropin-releasing hormone (GnRH) antagonists or agonists and danazol (Danocrine®). |
It depends on the cause of hematuria.
When an enlarged prostate causes blood in your pee and medications don’t treat it, a healthcare provider may suggest surgery. There are many different types of surgery to remove prostate tissue and stop prostate bleeding. A healthcare provider will review your options.
Advertisement
For cancers, you may need multidisciplinary care. Multidisciplinary care is when you have a group of healthcare providers who specialize in different diseases or conditions that affect different parts of your body. This may include:
Hematuria usually isn’t life-threatening. But sometimes, the cause of hematuria is serious. If you notice blood in your pee, schedule a visit with a healthcare provider so they can determine the cause.
Your outlook depends on what’s causing hematuria. But in general, your outlook is good. Hematuria may go away without treatment. Or it may go away pretty easily with treatment. A healthcare provider will tell you what to expect according to your specific cause.
You can’t prevent all causes of hematuria. But you can help prevent some causes by:
You may decrease your chances of certain conditions that cause hematuria by drinking enough fluids — preferably, water. Water is good for your urinary system and your body.
If you don’t drink enough water, your pee may be darker in color. If you’re extremely dehydrated, you could possibly have bloody pee.
Contact a healthcare provider if the water in your toilet looks pink or red after you pee.
But some types of hematuria aren’t obvious. In those cases, it’s important to talk to a healthcare provider if you have symptoms that relate to hematuria, like:
If any of your symptoms are severe, you should visit urgent care.
You may wish to ask a healthcare provider the following questions:
No, foods and drinks can’t cause hematuria. But certain foods can make you think you’re peeing blood because your pee looks pink, red or dark brown. These include:
There’s no need to panic if you notice your pee is pink or red. You may have blood in your pee if you have your period. Or maybe you recently ate a lot of beets. But it’s still a good idea to give a healthcare provider a call. It’s better to catch any cause of hematuria early, even if the cause isn’t serious. A provider will work with you to find out what’s causing blood in your pee and recommend the best possible treatment.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you see blood in your child’s urine, it’s time to call the doctor. Cleveland Clinic’s pediatric hematuria experts are here to help.
