Cystoscopy is a procedure providers use to diagnose and treat urinary tract problems. You might need cystoscopy if you have blood in your pee, painful urination, leaking pee or an inability to pee. During a cystoscopy, a urologist uses a scope to view the inside of your bladder and urethra.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
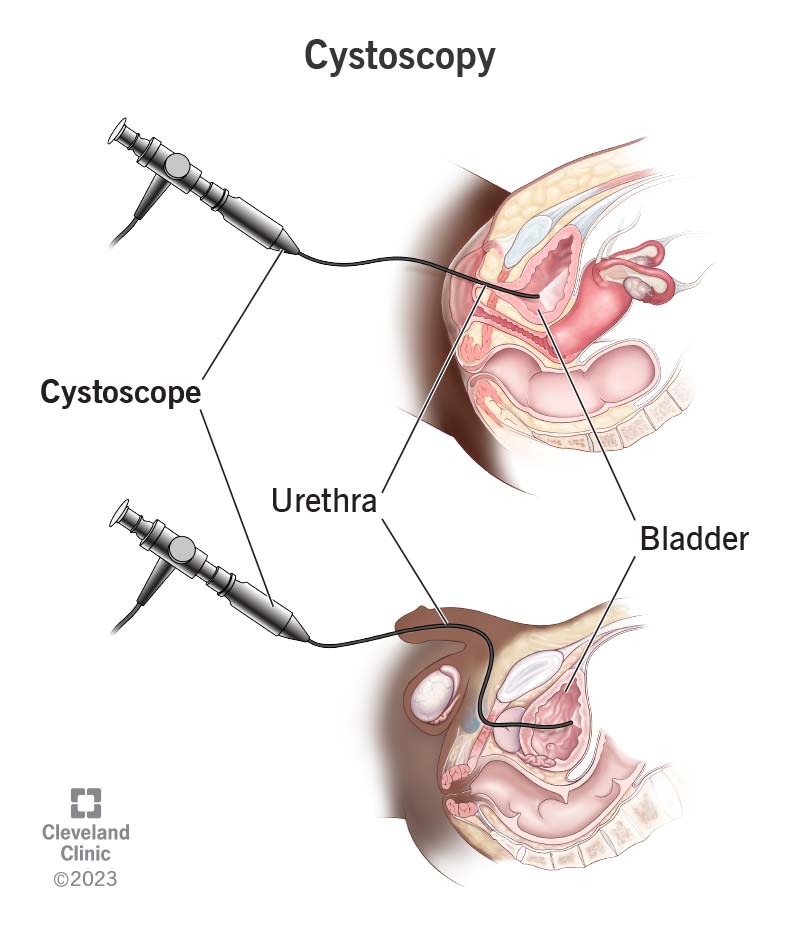
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/cystoscopy)
Cystoscopy is a procedure healthcare providers use to view the inside of your bladder and urethra (the tube that drains pee from your bladder out of your body). A urologist performs it with a lighted device with a camera or viewing lens (cystoscope).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Urologists use cystoscopies to diagnose and treat urinary tract problems. They can use it to rule out serious conditions, like bladder cancer, as a cause of your symptoms. Your urologist may also use a cystoscope to:
A cystoscopy can diagnose:
Your healthcare provider may recommend a cystoscopy if you’re experiencing:
Advertisement
To perform a cystoscopy, a urologist will insert a cystoscope into your urethra and up to your bladder. There, they can look inside your bladder and use instruments to remove samples of tissue, or perform other tests or treatments.
There are two types of cystoscopes:
Your healthcare provider will use the one that works best for your specific procedure.
If your provider is performing the procedure to help them diagnose an issue, yes, you’ll likely be awake during cystoscopy. They’ll use a numbing gel so you don’t feel pain. If you’re getting treatment or if your provider is performing a biopsy during cystoscopy, you may need sedation or general anesthesia.
Before cystoscopy, tell your provider about any medications you’re taking and if you might be pregnant. Your provider will give you instructions on how to prepare. Following their directions closely can reduce your risk of complications.
Your preparation will mostly depend on the anesthesia type and why you’re having the procedure. Before a cystoscopy, your provider may ask you to:
To perform a cystoscopy, a healthcare provider will:
Advertisement
A diagnostic cystoscopy usually takes about five to 10 minutes. The procedure may take longer if you’re having a biopsy or treatment.
A cystoscopy may feel uncomfortable, or you might feel like you need to pee. But general anesthesia or a numbing gel keeps you from feeling pain.
Depending on the reason for the cystoscopy, you may have an outpatient procedure (go home the same day) or stay overnight in the hospital. When you go home, your provider may prescribe antibiotics to prevent infection. Take any medications as prescribed.
Most people recover within a day or two from a cystoscopy. It may take longer depending on whether you had additional procedures at the same time (like a biopsy). Ask your provider what to expect.
You may have belly pain, blood-tinged pee or pain and/or burning when peeing for the first day or two after the procedure. You might also feel like you need to pee often and urgently.
To ease these symptoms, you can:
A cystoscopy is a relatively low-risk procedure. Potential complications include:
Advertisement
Your urologist will make notes about anything they notice during the procedure. This includes blockages, narrowing of your urethra, bladder stones, abnormal tissue or growths. They’ll also note if everything looks normal. They might talk to you about the results soon after the procedure or schedule a follow-up appointment to talk about them.
If your provider took samples of tissue for biopsy, a lab will look at them under a microscope for cancerous cells.
If you had a biopsy, it may take up to two weeks for your provider to get the results. If your provider is only doing a cystoscopy (no other procedures at the same time), they’ll know the results as they perform the procedure. Ask your provider when you should expect to see your results in your records or to hear from them.
Most post-procedure problems like painful urination and blood-tinged pee get better within a day or two. Call your healthcare provider if problems last longer or you experience:
Advertisement
Symptoms like pain, blood in your pee or an inability to control when you pee can make you feel anxious for answers about the cause. Cystoscopy is a way for your provider to start getting those answers. It’s a quick procedure with minimal risks and a short recovery time. Don’t hesitate to ask your provider about any concerns you have before or after the procedure. They can help you understand what to expect and make sense of the results.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a condition that’s affecting your urinary system, you want expert advice. At Cleveland Clinic, we’ll work to create a treatment plan that’s right for you.
