The intragastric balloon is a new, minimally invasive bariatric treatment for people with obesity. The balloon is a medical implant that a healthcare provider places in your stomach to restrict its capacity for a limited time. The provider uses an endoscope to pass the balloon down your throat, so there’s no surgery involved.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
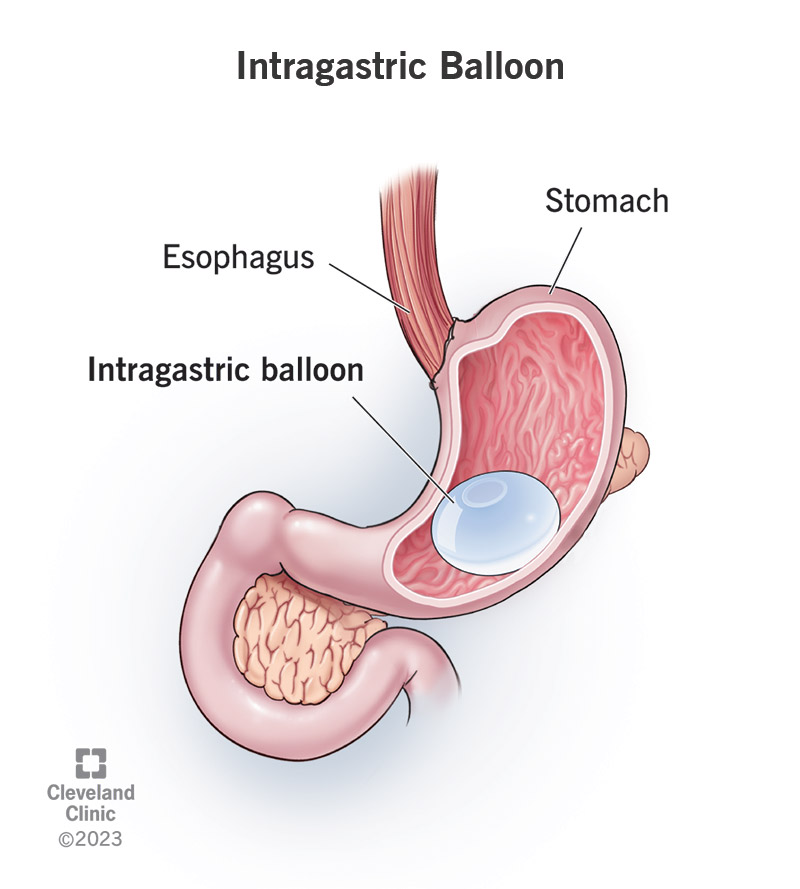
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/24773-intragastric-balloon)
The intragastric balloon system is a minimally invasive medical weight loss program for people with obesity. It combines long-term diet and lifestyle changes with a short-term medical implant. The implant is an inflatable balloon that a healthcare provider places nonsurgically inside your stomach (which is what “intragastric” means). It works by taking up space, making you feel full and restricting how much you can eat.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
When you have obesity, your body changes in ways that make it increasingly hard to lose weight by diet and exercise alone. One of those changes is that the volume of your stomach expands over time. As your stomach stretches, it holds more food and takes longer for you to feel full, which leads to eating more. This is why all medical weight loss procedures restrict the capacity of your stomach by some means.
The intragastric balloon offers an important alternative to the other available procedures. First, it’s the only procedure that’s designed to be impermanent. Second, it doesn’t require surgery to install it. It doesn’t require general anesthesia, either. This makes it a viable option for those who either don’t meet the qualifications for bariatric surgery or are looking for a lesser commitment.
In the U.S., the intragastric balloon is currently offered to people with a BMI of at least 30 who pass the health screening for the procedure. People with class III obesity who qualify for bariatric surgery may choose the balloon instead for its relatively low risks. People whose obesity makes surgery unsafe for them may use the balloon as a bridge procedure to lose enough weight to qualify for surgery.
Advertisement
Obesity causes metabolic changes that lead to a wide range of health conditions, from Type 2 diabetes and cardiovascular disease to kidney and liver diseases. If you have a BMI of 30 or more, you’re at a high risk of developing these diseases. But on the flip side, weight loss of just 5% to 10% reduces this risk and can even cause remission of these conditions. You can achieve this with the intragastric balloon system.
Average weight loss with the gastric balloon is about 10% of your total weight or about 30% of your excess weight. That’s enough to make a life-changing impact on your health in a short period. As with any weight loss system, you can lose more or less depending on how well you stick to the program. You can also regain the weight you lost if you don’t stick to the program after the balloon is removed.
The intragastric balloon is the newest FDA-approved medical procedure for weight loss. The U.S. Food and Drug Administration approved the first model, the Orbera®, in 2015. Providers recommend this model the most because it has the most research behind it. Endoscopic bariatric therapy in general is still new, but the intragastric balloon is the most commonly performed endoscopic bariatric procedure.
You’ll consult with your healthcare provider to determine if you’re a good fit for the intragastric balloon system. If you are, your healthcare provider will assemble a team of caregivers to support you through the program. You’ll consult with a nutritionist, gastroenterologist, psychologist/psychiatrist and possibly others to design a personalized weight loss program.
Your healthcare provider may not advise it if you have:
A healthcare provider will explain the risks, benefits and alternatives to the procedure and obtain your informed consent to proceed. They’ll often start you on acid-blocking medication to prevent acid reflux during and after the procedure. A few days before the procedure, they’ll put you on a clear liquid diet to help empty your stomach. The night before, they’ll ask you not to eat and drink anything after midnight.
Healthcare providers insert most intragastric balloons using an endoscope. An endoscope is a long, flexible tube with a camera attached. It goes in through your mouth and passes down through your esophagus to reach your stomach. Most people have this procedure while awake, but with a mild sedative. (The Obalon® is a newer balloon that you can swallow, but it still has to be removed by endoscope.)
Advertisement
You’ll have medication to help relax you and numb your throat for the endoscope. Your gastroenterologist or endoscopic surgeon will begin by examining your esophagus and stomach with the endoscope, which projects images onto a screen. Once they’re satisfied that you don’t have any conditions that could make the balloon unsafe, they’ll guide the balloon into place.
The Orbera balloon is filled with a sterile, saline solution, as most models are. The Obalon — as well as some others available outside of the U.S. — is filled with gas. Providers don’t use gas-filled balloons as often because they aren’t as effective overall for weight loss, but they can be more comfortable. Providers recommend them for certain people and circumstances, based on their characteristics.
Your endoscopist will fill the balloon with a syringe attached to the catheter, then detach the syringe and withdraw the catheter. The valve on the balloon seals to prevent leaks. The filled Orbera balloon takes up about a third of your stomach. The weight of the fluid makes it sink to the bottom, which is part of how it works. It slows down the emptying of your stomach through the valve at the bottom (pylorus).
The procedure itself takes 20 to 30 minutes. Afterward, you’ll spend a few hours recovering in the hospital. You’ll have IV fluids and medication to prevent pain and nausea. Your healthcare team will make sure you’re tolerating the balloon before they discharge you. They’ll also leave you with dietary instructions to follow in the weeks ahead. You’ll stay on a clear liquid diet for the rest of the day.
Advertisement
Your stomach will need time to adapt to the balloon before you resume your regular diet. You’ll start with a liquid diet and gradually advance to pureed foods, followed by a soft diet, and finally, the long-term diet designed by your nutritionist. You’ll stay in close contact with your healthcare team during this time. They’ll support you through the physical and psychological side effects while you’re adjusting.
The Orbera balloon stays in place for six months. During this time, you’ll continue to work with your team to make the diet and lifestyle changes that will sustain your weight loss over the long term. You’ll eat less, lose weight and retrain yourself to notice when you’re getting full. You’ll continue acid-blocking and anti-nausea medications as needed. The greatest weight loss happens in the first three months.
You’ll have a second endoscopic procedure to remove the balloon. You’ll be given a sedative and a topical anesthetic or lubricant in your throat to ease the removal. Your endoscopist will puncture the balloon, suction out its filling and then withdraw the deflated balloon. After the balloon comes out, your team will continue to work with you for six more months to reinforce your long-term lifestyle changes.
Advertisement
Side effects of mild gastrointestinal symptoms are common, and healthcare providers often prescribe medication to prevent or manage them. Symptoms usually only last a week or so, but sometimes longer. They include:
It’s usually more of a dull discomfort than acute pain, and it usually doesn’t last. Some people experience more noticeable pain during the first week after the procedure, but it’s manageable with medication.
Serious complications are rare, but they can occur. The risks include:
Most people lose a significant amount of weight with the intragastric balloon, enough to experience relief from many of the physical and psychological complaints that can come with obesity. The average weight loss of 10% is more than most people can achieve through lifestyle interventions alone. This experience can be a revelation that motivates people to maintain or continue their weight loss.
But the procedure itself isn’t permanent, and there’s nothing to stop you from regaining the weight after completing the program. Current studies suggest that only a minority of people maintain their weight loss from the intragastric balloon over five years. Some people have repeat procedures with the balloon, and others follow up with medications or weight loss surgery for a longer-term solution.
In the ongoing pursuit of safe and effective treatments for obesity, endoscopic procedures like the intragastric balloon represent an important alternative. They offer substantial weight loss with relatively low risk. The best results come from consistent support and follow-up with a team of healthcare providers. While the balloon itself is temporary, this support can help facilitate long-term changes.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have obesity and losing weight is an uphill battle, Cleveland Clinic experts can help you decide if bariatric surgery is an option.
