Kidney stones are clusters of crystals that form from minerals and other substances in your urinary tract. Most stones pass out of your body in your pee on their own, but they can be very painful as they move through. You might need a procedure to break up or remove the stone if it can’t pass on its own or is causing a blockage.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
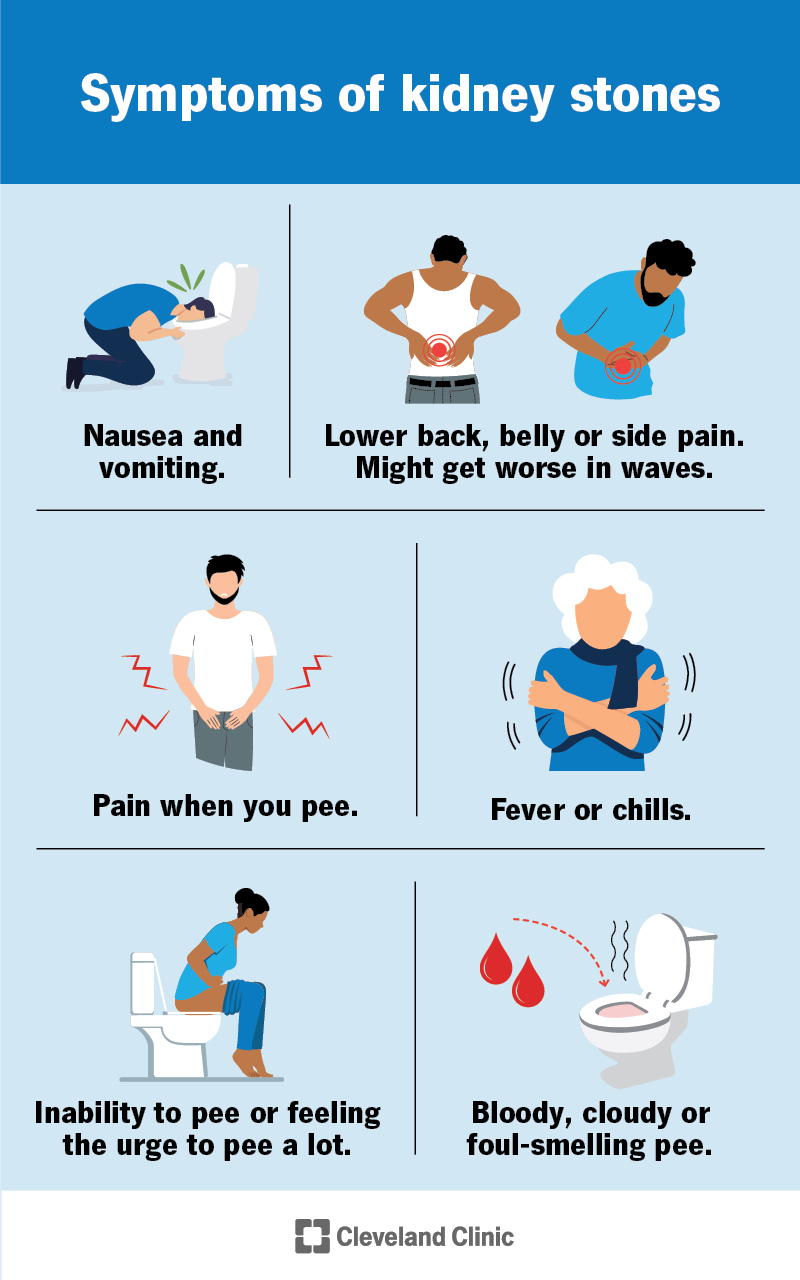
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15604-kidney-stone)
Kidney stones are solid masses or crystals that form from substances (like minerals, acids and salts) in your kidneys. They can be as small as a grain of sand or — rarely — larger than a golf ball. Kidney stones are also called renal calculi or nephrolithiasis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Depending on the size of your kidney stone (or stones), you may not even realize that you have one. Smaller stones can pass through your urinary tract in your pee with no symptoms. Large kidney stones can get trapped in your ureter (the tube that drains urine from your kidney down to your bladder). This can cause pee to back up and limit your kidney’s ability to filter waste from your body. It can also cause bleeding.
It can take as long as three weeks for kidney stones to pass on their own. Even some small stones can cause extreme pain as they go through your urinary tract and out of your body. You may need a provider to break up and remove a stone that can’t pass on its own.
About 1 in 10 people will get a kidney stone during their lifetime. They’re most common in men in their 30s and 40s. They’re also more common among non-Hispanic white people.
The most common symptom of kidney stones is pain in your lower back, belly or side (flank pain). It might feel like it extends from your groin to your side. It can be a dull pain or sharp and severe. It’s sometimes called colicky pain because it can get worse in waves.
Other kidney stone symptoms include:
Advertisement
Smaller kidney stones may not cause pain or other symptoms.
Your pee contains minerals, acids and other substances, like calcium, sodium, oxalate and uric acid. When you have too many particles of these substances in your pee and too little liquid, they can start to stick together, forming crystals or stones. Kidney stones can form over months or years.
Stones are named for the type of crystals they’re made up of:
You might be at a higher risk of developing kidney stones if you:
Certain health conditions can put you at a higher risk for kidney stones. These include:
Kidney stones can put you at risk for:
Healthcare providers use imaging, blood and urine (pee) tests to diagnose kidney stones. If your provider suspects you have a kidney stone based on your symptoms and physical exam, you may need one or more of these tests:
Advertisement
Video playlist content: This video playlist is available to watch online.
View video playlist online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_wd2jyjn5/flavorId/1_5f3sgelj/format/applehttp/protocol/https/a.mp4)
Kidney stone treatment options
If you have a small stone that’s likely to pass on its own, your provider will have you monitor your symptoms until it passes in your pee. They might prescribe medications that keep you comfortable and help the stone pass on its own.
Larger stones need treatment depending on their size, location, whether they’re causing infections or symptoms, and other factors. If you have a large stone or a blockage, or if a stone isn’t passing on its own in a few weeks, your provider will recommend procedures to break up or remove it.
If you have a kidney stone that can pass on its own and isn’t causing infection, a provider may prescribe or recommend medications to:
Advertisement
If you have a kidney stone that can’t pass on its own or is blocking your urinary tract, your provider will recommend a procedure to break up and/or remove the stone. The type of procedure they recommend depends on many factors, including the size and location of the stone. Kidney stone procedures include:
Advertisement
Yes, around 80% of kidney stones can pass on their own. The amount of time it takes for you to pass a kidney stone depends on its size and location. A stone that’s smaller than 4 mm (millimeters) may pass within one to two weeks. A larger stone could take about two to three weeks to completely pass. Once the stone reaches your bladder, it usually passes in a few days.
If you think you have a kidney stone, make sure a provider evaluates you to check for blockages or other complications. It’s important to follow up with your healthcare provider if you don’t pass the stone within four to six weeks.
Around 90% of small kidney stones (smaller than 6 mm) and 60% of large stones (larger than 6 mm) pass on their own. If you have a large kidney stone or one that’s blocking the flow of pee, you’ll need to have a procedure to break up and/or remove it. Sometimes, smaller stones that were expected to pass on their own can grow or move to create a blockage.
If you’ve had kidney stones, you’re likely to get more in the future. You’ll likely need to work on preventing them with changes to the foods you eat and, sometimes, medication.
If your provider thinks your kidney stone can pass on its own, you should drink plenty of water to help flush it out. Take any medications as prescribed and follow your provider’s recommendations on what to eat and drink (and what to avoid).
The things you eat and drink can impact your risk for kidney stones. Talk to your healthcare provider or dietitian about ways that you can reduce your risk. They might recommend:
Kidney stones shouldn’t stop you from going about your daily activities, or drastically reduce your quality of life. Thanks to passing them while you urinate, and thanks to treatment options, kidney stones aren’t permanent.
If you’ve had kidney stones, you’re at a higher risk for more kidney stones and chronic kidney disease.
No. Kidney stones don’t cause death.
Don’t hesitate to see your healthcare provider if you’re experiencing symptoms of kidney stones. If you have a kidney stone, you’ll need to know where it’s located and what size it is so that you can get treatment and prevent complications.
Go to the emergency department if the pain is unbearable. You may be prescribed medication for your pain and any nausea/vomiting.
You may want to ask your provider:
Kidney stones can be frustrating at best and agonizingly painful at worst. To stop your situation from getting worse, you should be evaluated by a healthcare provider as soon as possible. The pain can get severe, and surgery might be necessary. Remember: Don’t skip your prescriptions, drink lots of water and follow any dietary guidelines. Also, remember that kidney stones are a temporary condition. They won’t bother you forever.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Kidney stones can be a painful interruption in your busy life. At Cleveland Clinic, we’ll craft a treatment plan that works for you.
