A laparoscopy is a minimally invasive procedure that looks inside your stomach or pelvis. Healthcare providers use laparoscopies to diagnose medical conditions or perform surgery. Surgery using a laparoscope is called laparoscopic surgery. It’s generally safer than traditional surgery because it’s less invasive.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
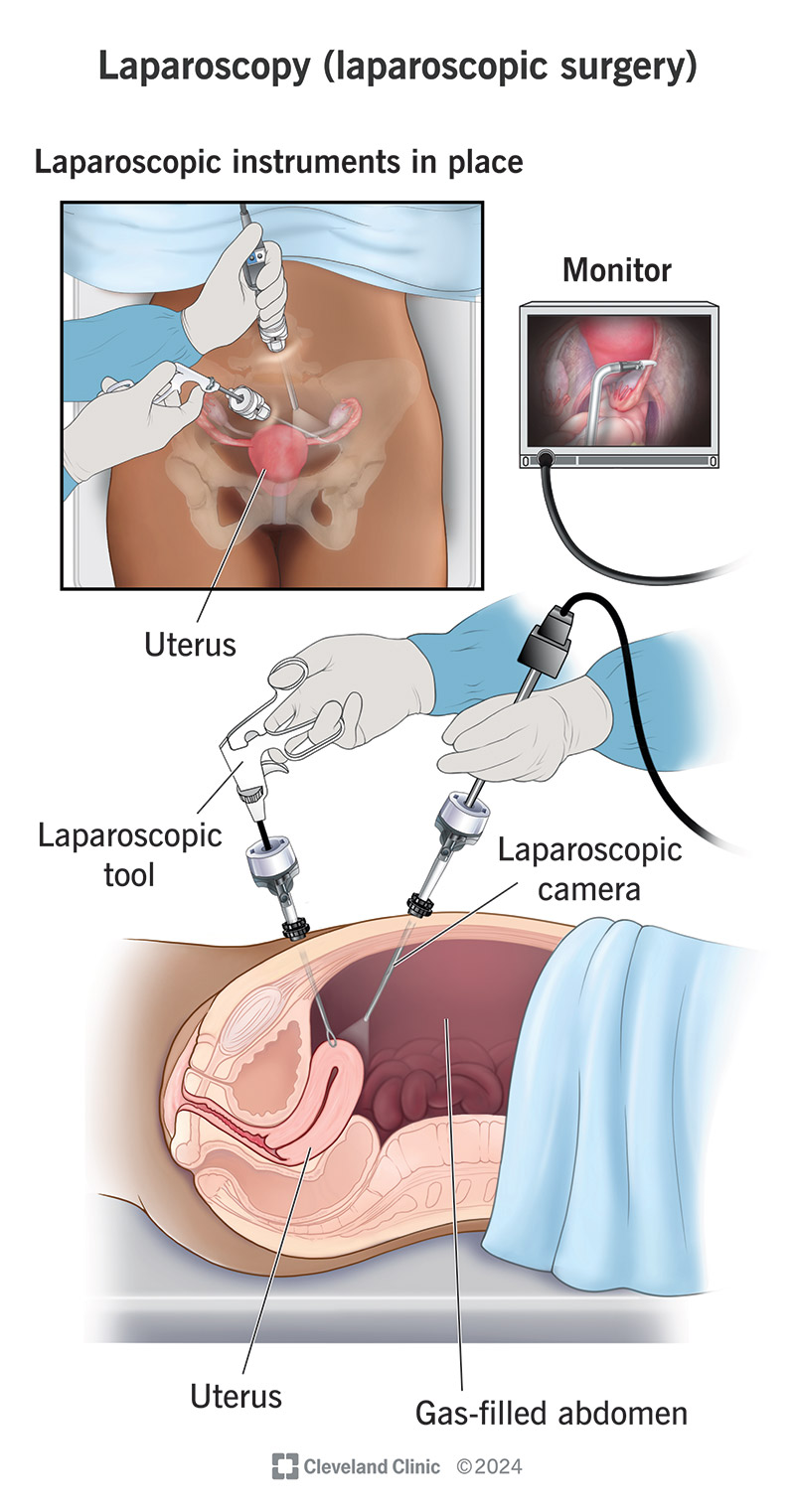
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/4819-laparoscopy.jpg)
A laparoscopy is a minimally invasive procedure your surgeon does to look for problems in your stomach or pelvic area. They use a tool called a laparoscope, which is a thin, telescopic rod with a video camera on the end. Your surgeon puts the laparoscope through a small cut (incision) in your belly (abdomen) measuring half an inch or less. Surgeons may make up to three more cuts to insert other surgical instruments so they can see all the organs in your belly and find any problems.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The laparoscope camera projects an image of the inside of your belly or pelvis onto a monitor in real time. Using these images, surgeons can watch their hand motions during the procedure.
Your healthcare provider might recommend a laparoscopy if other diagnostic tests can’t identify the cause of your condition. Healthcare providers also use laparoscopy to collect tissue samples (biopsies) for testing.
Traditional surgeries best suited for laparoscopic surgeries include:
Laparoscopy is a minimally invasive procedure, but that doesn’t always mean it’s a minor surgery. Many abdominal procedures can be done as laparoscopic surgeries, but they’re still major surgeries. Your surgeon is the best person to tell you if your procedure is a major surgery, how to prepare for it and what to expect during recovery.
Advertisement
Laparoscopic surgery is similar to a laparoscopy. But instead of looking for medical problems, your healthcare provider uses a laparoscope and surgical instruments to operate on your internal organs. People often use the terms interchangeably.
Healthcare providers use laparoscopies for many common surgeries. More complicated conditions may require traditional “open” surgery through a larger incision. But healthcare providers prefer laparoscopic surgery for a growing list of everyday operations because it costs less and improves surgical outcomes.
Follow these guidelines before the procedure or surgery:
You’ll lay on the operating table slightly tilted with your head lower than your feet. Your anesthesiologist will give you general anesthesia to relax your muscles and prevent you from feeling pain during surgery.
Your surgeon will then make a small cut near your belly button or under your rib cage. They’ll insert a gas tube into this incision to fill your belly with gas. Pumping the area with gas makes your organs easier to see on the monitor.
After removing the gas tube, your surgeon inserts the laparoscope. They may insert surgical instruments through incisions nearby to take tissue samples or perform surgical procedures.
Your surgeon will let the gas out of your body once the procedure is over and close your incisions.
A diagnostic laparoscopy usually takes from 30 minutes to one hour. Laparoscopic surgery can take from one to three hours, depending on how complicated your condition is. If the surgeon can’t safely complete the operation using laparoscopically, they may need to switch to a traditional open procedure with a larger incision.
After surgery, you’ll usually stay in a recovery room for about one hour while providers monitor your vital signs until you wake up.
You may have pain after surgery from small amounts of gas left in your body, as well as internal pain from the surgery or around your incisions. It’s also common to have shoulder pain. Your provider will give you pain medication to make you more comfortable.
Advertisement
Before leaving the hospital, schedule your follow-up appointment so your healthcare provider can check your healing progress.
The advantages of having laparoscopic surgery include:
Laparoscopy is a very safe procedure. But healthcare providers still consider it a major surgery. Possible complications include:
After you get home from laparoscopic surgery, you’ll want to take it easy for at least a day or two. You should follow these steps:
Advertisement
You can usually return to work three days after surgery, but check with your healthcare provider to be sure. If you need a doctor’s letter excusing you from work, please ask for one at your preoperative appointment.
Usually, you can start exercising again about a week after laparoscopy. But the type of surgery you have will also make a difference. Check with your healthcare provider to be sure.
When you can start having sex after laparoscopy depends on the type of laparoscopic procedure you have. It’s always best to check with your healthcare provider first.
Call your healthcare provider right away if you have any of these symptoms:
One of the best things about laparoscopy is that it allows your healthcare providers to see what’s happening inside your body without opening you up. They can do a lot through those tiny holes, but they can’t do everything. Sometimes, they might find something that requires a larger procedure. But most of the time, your surgeon can treat your issues using this minimally invasive procedure.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Sometimes you have surgery planned. Other times, it’s an emergency. No matter how you end up in the OR, Cleveland Clinic’s general surgery team is here for you.
